1 Medical Care
1 Medical Care
Cochlear implantation requires a multi-disciplinary team approach.
Patient care is composed of 3 stages: before,
during and after implant surgery.
 1.1 Preoperative Assessment and management
1.1 Preoperative Assessment and management
Preoperative CI assessment needs a multidisciplinary team approach.
The team concept allows for an exchange of information between the surgeon and other members of the implant and rehabilitation process.
The preoperative assessment,
intervention and follow-up (adjustments,
rehabilitation) must be performed by the same team.
Before surgery,
it is beneficial that the patient gets in contact with people already implanted.
 1.2 Surgical Procedure
1.2 Surgical Procedure
Cochlear implantation usually takes about 2 hours.
It is often performed on an outpatient basis,
under general anesthesia.
The facial nerve is monitored intraoperatively.
The surgical procedure consists of skin incision behind the ear and intact canal wall mastoidectomy.
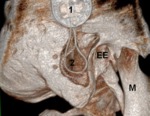
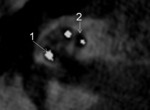
A recess is created in the skull posterior and superior to the mastoidectomy for placement and securing of the internal receiver-stimulator [1] ( Fig. 3 ).
The electrode array is inserted into the cochlea via the round window (or cochleostomy) into the tympanic scale.
 1.3 Postoperative care
1.3 Postoperative care
An average waiting period before the activation of the cochlear implant is 2-4 weeks following surgery date,
if the wound has completely healed [2].
Switch-on and tuning of the speech processor are then performed.
 2 cochlear implantation imaging
2 cochlear implantation imaging
Radiologist will assume an expanding role in evaluating affected patients as the frequency of CI continues to increase [1].
It is also imperative to be familiar with the growing number of imaging options: MRI,
CT scan and cone beam computed tomography (CBCT).
 2.1 Preoperative cochlear implantation imaging
2.1 Preoperative cochlear implantation imaging
Imaging analysis is one of the most important preoperative assessment instruments.
MRI and CT scan are required for all patients.
Role of imaging in the preoperative implantation assessment
- Help in etiological diagnosis of deafness
- Check for contraindication: The absence of the cochlea or of the cochlear nerve are the absolute contraindication of cochlear implantation
- Study of the feasibility and awareness for operational difficulties such as facial nerve dehiscence and cochlear ossification [1]
- Detect prognostic factor
- Choice of implanted side
- Choice of the electrode array length
 2.1.1 Preoperative cochlear implantation CT scan
2.1.1 Preoperative cochlear implantation CT scan
Technique
- Helical CT scan
- Submillimeter increments with a 0.5-mm overlap
- Both temporal bones - then reformation on each ear
- No contrast enhancement
- Multiplanar Reformation
Analysis
- Analysis of bilateral acquisition: Neighborhood condition requiring any prior treatment or compromising the prognosis (e.g.
sinusitis,
expansive process of the skull base)
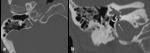
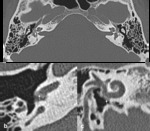
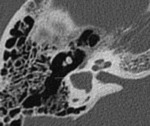
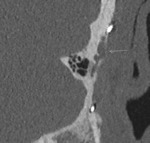
- Analysis of the mastoid: The degree of mastoïd pneumatization needs to be evaluated [3].
Dense mastoid sclerosis can potentially complicate the creation of the implant well-reservoir and limit exposure to the middle ear [1].
If the changes are asymmetric,
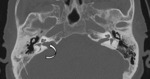
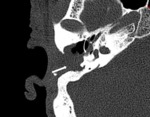
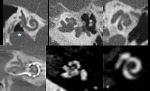
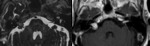
the aerated side may be chosen for implantation [1] ( Fig. 4 ). In the case of otomastoiditis,
an intact canal wall mastoidectomy may be performed prior to implantation [1] ( Fig. 5 ).
Anteriorsigmoid sinus makes mastoidectomy difficult and the other side should be chosen for surgery ( Fig. 6 ).
Any traumatic or surgical scars could affect srgery ( Fig. 7 ).
- Analysis of the middle ear: Ventilation state of the eardrum can direct the choice of side to operate.
Acute otitis media is treated prior to implantation to ovoid potential labyrinthitis or meningitis [1] ( Fig. 8 ).
A narrow tympanic cavity,
which is an insufficient development of the tympanic cavity and mastoid antrum,
may pose difficulties to the surgeon limiting the surgical field ( Fig. 9 ).
- Vascular conditions: Abnormal middle ear vascular anatomy could potentially complicate mastoidectomy and cochleostomy [1].
Vascular anomalies are often apparent clinically and are easily confirmed with MRI or CT scan [1].
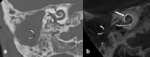
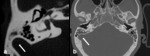
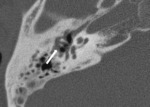
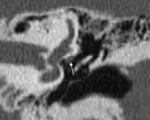
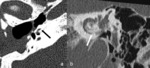
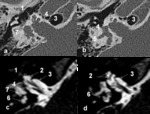
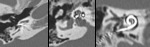
Special attention needs to be given to high-riding or diverticulum of the jugular bulb ( Fig. 10 Fig. 11 ) and aberrant carotid artery.
- Facial nerve analysis: Facial nerve compromise or paralysis resulting from cochlear implantation are rare [1].
Recognizing facial nerve dehiscence or an atypical course pre-operatively can help prevent this complication and may assist in the choice of CI side [1].
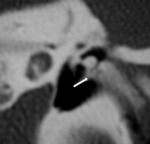
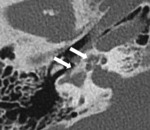
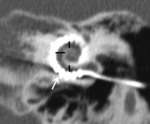
Facial nerve dehiscence is readily apparent at CT ( Fig. 12 ). An abnormal course of the mastoid segment of the facial nerve can also make the mastoidectomy difficult.
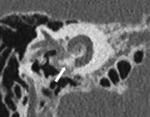
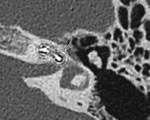
- Analysis of the round window:As the electrode array is generally inserted into the round window,
this latter should be analyzed to check,
whether there is any stenosis,
filling or ossification ( Fig. 13 Fig. 14 ).
- Analysis of the cochlea: The analysis of the cochlea is mandatory to determine the surgery approach and the electrode array choice.
It can help also to detect the etiology of deafness such as cochlear partition anomalies (common cavity,
Mondini dysplasia).
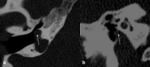
Cochlear ossification with luminal obstruction is not a contraindication for implantation but is important to be identified preoperatively as it makes the cochleostomy more challenging [1] ( Fig. 15 ).
Ossification is especially important to check if the patient has a history of meningitis.
Retrofenestral otosclerosis is also not a contraindication for CI [1].
However,
it is mandatory to detect this condition preoperatively,
mainly for two reasons.
At first,
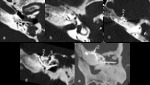
it causes a cochlear wall fragility and could lead to misplacement of the electrode array especially in the cystic focus of otosclerosis ( Fig. 16 Fig. 17 Fig. 18 ).
Second,
facial nerve stimulation in CI is more common in patients with otosclerosis and is likely related to conduction of current through otospongiotic bone (corrected by programming out the electrodes causing the stimulation) [1].
The osteogenesis imperfecta is a rare cause of deafness.
CT and MRI findings do not differ from those seen in patient with combined fenestral and retrofenestral otosclerosis with osteopenic appearance of the bony labyrinth ( Fig. 19 ).
The risk of cerebrospinal fluid (CFS) gusher is significantly increased in the presence of bulbous,
dilated distal IAC,
often associated with absence of the bone partition that separates the distal canal and the base of the cochlea [1] ( Fig. 20 ).
The potential for a gusher to occur during cochleostomy does not preclude implantation [1].
Management of CSF gusher can be mainly performed during the initial surgery by precise tight packing of the electrode entrance.
Generally a silicone ring is used for hermetic insertion of the electrode through the cochleostomy instead of the classic packing of the fascia and soft tissue around the electrode array.
Some new electrodes with "cork" stopper look promising in preventing the postoperative CSF leak around the electrode. To ovoid array misplacement through the deficient modiolus into the IAC,
a short ring shaped electrode should be used.
- Cochlear length measurement: Cochlear duct length (CDL) is the scala tympani length measured at the organ of Corti corresponding to the complete and tow-turn CDL.
It is measured from the middle of the round window to the helicotrema [4,
5].
It can vary between 25 and 35 mm,
with a variation by 40% between shortest and longest cochlea [4].
CDL measurement helps choosing the length of the array electrode.
Indeed,
it is thought that selecting an electrode array length adapted to each individual’s cochlear anatomy may reduce frequency-place mismatch and thus improve speech perception outcome [6].
We use two methods for CDL measurement: manual measurement and calculated from the distance “A”.
The CDL manual measurement is based on multiplanar reconstruction (MPR).
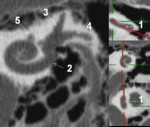
A coronal oblique reconstruction is performed in a plane passing through the basal turn of the cochlea,
the round window and the upper semicircular canal ( Fig. 21 ).
The cochlea is then measured with the curved measurement tool along its outer wall,
from the round window to the apex ( Fig. 22 ).
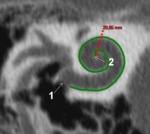
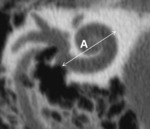
The CDL calculated from the linear distance of “A”,
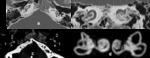
“A” (in mm) is the distance between the center of the round window and the farthest point on the opposite wall of the cochlea on a reformatted CT scan slice described above [7] ( Fig. 23 ).
The equation for estimation of complete CDL is : CDL (oc)= 4.16A-4 and for CDL(i)=4.16 A-2.7 ,
with “OC” organ of Corti and “i” represents the implantable CDL of the cochlear implant [5].
The measure is only valid for normal cochlea.
The average length of A = 8.431 +/- 0.525 mm.
Some manufactures have an application allowing a direct calculating of CDL from the “A” distance.
- Analysis of the posterior bony labyrinth: CT scan readily depicts the enlarged vestibular aqueduct [1].
The posterior labyrinth can show ossification,
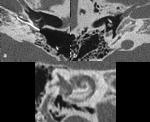
malformation ( Fig. 24 ) or a superior semicircular canal dehiscence,
which could result in some hearing disorders.
The CT scans demonstrate the opening in the bone that should cover the superior canal.
However,
CT imaging can miss a thin layer of intact bone overlying the canal with false positive results ( Fig. 25 ).
CBCT seems superior in these cases.
 2.1.2 Preoperative cochlear implantation MRI
2.1.2 Preoperative cochlear implantation MRI
Technique
- Conventional brain MR imaging: Axial FLAIR,
Diffusion,
axial T2 *,
coronal T2 and 3D T1-weighted sequences.
- Analysis of IAC and membranous labyrinth: thin-slice sequences (0.7 mm) 3D steady state sequences (CISS,
FIESTA,
and DRIVE).
CISS is a 3D gradient-echo pulse sequence that allows reduced sensitivity to susceptibility changes and flow while retaining the bright fluid signal intensity achievable with true fast imaging with steyady-state precession (FISP) [1].
High-resolution heavily T2-weighted techniques allow very good delineation nerves in the CSF and membranous labyrinth.
- 3D reconstructions with maximum intensity projection image (MIP) allow an anatomical presentation of the membranous labyrinth.
Objectives
- Help in etiological diagnosis of deafness
- Check for contraindication especially the cochlear nerve absence.
- The brain MRI sequences help to detect any disease causing an uncertain functional prognosis implantation or requiring specific management.
Indeed,
MRI after CI is only possible respecting safety recommendations and guidelines.
CI generates also artifacts which can alter the quality of the images particularly when the abnormalities to explore are ipsilateral to the implant.
- Check in the hearing tracts and nuclei: implantation should not be performed on the ipsilateral side in a patient with a brainstem disorder such as infarct involving the cochlear nuclei that leads to unilateral sensorineural hearing loss [1].
- Help to make a cognitive assessment in the elderly
Analysis
- Analysis of membranous labyrinth: A normal membranous labyrinth shows a hypersignal in 3D steady state sequences.On 3D reconstructions the cochlea,
the vestibule and the three semicircular canals are always completely visible.
The fluid signal loose of the membranous labyrinth can be caused by sclerosis,
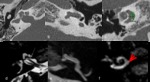
ossification or tumor developed within the fluid spaces ( Fig. 26 ).
Labyrinthitis and labyrinth hemorrhage can also result in replacement of the normal bright endolymphatic signal intensity ( Fig. 27 ).
MRI assesses also the labyrinth morphology and helps to diagnose malformations.
The cochlear segmentation,
the modiolus and the interscalar septa are well assessed.
Generated MIP images improve the evaluation of the cochlea [1].
The endolymphatic sac and duct enlargement and semicircular canals malformations are easily diagnosed ( Fig. 28 ).
The semicircular canals must be completely visible.
Any amputation is pathologic and can be related to malformation,
ossification or sclerosis.
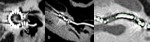
- Analysis of the cochlear nerve and IAC content: The cochlear nerve is best seen on oblique sagittal MPR images perpendicular to the plane of the internal auditory canal (IAC) [1].
It is seen in the anteroinferior quadrant of the canal.
It is the larger nerve (> 0,8mm) and have at least the same size as the facial nerve ( Fig. 29 Fig. 30 ).
Contrast material-enhanced axial T1-weighted MR MRI with T1 contrast (gadolinium) helps to diagnose the acoustic neuromas (also known as schwannomas) ( Fig. 31 ).
 2.1.3 Preoperative cochlear implantation CT scan and MRI
2.1.3 Preoperative cochlear implantation CT scan and MRI
After systematic confrontation between CT scan and MRI,
the radiologist should be able to answer those questions :
- Is the cochlea normal? And is the tympanic scale patent especially in retrofenestral otosclerosis and labyrinthine ossification? ( Fig. 32 ).
- Are there any imaging findings that contraindicate implantation?: absence of the cochlea or absence of the cochlear nerve
- Are there any imaging findings that could significantly alter surgery? : facial nerve dehiscence,
cochlear ossification,
some vascular conditions (high ridding of the jugular bulb and carotid aberrant course) and cochlear malformation with risk of CSF gusher.
- Are there any conditions that necessitate treatment or management before implantation or lead to choose the side to implant? Acute otitis and acute labyrinthitis should be treated prior to implantation to avoid postoperative infectious and hemorrhagic complications.
- Are there any central nervous system disorders? CI should not be performed on the ipsilateral side in a patient with pathology involving the auditory pathways in brain that leads to unilateral sensorineural hearing loss [1].
If a central nervous disease is detected,
the medical staff evaluates the MRI control possibilities regarding artifacts.
- What is the cochlear length?
All patient candidacies for cochlear implantation are discussed during the staff meeting and in few cases imaging findings raise additional questions and would not lead to evident decision ( Fig. 33 ).
 2.2 Post-operative cochlear implantation imaging
2.2 Post-operative cochlear implantation imaging
 2.1.1 Imaging Purpose:
2.1.1 Imaging Purpose:
Cochlear implants can restore speech recognition,
but variability in outcomes remains a constant feature especially in post-lingually defened adults [8].
Among factors accounting for this variability,
duration of deafness is probably the most critical one [8].
More recently,
scalar localization of the electrode array has been suggested to influence the hearing performance [8].
Intracochlear position of the cochlear implant has been identified as a contributor in functional outcomes [8].
Radiological tools must be accurate enough to determine the final placement of the electrode array [8].
Imaging purposes
- Check the electrode holder position which should be in scala tympani and not translocated into scala vestibuli through ruptures and factures of the structures separating the scalae [7].
Scala tympani is the optimal place for electrode array insertion,
as terminal sensorineural structures and spiral ganglia are more likely to be damaged in a scala vestibuli placement [8,9]
- Verify if the implant is correctly positioned with maximal insertion depth and regular route through the cochlea [10].
The depth of insertion can be measured as degrees of angular rotation within the cochlea [10]
- The appearance and position relating to the modiolus depend on the type of cochlear implant
- Postoperative imaging serves as reference imaging in case of subsequent performance loss.
- Detect the electrode proximal to the facial nerve in the case of facial stimulation
- Detect complications in the recess for placement and securing of the internal receiver-stimulator and in the mastoidectomy cavity
Technique
The postoperative assessment consisted of a simple radiograph: Stenver's incidence and/or CT scan.
Today CBCT generating less artifacts and radiations than the CT scan,
is the modality of choice to verify the correct positioning of the electrode into the scala tympani.
Currently all our implanted patients benefit from post-operative CBCT.
 2.1.2 Standard radiography “Stenver’s view”
2.1.2 Standard radiography “Stenver’s view”
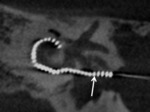
Conventional radiography allows early confirmation of correct placement of the array and detection of kinking or bending,
but does not allow the visualization of anatomic relationship with the inner ear [10].
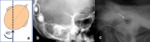
This method offers information about the position of the device within the petrous bone.
Positioning within the cochlea is approximately indirectly educible from the configuration of the electrode ( Fig. 34 ).
Additionally,
buckling of the electrode may be visible.
In more complex cases,
a more detailed view of the electrode is eligible.
In these cases,
conventional CT scans or CBCT offer additional information of the electrode positioning within the cochlea [11].
 2.1.3 Postoperative CT scan
2.1.3 Postoperative CT scan
Analysis
- Mastoïdectomy cavity: to detect any complication such as madtoiditis
- Recess for placement and securing of the internal receiver-stimulator: to detect any bone apposition ( Fig. 35 ).
- Positioning of the electrode holder in the scala tympani and verification of all individual electrode contacts : High-resolution CT scan (HRCT) provides excellent definition of the fine osseous structures of the temporal bone,
allowing precise assessment of the intracochlear position and insertion depth of the electrode array,
together with the visualization of each individual electrode contact [8] ( Fig. 36 Fig. 37 ).
Lecerf et al.
validated HRCT midmodiolar reconstructions showing a high radio anatomic concordance after microdisscetion of implanted temporal bone [12].
- How to recognize the scala position of electrode array? Where the electrode array remained in the inferior part of the basal turn,
we inferred scala tympani localization [8].
Diagnosis of dislocation from scala tympani to scala vestibule relied on the visualization of the change in trajectory of the electrode array,
and on the identification of the implant in the inferior part of the basal turn for its proximal portion (scala tympani) and in the superior part of the basal turn for its distal tip (scala vestibuli) [8].
The ascending part of the basal turn,
i.e.
pars ascenders seems to be the most vulnerable region for translocation [8].
This vulnerability is probably related to the constant narrowing of the scala tympani in this area,
with an average reduction of 300 μm in its diameter between 90° and 180° [8].
( Fig. 38 Fig. 39 ).
- Additional identification of single electrodes is possible in all implants of Medel and Advanced Bionics Companies [11].
Identification was not always possible in Cochlear Nucleus implants due to artifacts produced by narrower distances between electrodes.
Depending on implant type,
electrode array insertion could apparently be identified as next to modiolus or far from modiolus [11] ( Fig. 40 Fig. 41 ).
- Identification of the causing electrode for facial nerve stimulation is possible with CT scan.
This problem is usually corrected by programming out the electrodes causing the stimulation [1].
- Incomplete electrode array insertion with electrode contacts in middle ear and aberrant extracochlear course of electrode array are also clearly visible in CT scans ( Fig. 42 ).
Limits
- CT scans are radiating and often affected by artifacts due to electrode and generator [11] ( Fig. 43 ).
- Difficulty of assessing the correct position of deeply inserted intracochlear electrodes: Scalar localization of deeply inserted electrode carriers cannot be precisely determined by means of CT scans [13]
 2.1.4 Post operative CBCT
2.1.4 Post operative CBCT
As mentioned previously,
dislocation from scala to the other can result in major structural damage [9].
Tympanic scale insertions for intracochlear positioning of the implant are advantageous with regard to speech performance results [14].
Thus postoperative imaging should be able to evaluate precise electrode location [14].
CBCT uses reduced radiation while preserving a detailed view of electrode position within the inner ear [9].
An atraumatic insertion technique is of particular importance with regard to the increasing indications (e.g.
hearing preservation implantation) for cochlea implantation [14].
CBCT enables the assessment of intracochlear trauma in terms of misplacement of the electrode in the vestibular scale or a dislocation between the scales.
Penetration of the basilar membrane damages the Organ of Corti and induces a loss of sensory cells [14].
Technique
- Patient must keep the head in a fixed position.
- The Region of Interest (ROI) is marked by target light beams that can be arbitrarily positioned
- An emitter-detector unit rotates around the patient’s head
- Sub-millimetric spatial resolution (0.2 mm isotropic voxels) is acquired with multiplanar reconstructions in three plains: coronal,
axial and sagittal [14]
Analysis
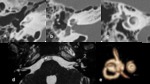
- The cochlear implant is presented as a limited metallic artifact with aeric hypodensity that surrounds the electrode array [8] ( Fig. 44 ).
- CBCT has been demonstrated to be a reliable tool to assess scalar localization of the electrode array [8].
The ability to determine the exact position of the electrodes by CBCT compared with histologic sections was demonstrated by Kurzweg et al [8].
( Fig. 45 )
- Similarly to the CT scan,
midmodiolar reconstruction in CBCT can show the translocation as modification from inferior part of half turn section to superior part in next half turn section by mean of mid modiolar and pars ascendens reconstructions [8].
Uncurling of the cochlea in one plane based on the raw data acquired,
performed in the Curved-MPR Mode can also be used to determine and approve the exact position of the electrode in the cochlea [14].
3 positions of the CI are possible: the inferior position of the electrode is typical for an insertion into the tympanic scale,
the superior position for vestibular scale and the dislocation between the scales can be assumed because of the change from the inferior to the superior position in the curled-up cochlea [14].
- CBCT allows recognizing the exact position of the electrode in which in ramp (92%) [14].
- Like in CT scans the feature of the electrode array in CBCT depends on the electrode type and additional identification of single electrodes is often possible ( Fig. 46 Fig. 47 ).
- A deeply inserted implant is efficiently detected with CBCT ( Fig. 48 ).
- Electrode misplacement include tip-over,
loop,
kinking,
scalar transition,
and incomplete insertion ( Fig. 49 Fig. 50 Fig. 51 )[15].
CBCT vs.
scanner
- Low radiation and metal artifact,
high resolution and low cost on CBCT instruments are considering choices in post-operative cochlear implantation [8,14].
- The CBCT radiation dose may be 8-22 times lower than HRCT scan [8].
- Aschendorff et al.
have shown that postoperative CBCT images of the type Cochlear implants ® were superior to CT scan images
Limits
- Cone beam CT image quality is possibly reduced by patient movement (swallowing) and shows signs of movement artifact during the acquisition.
In order to attempt retakes reduction,
patients can be immobilized using a head strap and don’t swallow.
Elderly were more likely to move during scan acquisition.
- Some metal artifacts are seen in images acquired with CBCT dedicated to dental examination ( Fig. 51 ).
Better results are obtained when using a CBCT dedicated to temporal bone examination with patient lying.
- Poor soft tissue contrast.
- Does not detect a rupture of the basilar membrane without translocation
- CBCT imaging is able to provide a good indication of the scalar position of implanted electrodes,
although estimation may be slightly less reliable for apical electrodes and for straight electrode designs [16]
Perspective
Some studies have evaluated the feasibility of using CBCT technique in combination with (high resolution) MRI to identify electrode movements following cochlear implant surgery and identify the inter-scalar position of the electrode [17].
 2.1.5 Cochlear implantation and MRI
2.1.5 Cochlear implantation and MRI
For many years patients with CI could not undergo MRI examinations [18].
However in the last 15 years,
several studies by different research teams and manufacturers have shown no major incidents in MRI examinations using magnetic field strengths up to 1.5T [15].
Several authors concluded that MRI scans up to 1.5T are safe in patients carrying CIs with non-removable magnets,
if strict guidelines are followed [15].
Patients receiving a CI might have three major disadvantages regarding magnetic resonance (MR) imaging:
- The magnetic receiver coil under the skin might cause pain during the acquisition of the MR images
- Dislocation of the implant is possible
- The internal magnet creates large artifacts that limit the diagnostic validity ( Fig. 53 ).
Key points
- Current contraindications 3T MRI (ongoing studies for removable magnet implants)
- Possible MRI in patients with cochlear implant up to 1.5T
- Consult the manufacturer’s instructions before performing MRI : manufacturer’s agreement is required
- Strict adherence to safety recommendations and guidelines
- Prior medical consultation
- Patient with mechanically damaged implants must not undergo MRI
- Risk of interaction between the magnet and ferromagnetic element (twisting under the skin) 1.5 Teslas,
and damage to the implant (for magnetic fields below 1.5 Tesla)
- Artifacts related to the ferromagnetic material of the implant
Surgical required information
- Appropriate fixation of the implant
- Information about the mastoid recess and the method of attachment
- A minimum thickness of the bone underneath the implant magnet of 0.4 mm is required (in an MRI scanner torque forces act on the implant magnet,
exerting rotational pressure: the device will try to turn to line up with force lines.
The resulting forces on the edges of the implant are counterbalanced by the cranial bone and the skin flap.
Bone underneath the implant magnet should be thick enough to withstand these exerting forces.)
- MRI scan not to be performed earlier than 6 months post implantation (performing an MRI at an earlier stage may result in implant displacement and/or damage to the implant).
- The exact type of implant must be verified with the surgical history [1]
MRI precautions
- The MRI imaging compatibility of the implant must then be ascertained from the manufacturer [1]
- All external components of the implant system must be removed
- A supportive head bandage must be placed over the implant: The internal hardware may be left in place,
maintained by an external restraint (For the 3 major manufacturers of cochlear implantation placed in Europe)
- Strict instructions on positioning of the head in the magnet and in the area of 30 cm before entering the tunnel: the longitudinal axis of the head must be parallel to the main magnetic field of the scanner (The patient should not turn or bend his/her head to the side; otherwise partial demagnetization of the implant magnet is possible.)
- Sometimes surgical removal is necessary or demagnetization of the internal magnet of the implant before MRI
- Implants made from nonmagnetic and nonconducting materials are MR Safe [19].
- Finally,
removal of the magnet should be verified [1]
MRI and CI with Removable Magnet
- About 10% of cochlear carriers in developed countries can be expected to undergo MRI within their lifetimes [18].
- MR imaging in CI patients also raises concerns regarding MRI-induced artifacts caused by the implant [18].
- Artifacts are induced by both the metallic parts of the CI and the magnet inside the implant.
- One solution to reduce artifacts and to increase patient safety was the use of implants with removable magnets [18],
which reduces implant torque and the risk of demagnetization during MR scans.
The implant also offers the possibility of removing the magnet in case of large imaging artifact.
- Some MR sequences are more exposed to CI magnet-induced field distortions and consequent more pronounced artifacts [18].
In particular,
the 3D CISS and the T1w MPR enlarge artifacts [18].