Diverticulitis
Diverticula are small bulging pouches of mucosa and submucosa through the muscularis of the colonic wall.
Diverticula can be found anywhere in the colon,
but predominantly in the descending and sigmoid colon.
They can also occur anywhere in the digestive system,
but they are less common than those arising from the colon.
Diverticulitis results from the obstruction of the neck of the diverticulum,
with subsequent inflammation,
perforation and infection.
The infection may later progress to abscess formation and/or generalised peritonitis.
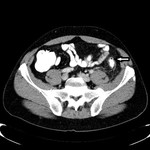
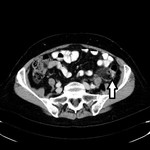
The appearance of acute diverticulitis on CT scans parallels the pathologic features.
The most common CT finding is paracolic fat stranding,
relatively mild focal intestine wall thickening,
presence of diverticula,
“comma sign” – accumulation of fluid in the root of the sigmoid mesentery,
and “centipede sign” – engorgement of the mesenteric vessels (Fig.
3-8).
Diagnosis of diverticulitis from CT findings may be difficult to make when the location is atypical.
The combination of diverticula and accentuated fat stranding suggests the diagnosis,
even in unusual locations,
such a small intestine (Fig.
9).
The most important entity in the differential diagnosis is colon adenocarcinoma.
There are several features that help to differentiate these two conditions as summarized in Table (Fig.
10-11) [1].
Appendicitis
Acute appendicitis is a very common cause of acute abdominal pain that requires surgical intervention.
Acute appendicitis occurs when the appendiceal lumen is obstructed leading to fluid accumulation,
luminal distension,
inflammation,
and finally perforation.
Direct visualization of dilated,
≥ 6 mm in maximum diameter,
fluid filled appendix is the most specific CT finding of appendicitis.
Other direct signs include appendiceal wall thickening (wall ≥ 3mm),
appendiceal wall hyperenhancement and periappendicular fat stranding (Fig.
12-13).
Periappendicular fat stranding is typically mild to moderate,
but it can be severe.
Secondary signs include appendicolith(s),
or thickening of the cecal apex.
Appendicoliths are present in one third of patients with appendicitis,
although they are not diagnostic.
Appendicoliths may have prognostic importance because their presence increases the likelihood of appendiceal perforation (Fig.
14) [5].
Epiploic appendagitis
Epiploic appendages are small adipose pouches that arise from the serosal surface of the colon to which they are attached by a vascular stalk.
There are approximately 50-100 epiploic appendages,
typically 1-2 cm thick and 2-5 cm long.
They are visible on CT images only if they are surrounded by fluid or inflammed.
Sigmoid colon and cecum are the main sites of involvement.
Epiploic appendagitis has been reported in 2,3-7,1% of patients clinically suspected of having diverticulitis and 0,3-1% of patients suspected of having appendicitis [2].
Their torsion leads to infarction which results in a focal inflammation.
CT findings include paracolic oval fatty mass,
well-circumscribed hyperattenuated rim,
sometimes central dot and paracolic fat stranding (Fig.
15-17) [1-4].
Omental infarction
The greater omentum is a fat - laden peritoneal fold extending from the greater curvature of the stomach to adjacent organs in the abdominal cavity.
The blood supply of the greater omentum travels mostly through the right and left gastroepiploic arteries [3].
Normally it appears on CT scans as a band of fatty tissue with small vessels and is located just anterior to the transverse colon.
Omental infarction develops as a result of venous hemorrhagic infarction,
either due to torsion or spontaneous.
Risk factors include obesity and recent surgery.
Segmental omental infarction typically occurs on the right causing upper or lower right quadrant pain and often leads to clinical misdiagnosis of appendicitis or gallbladder disease.
On CT scans,
the infarcted omentum appears as a cakelike high-attenuation fatty mass centered in the omentum.
Reactive bowel wall thickening may be present,
but the inflammatory process in the omentum is usually more severe (Fig.
18) [1-3].
Other causes of fat stranding
Other acute and chronic entities of the mesentery and bowel wall although less common should be considered in the differential diagnosis.
Acute conditions that cause fat stranding include peritonitis; inflammation,
infection or ischemia of the bowel (these entities typically cause circumferential thickening of the bowel wall that is more severe than associated fat stranding; perforation of colon cancer; inflammation associated with pancreatitis or cholecystitis; trauma and surgery.
Chronic conditions that cause fat stranding include neoplasm of the omentum (primary or metastases),
chronic infections of the omentum (tuberculosis) and mesenteric panniculitis (Fig.
19) [1-4].