This poster is published under an
open license. Please read the
disclaimer for further details.
Type:
Educational Exhibit
Keywords:
Musculoskeletal system, Radioprotection / Radiation dose, Extremities, CT, MR, Ultrasound, Radiation safety, Physics, Safety, Trauma, Arthritides, Calcifications / Calculi
Authors:
J. Ninčević1, Z. Atlagović2, M. Mustapic1; 1Zagreb/HR, 2Nova Gradiška/HR
DOI:
10.1594/ecr2016/C-1075
Findings and procedure details
There are a few principles that should be fulfilled in order to obtain dose reduction in patients who undergo CT examination.
1. Indication
All clinicians should be aware of the dose delivered during CT examinations.
Routine,
frequent and repeated CT examinations,
without providing new information should be avoided.
Clinical information is always crucial.
Depending on the clinical findings,
radiologists should suggest the best imaging modality regarding the specific pathological entity.
For instance,
in politrauma patients or in pre-operative planning, CT is supreme method,
depicting calcified bone matrix,
and using multiplanar and three-dimensional reconstructions.
In those cases CT is definitely indicated.
2. Substitution
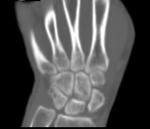
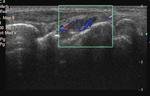
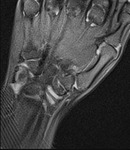
Whenever possible CT should be replaced by non-irradiating imaging modality such as sonography or MRI.
It is absolutely justified,
especially in children (Fig.
1-3).
The published results of different studies showed the possible benefits of substitution.
There is a study of 30 lumbar CT in patients under the age of 35 which showed that only 7 (23%) CT examinations were really indicated,
20 (67%) patients would have benefited from MRI and in 3 patients imaging was not indicated at all.
Analysing cost-benefit ratio,
another study demonstrated that 90% of the lumbar CT could have been replaced by MRI.
3. Optimisation
Both radiologists and radiology technicians should be involved in protocol optimisation.
Performing dynamic or perfusion CT examinations,
the dose can be reduced by limiting the number of acquisition phases.
Precise anatomic zone centering enables optimum ratio of image quality and irradiation dose.
Positioning of the patient is important,
which means that peripheral joints should be scanned as far as possible from the patient’s body in order to reduce the dose delivered to radiosensitive organs.
Reduction of kilovoltage,
especially during peripheral joints examinations,
reduces the dose.
For instance,
reduction from 120 to 80 kV reduces the dose 2.2 times,
which enables enough contrast resolution for bone structure analysis.
For proximal joints,
near patient's trunk,
such as shoulder,
hip,
sacroiliac or spine,
suggested kilovoltage depends on patient’s morphotype (120 kV for standard morphotype,
100 kV in thin patients and 135-140 kV in overweight patients).