Most of the misdiagnoses occur by a combination of factors in the radiological process.
Part of our work as radiologists is to detect and analyse their causes.
Our poster is focused on common diagnostic errors.
A diagnostic error consists in the omission or incorrect interpretation of a radiological finding [1].
The most common radiological error in spine is the omission of fractures.
It is considered the main cause of legal action against radiologists,
after failing to detect breast and lung cancer [2].
Since the publication of the article "To err is human" in the year 1999 with the alarming fact that up to 100,000 people a year were dying by medical errors [3] the degree of vigilance towards errors has grown.
In the United States of America a third of all radiologists are sued and at the same time a third of these are accused of medical malpractice [1].
A third of these demands are due to errors in the spine,
most frequently the cervical spine (68%) with an average of nearly half a million dollars compensation [4].
Not only the patients' health,
but also their sick leaves and economic compensations depend on thousands of spine reports issued every year.
Therefore,
it is our responsibility to know why errors occur and how to detect them to avoid making the same mistakes in the future.
The reduction of errors has a positive impact on the health of the patient,
healthcare costs and also the radiologist.
Concept,
frequency and importance of the diagnostic error
In Radiology a diagnostic error is considered as the incorrect interpretation of the images,
regardless of whether this causes harm to the patient or not [5].
The prevalence of the error ranges from 3% to 30%,
depending on the series and criteria that are analysed [2,
6,
7].
Unlike a simple error,
negligence occurs when an incorrect interpretation exceeds an acceptable limit (by imprudence or inexperience) and causes damage to the patient [8].
It is estimated that up to 20% of the radiological errors are clinically relevant or correspond to one greater diagnostic error [9].
It is important to convince the doctors,
managers and judges that radiological errors are biased by the belief that perfection and infallibility can be required to the radiologist,
when in fact the standard pattern of assistance and perfection are not synonymous [8,
10-14].
The practice of the radiologist should be judged according to whether the diagnostic process is correct,
not only according to the diagnostic or therapeutic outcome [5,
8,
15].
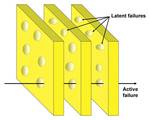
Errors are classified as active and latent.
Active errors are those committed by radiologists on their own.
They happen when a diagnosis is omitted or incorrect,
when follow-up or other imaging tests are not recommended,
or by inefficient communication of critical or unexpected findings to the requester of the study [16].
Latent errors are those arising from the system and involved in the whole radiological process since the moment the patient comes to the radiology department,
to the point the medical requester receives the radiological report.
They include for example defects in equipment,
scheduling,
organization issues,
PACS system,
workloads,
work environment or internal policies of the service [2,
16,
17].
Up to 90% of medical errors stem from a combination of these factors [13,16].
Here is the importance of identifying latent errors,
their correction is likely to create a greater positive impact in terms of quality of care (table 1).
To explain the errors and accidents the English psychologist Reason described a theory based on the model of the Swiss cheese (Fig.
1-3),
which argues that to make an active error that causes harm,
several latent errors must occur simultaneously [16].
|
Table 1.
Latent errors or System errors
|
|
Category
|
Issues,
examples,
situations
|
|
Equipment,
design,
and maintenance
|
Availability,
functioning,
and maintenance of machines,
design of the work environment,
ergonometry,
hygiene and cleaning,
interruptions,
ambient noise,
PACS
|
|
Staffing
|
Staff with proper skills,
adequate staffing for workload
|
|
Comunication
|
Work-direct communication,
openness,
interrelation,
work atmosphere
|
|
Training
|
Training for new equiptment,
procedures,
team training,
continuing medical education,
resident supervision
|
|
Procedures
|
Existence of protocols,
adherence to protocols,
management of errors,
informed consent,
quality control,
double-reading
|
|
Planning and organization
|
Team performance,
labour distribution,
work goals,
workload,
work hours,
imaging management,
patient safety,
list of tasks,
future developments,
balance between goals and safety
|