This poster is published under an
open license. Please read the
disclaimer for further details.
Keywords:
Ear / Nose / Throat, Interventional vascular, Head and neck, Catheter arteriography, Embolisation, Neoplasia
Authors:
T. Amer, A. Elmokadem, A. M. AbdEl-khalek; Mansoura/EG
DOI:
10.1594/ecr2016/C-0329
Results
Clinical data:
This study included 20 male patients (mean age ± SD: 14.6 ± 7.2 years) with Juvenile angiofibroma and intracranial extensions.
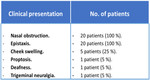
The different clinical presentation is outlined in table (1).
Tumor extension and staging:
Tumor staging was determined by review of the physical examination and imaging studies including CT and MRI for all patients.
Extension of tumor into the middle cranial fossa was seen in 19 patients (95 %) [Right side in 11 (55 %) and left side in 8 (40 %)],
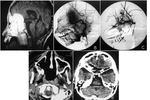
while tumor extension to the anterior cranial fossa (figure 1) was seen only in one patient (about 5%).
The tumors were classified according to Fisch classification to Stage IVa in 17 patients (85%) and stage IVb in 3 patients (15%).
Blood supply to the tumor:
Blood supply to the tumor was the internal maxillary artery (IMA) in all patients.
Bilateral supply was found in 4 patients (20 %) and unilateral supply in 16 patients (80 %).
Complication of embolization:
The technique of IMA embolization is a relatively safe technique.
No procedure related mortality in our group.
Minor complications were seen nearly in all patients except one patient who had a major complication in the form temporary visual loss due to embolization of aberrant left ophthalmic artery which was arising abnormally from the left middle meningeal artery.
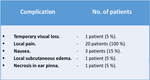
The embolization complications are listed in tables (2).
Operative results and tumor recurrence:
The average amount loss calculated during the surgery was 650 ml and the average amount of blood transfusion was 944.4 ml.
Most of the blood loss was from skin incision in the highly vascular scalp and face and not from the embolized tumor,
according to the data available from the surgeons.
Complete tumor resection with no recurrence was seen in 15 patients (75 %) as evidenced by post contrast CT and MRI,
while tumor recurrence was seen in 5 patients (25 %) after a period ranging from 1 to 3 years.
Extra-cranial recurrence was seen in 2 patients (10 %),
they were embolized and reoperated again,
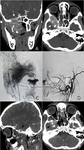
while intra-cranial recurrence was seen in 3 patients (15 %) (figure 2),
one of them was embolized and re-operated and for the other two nothing was done apart from short interval follow up which show spontaneous regression over time.
The surgical complications are listed in tables (3).