Ankylosing spondylitis (AS) is a chronic autoimmune spondyloarthopathy mainly affecting the axial skeleton [1].
The ankylosed spine is prone to fracture even after a minor trauma and patients with AS have a fourfold vertebral fracture risk during their lifetime compared to healthy individuals [2,
3].
A delay in diagnosis often occurs due to both patient and doctor related factors.
Even in the presence of symptomatic clinical vertebral fractures,
patients frequently fail to differentiate acute fracture-type pain from preexisting inflammatory pain,
so the diagnosis is often overruled by attributing the pain to disease activity [4,
5] (Fig. 1).
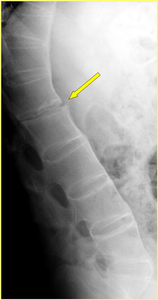
Fig. 1: Persistent mechanical back pain during 3-4 weeks in a 57-year-old man with AS. Lateral radiograph of the thoracolumbar spine shows ossification of the anterior longitudinal ligament except for L1-2 level (arrow) where the bony bridging is incomplete. This sign raised the suspicion of a fracture (Fig. 3).
References: Institute of Radiology, Catholic University, School of Medicine, Rome/IT
Furthermore,
the absence of major trauma in the patient’s history,
as well as difficulties in fracture identification on the basis of radiography alone may also lead to a doctor’s delay [3,
6].
Delayed diagnosis can worsen prognosis,
as vertebral fractures are often unstable and require proper treatment in order to avoid primary and secondary neurological injury.
Inflammation and new bone formation represent the two central features of AS promoting the pathological remodeling of the spine.
Inflammation is characterized by enthesitis that determines ectopic bone formation within the affected structures and progressively leads to ossification of the spinal ligaments,
intervertebral disks,
endplates and apophyseal structures [1].
As the disease progresses,
chronic inflammation promotes the development of syndesmophytes and causes the “squaring” of the endplates of vertebral bodies,
finally resulting in the characteristic hyperkyphotic “bamboo spine” [1,
7].
AS is also associated with osteoporosis that is attributed to an uncoupling of the bone formation and bone resorption processes and promotes weakening of the spine as well as increased risk of vertebral fractures [5,
8,
9].
Biomechanically,
the loss of flexibility of the fused spine results in a structure that behaves like a long bone and acts as a rigid lever,
incapable of appropriately dissipating the energy of a traumatic event [1,
6,
10].
Susceptibility to spinal fractures in patients with AS is further increased by a significantly impaired mobility,
as well as problems with balance and coordination that reduce the ability to take protective measures during a fall [1,
11].