A new service for the specialist evaluation and follow up of lung nodules was introduced at South Devon Healthcare NHS Foundation Trust (Torbay,
UK) in November 2014.
Nodules identified during the reporting of radiological investigations are highlighted to the referring clinician via a short code to which all radiologists at our institution have been made aware.
A proforma is sent to the referring clinician (Hospital consultant or General Practitioner) for completion.
This proforma is returned to the Virtual Lung Nodule Clinic (VLNC) for assessment of suitability.
The VLNC is held weekly and run by a consultant respiratory physician and consultant chest radiologist.
The physician reviews the clinical details on the proforma and the patient’s hospital notes.
The radiologist reviews relevant imaging.
There is no need for the patient to be present as the value of clinical assessment in patients with (normally) asymptomatic lung nodules is limited. Ten cases are usually reviewed over a one to two hour period.
Broad guidelines that mandate referral to the VLNC are:
- Anyone with a lung nodule fitting the size criteria (5mm - 15mm) which may have resulted in an unnecessary respiratory clinic referral in the past.
- Anyone with a lung nodule fitting the size criteria (5mm - 15mm) where there is uncertainty about what management plan needs to be followed for a small lung nodule or nodules.
Groups who do not need referral include:
- Patients with known cancer who are already on follow up for their primary cancer and being looked after in an MDT setting.
- Where the radiologist is happy they have sufficient information to recommend the appropriate follow up or management plan.
The radiological assessment of lung nodules is now based on new British Thoracic Society guidelines published in August 2015.
Review of previous imaging and comparison with nodule size,
morphology and volume measurements are performed.
Nodules are managed according to recent BTS guidelines.
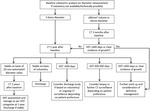
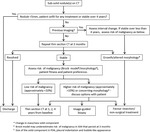
Algorithms are presented opposite (Figs 1-3).
Risk for malignancy calculators are used which are freely available on the BTS website.
Possible outcomes include:
- Reassure and discharge
- Repeat CT scan in accordance with the BTS guidelines and review in nodule clinic.
- Advise clinical assessment.
- Request PET-CT scan.
- Referral to an MDT
A detailed non-medical letter is dictated to the patient with a copy sent to the GP and referring hospital clinician if appropriate explaining the imaging findings and management plan.
The patient is also given a contact number if they want to phone and speak to one of the respiratory team.
In addition they are sent a detailed patient information leaflet about incidental lung nodules.
Outcomes
The VLNC has been run for 14 months at the time of writing (starting in November 2014).
As at December 2014 94 separate patients have been discussed with a total of 109 'attendances'.
Of these,
29 patients have so far been discharged from the VLNC (30%).
Twenty-four of these patients (83%) were discharged after one review at the VLNC.
Of patients discharged,
intrapulmonary lymph nodes and granulomata were the most common findings.
The majority of patients (n=51) had pulmonary nodules which required or will require follow-up with CT.
Eight patients were referred for further investigation with PET-CT and six patients required formal review in respiratory clinic for suspicious nodules.
Non chest hospital consultants and GPs are enthusiastic about the service as it gives them easy access to an expert chest opinion regarding the management of pulmonary nodules.
We are in the process of getting feedback from patients.
To date none have requested phone or face to face communication.
Indicative Cases
Case 1
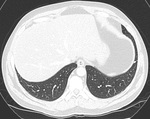
A 68 year old male had a CT thorax abdomen and pelvis due to suspicion of malignancy following an unprovoked DVT.
This demonstrated a 7mm nodule within the left lower lobe which was classed as indeterminate by the reporting radiologist (Fig 4).
The case was reviewed at the VLNC and the nodule was thought to have the hallmarks of an intrapulmonary lymph node (Figs 4&5).
The referring clinician and patient were informed and no further follow up was required.
Case 2
A 55 year old female had an incidentally discovered lung nodule on CT in December 2013 (Fig 6).
This was followed up with CT chest twice at 6 monthly intervals during which time the nodule increased in volume measurement (Figs 7&8).
A PET-CT was therefore performed which did not show increased metabolic activity (Fig 9). MDT opinion was that the nodule was most likely benign,
but a further CT chest is planned for January 2016 to ensure no further increase in size.
Case 3
A 69 year old male smoker had a CT chest and abdomen following a possible nodule discovered on chest radiograph performed for cough.
CT demonstrated a 19mm nodule within the left lower lobe (Fig 10) which was referred to the VLNC.
The Brock score was 18.8% and therefore a PET-CT was performed.
This showed the lung nodule was of increased metabolic activity in keeping with malignancy (Fig 11).
There was no regional or distant disease and the patient is scheduled for surgical treatment.
Case 4
A 54 year old female with a previous history of breast cancer had a 13mm lung nodule discovered during a CT performed for right upper quadrant pain (Fig 12).
This was reviewed at the VLNC and a Brock score of 10.2% was calculated.
A PET-CT was performed which demonstrated increased metabolic acitivty within the lung nodule (Fig 13) as well as mediastinal lymph nodes and bones (not visible on CT) consistent with metastatic spread of breast cancer.