Spectrum of diagnostic errors in the vertebral spine
Radiology depends essentially on the identification and interpretation of visual findings,
thus perception biases and cognitive have a more important role than in other areas [11].
While the training can improve the diagnostic radiologist threshold,
some of these processes are not always subject to conscious control by the human mind [7].
Errors of perception:
They consist of the omission of a finding that is present in the image [2,
8,
18].
They are the most common (80%) and constitute the first cause of lawsuit in Radiology [2].
In general,
they are triggered off by other factors,
e.g.
the poor quality of the images,
equivocal or insufficient clinical information,
the level of alert of the observer,
eyestrain,
distracting factors,
the degree of visibility (evidence) of the alteration,
lack of review of previous studies,
etc.
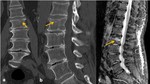
Retrospective error is frequent in these situations (Fig.
4) or tendency to wrongly believe after knowing the diagnosis that the injury would have identified [8,
10].
Omission error:
It is to ignore a finding despite having kept the eyes on this anatomical area [2].
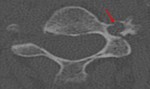
Some common spine omissions are sacral fractures,
hernias,
spondylolysis,
and transverse process fractures (Figs.
5-11).
Injuries located in peripheral areas or outside the field of interest,
injuries visible in few slices or unexpected incidental findings can explain these errors.
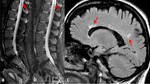
Satisfaction of search error (SOS)
It occurs when once detected an injury the radiologist prematurely ends the search,
omitting other relevant findings (Figs.
12-14) [2,
11,
16].
To avoid these errors the radiologist should always perform a systematic analysis of the study and a secondary search.
It should also be aware of lesions that often arise in association and do a conscious search for both these findings,
and any other incidental ones.
Cognitive errors
In these cases the anomaly is detected but interpreted in the wrong way.
Cognitive errors include a misperception,
failed heuristic or biases of cognition.
Cognition biases relate to psychological distortions that lead to a poor critical judgment [7] patterns.
Framing bias (Induction error or bias of conditioning)
This error occurs when the radiologist is influenced by the way a clinical problem is outlined (Fig.
15) [11].
It can be prevented by analysing the study before reading the clinical information or by requesting additional clinical information in the face of unexpected image findings.
Availability bias
It is the tendency to consider first a diagnosis that is familiar and prevailing in the mind for any particular reason.
For example,
a radiologist who is sued for having omitted a pathological fracture is likely that tends to consider a possible tumoral origin more frequently in his diagnoses [5] than other colleagues. To avoid them you can get objective information about the real prevalence and likelihood of the diagnosis and compare the rate of similar diagnoses in the team of radiologists of your health centre [7].
False positive error or over-reading
It happens when non-pathological radiological findings are wrongly interpreted as disease.
It can occur with anatomic variants,
normal post-surgical findings or image artifacts [7,
19-22].
They are usually due to insufficient academic knowledge and indicate lack of experience.
They are most frequent in young residents or radiologists.
(Figs.
16-20).
Continuing medical education and the consultation with other colleagues have been shown to reduce these errors [17].
False negative error or underreading
It is the tendency to not associate a pathologic significance with the radiological images.
They might be caused by fear to overdiagnose simple or incidental findings or pressure from the administration to reduce expenses by false positives [2].
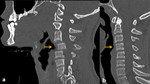
Premature closure error
It is the tendency to assume a diagnosis without a full verification.
This error is illustrated in Figure 21,
which corresponds to a 25 year old patient with a cervical trauma and a wrong diagnosis of epidural hematoma instead of cervical disc herniation [20]. It is advisable to assess differential diagnoses with reasonable alternatives; never convert an inconclusive diagnosis into a definitive one without clinical correlation and/or complementary additional tests if they were necessary [7].
The radiologist should express the degree of certainty of the diagnosis in the radiology report.
Alliterative Error
This type of error results from the influence of a former diagnosis made by another radiologist [2].
The probability that the second radiologist perpetuates this error in following reports of the same patient is high if he is not aware of the error (Figs.
13 and 21) [7,
23].
They can be avoided by analysing images,
both the present and the previous,
before reading the reports.
It is useful to search for evidence that could refute the initial diagnosis,
not only the one that can confirm it [7],
and always avoid the "copy and paste" of previous reports.
Communication errors
They are a frequent cause of lawsuit against the radiologist.
It is important to remember that the responsibility of the radiologist includes not only to make a correct diagnosis,
but also to communicate in a direct and effective way the critical,
serious and unexpected findings or modifications to reports that change the patient management [2].
Also the radiologist should suggest additional radiological procedures (Fig.
9) or follow-ups where appropriate [24,
25,
26].
Finally,
errors in the numbering of the vertebral levels,
because of anatomic variants that include transition vertebrae (Fig.
22),
floating ribs,
absent or hypoplastic vertebral bodies,
variability in the level where the medullary cone ends or inconstant insertion of ligaments in the transverse processes of L5 should be stated in the radiological report [20,
21],
due to implications in upcoming therapeutic or surgical procedures,
since misidentification would bring about an intervention in the wrong spine level.
Strategies to prevent them are simple.
Radiologist should describe the numbering scheme adopted in those cases in which the anatomy deviates from the standard pattern or use sagittal imaging of the adjacent spinal segments to get more anatomical references [24].