This poster is published under an
open license. Please read the
disclaimer for further details.
Keywords:
Outcomes, Diagnostic procedure, Normal variants, Nuclear medicine conventional, Gastrointestinal tract, Quality assurance
Authors:
V. M. Rhodes, N. Moffitt, T. Toma; SOUTHEND ON SEA/ESSEX/UK
DOI:
10.1594/ecr2016/C-1199
Results
This study comprised of 279 patients who were referred for and underwent a SeHCAT scan consecutively between 30th Sept 2013 and 30th Sept 2015.
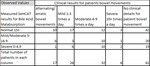
Of these patients 85 (30.5%) had post cholecystectomy diarrhoea and of these 40 (47%) patients had positive SeHCAT results (Table 3).
From the NICE guidelines a positive SeHCAT result of 0-4.9 is severe,
and 5-15 is mild/moderate,
whereas 15+ is a normal result.
Of the 279 patients who were part of this study 207 (74.2%) were female leaving 72 (25.8%) male.
Of the 85 patients who had undergone cholecystectomy 78 (91.8%) were female and 7 (8.2%) male (Table 3).
Diarrhoea is described as an increase in frequency of bowel movements or a significant variation of the stools characteristics from previous bowel habits that often lead to loose watery bowel motions (Notta et al 2011).
The severity of diarrhoea is determined by the size and number of stools passed within a period of time.
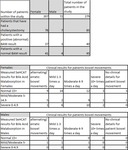
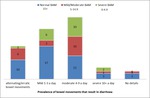
From the clinical details 4 categories of bowel motions were determined,
1) mild diarrhoea 1-3 times a day,
2)moderate diarrhoea 4-9 times a day,
3) severe diarrhoea 10+ times a day and 4) patients with alternating/erratic diarrhoea episodes who may have some good days intermixed with bad days.
Of the 85 patients who presented with post cholecystectomy diarrhoea there were 26,
32,
6 and 17 patients in each category respectively.
4 patients (3 with normal BAM and 1 with mild/moderate BAM) were rejected from the final study at this point as clinical details for these patients’ diarrhoea severity were unable to be obtained due to the unavailability of the patient notes.
Table 1 depicts the results of both the patients’ bile acid malabsorption and the severity of their diarrhoea,
for the set of patients who had undergone cholecystectomy.
The χ2 test was used for comparison of the qualitative data gathered by the retrospective study.
The χ2 test tested our null hypothesis that there is no correlation between the clinical severity of the patient’s diarrhoea and a positive result for bile acid malabsorption.