This poster is published under an
open license. Please read the
disclaimer for further details.
Keywords:
Outcomes, Diagnostic procedure, Normal variants, Nuclear medicine conventional, Gastrointestinal tract, Quality assurance
Authors:
V. M. Rhodes, N. Moffitt, T. Toma; SOUTHEND ON SEA/ESSEX/UK
DOI:
10.1594/ecr2016/C-1199
Conclusion
Conclusion
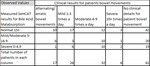
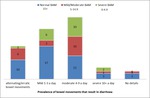
The results,
in table 1 and fig 1,
show that in patients who had undergone SeHCAT testing post-cholecystectomy,
more patients had diarrhoea with a normal SeHCAT result,
and therefore no BAM present after cholecystectomy,
than patients that had diarrhoea with a positive SeHCAT result.
This gives rise to the probability that there are additional unknown factors which may play a role in the prevalence of these patients diarrhoea.
Our results have also shown that only 47% of patients who had post-cholecystectomy diarrhoea had a positive result for bile acid malabsorption.
This suggests that over half of the patients within this study must have some capacity for bile acid reabsorption after surgery,
which may help them to compensate for the changes in intestinal transit time and bile acid load after surgery.
Farahmandfar et al’s (2012) review of 25 studies concluded that cholecystectomy did not seem to have any positive effect on diarrhoea,
and although cholecystectomy does not seem to significantly improve pre-operative diarrhoea it may be the cause of new onset post-operative diarrhoea.
However from the results we obtained this new onset of diarrhoea does not seem to affect the severity that the patient suffers.
The results acquired appear to demonstrate no definitive association between described severity of diarrhoea and positive bile acid malabsorption result.
This is corroborated by the results of the χ2 test from which a P value of 0.996 is obtained.
This confirms the null hypothesis has a 99.6% of being correct (Table 2).
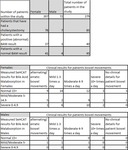
Males and females who had had a SeHCAT test and a cholecystectomy were looked at separately (Table 3),
as it is known that they differ in most aspects of bowel function .
However with such a disproportional number of women (91.8%) vs men (8.2%) in this study we cannot accurately assess any significant difference between the male prevalence of post cholecystectomy diarrhoea,
with a positive BAM result,
compared to the females due to the small study size (Hearing et al 1999).
As this was a retrospective review there were some limitations encountered.
This includes the fact that there was no clear pre-study classification for patient assessed diarrhoea and as such there may be differences in definitions of what constitutes as diarrhoea and how it affects the patient.
There is also some concern over whether what the patient describes as diarrhoea is real diarrhoea or pseudo-diarrhoea (an increased frequency of defecation) as the records given do not always clearly separate these.
As no symptom questionnaire was administered prior to the SeHCAT test we had to rely on the documentation of these symptoms in the patients’ notes,
this prevented us from using any validation criteria,
such as the Rome III criteria,
to ensure accuracy with our results(O’Donnell 1999,
Notta et al 2011,
Gracie et al 2012).
In conclusion our aim was to determine whether the prevalence of post cholecystectomy diarrhoea had any correlation to the clinical severity of the patient’s diarrhoea and a positive result for type 3 bile acid malabsorption and we were able to conclude that there is no correlation between severity of diarrhoea experienced and the positive outcome of a SeHCAT test for bile acid malabsorption.