INFLAMMATORY DISEASES
MULTIPLE SCLEROSIS
- Definition: Multiple sclerosis (MS) is a progressive neurodegenerative disorder characterized histopathologically by multiple inflammatory demyelinating foci called “plaques.”
- Location: Most MS plaques are supratentorial.
Less than 10% occur in the posterior fossa although infratentorial lesions are relatively more common in children.
MS plaques in the deep cerebral white matter are linear,
round,
or ovoid lesions that are oriented perpendicular to the lateral ventricles at or near the callososeptal interface.
Centripetal perivenular extension is common,
causing the appearance of “Dawson fingers” radiating outward from the lateral.
Other commonly affected areas include the subcortical U-fibers,
brainstem,
and spinal cord.
Infratentorial lesions were shown to have a sensitivity of 66% and a specificity of 98% in the diagnosis of MS.
A typical location are the middle cerebellar peduncles near the exit pathways of the cranial nerves and along the surfaces of cisterns and 4th ventricle with subtle mass effect upon it.
- Epidemiology: Onset typically occurs in young to middle-aged adults from 20-40 years of age.
It has been estimated that 35% of patients presenting with clinically isolated syndrome with brainstem involvement will develop clinically definite MS.
Furthermore,
lesions are commonly found in the brainstem in patients who have already received a diagnosis of MS
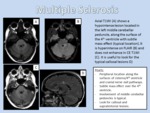
- Imaging Findings: Most MS plaques are hypo- or isointense on T1WI.
The hypointensity “black holes” correlates with axonal destruction and chronic/severe cases typically show moderate volume loss and generalized atrophy,
the corpus callosum becomes progressively thinner and is best delineated on sagittal T1WI.
Acute lesions are characteristically hyperintense in T2 and FLAIR and are contrast enhancing. Restricted diffusion is not characteristic.
Lesions show incomplete peripheral contrast enhancement “open ring” enhancement,
although this feature might be difficult to see in areas of demyelination in the brainstem and cerebellum because of their usual small size.
Large abnormalities still do occur that may be confused with tumors like gliomas,
but acute lesions do not usually develop cysts or an exophytic component (Figure 1).
Demonstrating typical supratentorial MS lesions,
specifically in the periventricular white matter touching the ventricular surface and the callososeptal sulcus,
are other findings that may be helpful in reaching a diagnosis.
Although neuromyelitis optica (Devic’s disease) can have brainstem,
optic nerve and spinal cord involvement while sparing the brain.
NEUROSARCOID
- Definition: Sarcoidosis is a multisystem inflammatory disorder characterized by discrete non-caseating epithelioid granulomas.
When sarcoidosis affects the CNS it is termed Neurosarcoid (NS).
- Epidemiology: it affects the CNS in approximately 5% of cases,
usually in combination with disease in other organs.
Only 5-10% of NS cases are confined to the CNS and occur without evidence of systemic sarcoidosis.
- Location: Leptomeninges,
especially around the base of the brain in the form of diffuse leptomeningeal thickening +/- focal nodular lesions is seen in about 40% of cases and the hypothalamus and infundibulum are also favored intracranial sites.
NS can involve cranial nerves,
eye and periorbita,
bone,
the ventricles and choroid plexus,
and the brain parenchyma itself.
Both supra- and infratentorial compartments are affected.
Sarcoid can also involve the spinal leptomeninges,
cord,
and nerve roots.
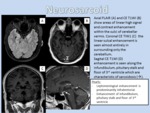
- Imaging Findings: NS is isointense with brain on T1WI and hyperintense relative to CSF.
Sulci filled with leptomeningeal infiltrates appear effaced and there are also dura-based masses.
Signal intensity on T2 depends on the amount of fibro collagenous material present.
Longstanding dural lesions are relatively hypointense and are very characteristic,
while parenchymal infiltration along the perivascular spaces causes a vasculitis-like reaction with edema,
mass effect,
and hyperintensity on T2/FLAIR.
The most common finding on T1 C+ scans is nodular or diffuse leptomeningeal thickening and parenchymal disease in half of the patients.
Hypothalamic and infundibular thickening with intense enhancement is seen in 5-10% of cases and although rare,
NS may cause solitary or multifocal thickened enhancing cranial nerves as well as enhancing masses in the ventricles and choroid plexus (Figure 2).
NEUROBEHÇET SYNDROME
- Definition: Behçet’s disease (BD) is a vasculitis characterized by the presence of the classic triad of uveitis,
oral aphthae,
and genital ulcers.
- Epidemiology: This syndrome affects young adults,
predominantly men,
between 20 and 40 years of age.
Neurological signs in BD are present in from 4% to 49% of cases.
However,
most patients diagnosed with BD that do not exhibit clinical signs of CNS involvement will not have abnormal cranial MRI findings.
- Location: it most often involves the brainstem,
especially around the cerebral peduncles and the pons.
The thalamus and basal ganglia are the next most common sites of involvement,
and similar foci can be noted in the cerebral hemispheres.
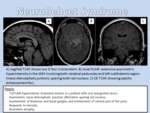
- Imaging Findings: Small foci of high signal intensity on T2WI images; these foci are iso or hypointense relative to brain parenchyma on T1-weighted images Lesions may be circular,
linear,
crescent-shaped,
or irregular.
The development and disappearance of lesions at CT and MR imaging correlate with the course of clinical neurologic deficits.
Lesions have a pronounced tendency to extend cranially or caudally into other BS segments or even into the cerebellum or supratentorial region (thalami and basal ganglia) and midbrain and central pons involvement that spares the red nucleus is a characteristic finding (Figure 3).
The supratentorial and peripheral location as well as the clustering of the lesions around the 4th ventricle helps to suggest MS over Neurobehçet.
Characteristically lesions may diminish in size or even to remit completely in response to steroids alone or in combination with immunosuppressive drugs.
WALLERIAN DEGENERATION
- Definition: Wallerian degeneration (WD) is anterograde degeneration of axons and the surrounding myelin sheaths secondary to injury of the cortex or subcortex.
- Etiology: In the brain,
WD most often occurs after trauma,
infarction,
demyelinating disease,
or surgical resection.
- Location: Virtually any WM tract or nerve in the brain,
spinal cord,
or peripheral nervous system can exhibit changes of WD.
The caudally directed motor fiber pathways of the descending corticospinal tract (CST) are the most common sites of visible brain involvement.
Other affected locations include the corpus callosum,
optic radiations,
fornices,
and cerebellar peduncles.
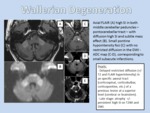
- Imaging findings: MRI findings for WD are visible over the entire affected tract and follow a sequence after the initial insult.
+ Stage 1: during the first 4 weeks of the insult there are no abnormalities in MRI.
+ Stage 2: 4 to 14 weeks,
transient T2 hypointensity in the affected tract.
+ Stage 3: 14 weeks to 6 months is the period where the characteristic high T2 signal intensity is seen along the affected white matter tract.
+ Stage 4: in 6 months to several years the changes become chronic and reduced volume of the affected tract can be visualized.
DWI reveals early abnormalities in the affected tract from day 2 after onset of the disorder with restricted diffusion of the affected tract on ADC mapping,
but these abnormalities are transient and cease after week 2 (Figure 4).
INFECTIOUS DISEASES
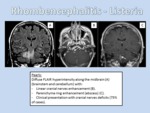
LISTERIAL RHOMBENCEPHALITIS
- Definition: Listeria monocytogenes is a food-borne pathogen and emerging cause of zoonotic infection,
it is a gram-positive intracellular bacterium that dwells in soil,
vegetation,
or animal reservoirs.
- Epidemiology: It can cause gastroenteritis,
mother-to-fetus infection,
septicemia,
and CNS infection in immunocompromised individuals,
pregnant women,
and newborns.
Cases in immunocompetent people are rare.
Symptoms include fever,
headache,
cranial nerve palsies,
vertigo,
and somnolence.
Once symptoms of CNS disease develop,
the mortality rate is 25-30%.
- Location: it shows a specific tropism for the meninges,
brainstem and lower cranial nerves.
- Imaging findings: they are non-specific and can occur as meningitis,
encephalitis,
cerebritis,
or abscess.
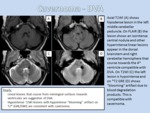
There is leptomeningeal thickening and enhancement that often locates around the lower cranial nerves.
Focal areas in midbrain,
pons,
or medulla that are hyperintense in T2 and FLAIR with no restricted diffusion are seen if cerebritis is present (Figure 5).
Parenchymal ring enhancement with significant perilesional edema is seen in cases of abscess,
and the etiology should be suspected for in an appropriate clinical setting and the characteristic imaging findings.
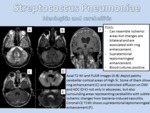
PNEUMOCOCCAL RHOMBENCEPHALITIS AND MENINGITIS.
- Definition: Streptococcus pneumoniae is a common cause of pneumonia,
sinusitis and acute otitis media.
Moreover,
S.
pneumoniae is a common cause of bacterial meningitis in both children and adults (especially in the elderly) in the setting of septicemia.
- Location: involvement of the supratentorial meninges with or without infratentorial compromise may be observed.
Extension of the disease to the CNS parenchyma in adults is rare and has rarely been reported.
Infratentorial involvement is invariably seen along supratentorial disease.
- Findings: Contrast enhancement of the leptomeninges is primarily seen.
DWI can show multiple widespread parenchymal foci of increased signal intensity,
consistent with multiple acute infarctions from small vessel bacterial-induced vasculitis.
Changes secondary to cerebellitis with ill-defined and often multiple areas of T2/FLAIR hyperintensity and abscess formation with parenchymal ring enhancement can be observed (Figure 6).
All of these changes are non-specific and etiology is found during CSF,
blood or other infections sites cultures.
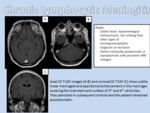
CHRONIC LYMPHOCYTIC MENINGITIS
- Definition: Aseptic meningitis is a clinical syndrome characterized by meningeal inflammation (increased white blood cell count in cerebrospinal fluid) without identification of bacterial pathogen in cerebrospinal fluid by routine culture technique.
Chronic lymphocytic meningitis occurs when multiple episodes of such meningitis are identified and no etiology can be documented.
- Epidemiology: possible causes include viruses,
fungi,
difficult to culture bacteria,
malignancy,
drug exposure,
or autoimmune diseases.
- Location and imaging findings: Location and imaging findings of chronic lymphocytic meningitis are nonspecific and no different from the ones described for RHOMBENCEPHALITIS as a whole.
They tend to be small,
subtle changes mostly in the form of leptomeningeal thickening or small nodules that may or may not show contrast enhancement (Figure 7).
Imaging findings do not denote acute disease since meningeal changes can persist over time.
It is mostly a diagnosis of exclusion when all of the other aforementioned causes are tested for and excluded (as it was the case in our patient).
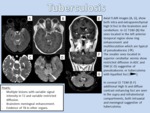
TUBERCULOSIS
- Definition: Tuberculosis of the central nervous system can result from either hematogenous spread from distant systemic infection as well as direct extension from local infection.
- Epidemiology: CNS involvement is thought to occur in 2-5% of patients with tuberculosis and up to 15% of those with AIDS-related tuberculosis.
- Patterns of infection and imaging findings:
A) Acute/subacute TB meningitis (TBM): constitutes 70-80% of cases as an inflammatory reaction in the cisterns,
or as an isolated pachymeningitis with focal or diffuse dura-arachnoid thickening.
There are basilar exudates which are isointense with brain on T1WI,
giving the appearance of “dirty” CSF.
FLAIR scans show increased signal intensity in the sulci and cisterns.
Marked linear or nodular meningeal enhancement is seen on T1 C+ FS sequences ((Figure 8).
Tuberculous exudates often extend into the brain parenchyma along the perivascular spaces,
causing a meningoencephalitis.
Vascular complications are common complications of TBM.
The “flow voids” of major arteries may appear reduced.
Parenchyma adjacent to meningeal inflammation may demonstrate necrosis.
Penetrating artery infarcts with enhancement and restricted diffusion are common.
B) Neurotuberculosis (Tuberculoma): solid focal parenchymal infection with central caseating necrosis which can be found anywhere and appear hypo or isointense with brain on T1WI and hypointense on T2WI.
Liquefied areas may be T2 hyperintense with a hypointense rim.
Enhancement is variable,
ranging from small punctate foci to multiple rim-enhancing lesions.
Mild to moderate round or lobulated ring-like enhancement around a non enhancing center is the most typical pattern.
Solid caseating tuberculomas do not restrict on DWI although liquefied foci may restrict (Figure 8).
MRS can be very helpful in characterizing tuberculomas and distinguishing them from neoplasm or pyogenic abscess.
A prominent decrease in NAA:Cr with a modest decrease in NAA:Cho is typical.
A large lipid peak with absence of other metabolites such as amino acids and succinate is seen in 85-90% of cases.
C) TB Pseudoabscess: contains macrophages and liquefied necrotic debris.
Unlike tuberculomas,
TB pseudoabscesses are usually hyperintense to brain on T2/FLAIR and restrict on DWI.
A ring-enhancing multiloculated lesion or multiple separate lesions is the typical finding on T1 C+ images (Figure 8).
MRS shows lipid and lactate peaks without evidence of cytosolic amino acids.
NEOPLASTIC DISEASE
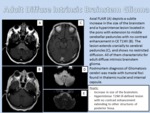
ADULT DIFFUSE INTRINSIC LOW-GRADE BRAINSTEM GLIOMA
- Definition: Adult diffuse intrinsic low-grade brainstem glioma (ADILGBS) are poorly demarcated nonhenancing lesion affecting more than 50% of the brain stem.
- Epidemiology: they appear in young adults between 20 and 50 years and are the most frequent type of brainstem glioma in adults.
- Location: may be limited to brainstem segments (midbrain,
pons,
medulla) but as they are a diffuse kind of lesion,
they can also infiltrate adjacent brainstem segments or adjacent regions such as the cerebellum or thalamus.
- Imaging Findings: Diffuse enlargement of the brainstem with hyperintense areas on T2WI and FLAIR sequences and hypointense signal on T1WI distributed In the aforementioned locations without contrast enhancement or restricted diffusion ((Figure 9).
In some cases,
pontine lesions present a ventral exophytic growth surrounding the basilar artery.
MRS shows a pattern similar to that observed in supratentorial gliomas with an elevation of Cho/NAA ratio,
Cho/creatine ratio,
and lactate peak.
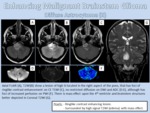
ENHANCING DIFFUSE BRAINSTEM GLIOMA
- Definition: Enhancing Diffuse Brainstem Glioma (EDBG) are contrast enhancing lesions representing the second most common group of brain stem glioma in adults.
- Epidemiology: EDBG generally appear in patients older than 40 years and histologically are mostly anaplastic astrocytomas and glioblastomas.
- Imaging Findings: EDBG present as a contrast-enhancing mass surrounded by an area of edema with mass effect.
Almost two thirds of patients exhibit enhancement in a ring like pattern (Figure 10).
Unfortunately the radiological appearance is nonspecific and further work up is needed in order to distinguish them from other contrast enhancing lesions in the brainstem of multiple etiologies and biopsies are often needed,
with PET with 18F fluorodeoxyglucose and 11C methionine being helpful in the search of a biopsy target.
Foci of contrast enhancement often show increased perfusion in MR perfusion.
EXOPHYTIC BRAINSTEM GLIOMA
- Definition: exophytic contrast enhancing gliomas not classified in any of the other adult brainstem gliomas groups (ADILGBS,
EDBG,
tectal gliomas).
- Epidemiology: They are very rare in adults and are mostly pilocytic astrocytomas (Grade I WHO).
PILOCYTIC ASTROCYTOMA (GRADE I WHO)
- Definition: is a well-circumscribed,
typically slow-growing glioma of young patients,
classified as a type 1 glioma according to WHO.
- Location: The cerebellum is the most common location,
followed by the optic chiasm and nerve,
and pons and medulla.
- Imaging findings: The most common appearance of a posterior fossa PA is a well-delineated cerebellar cyst with a mural nodule,
they are well-delineated and appear slightly hyperintense to CSF on both T1-and T2WI.
They do not suppress completely on FLAIR.
The mural nodule signal intensity is variable.
Solid PAs appear iso- or hypointense to parenchyma on T1WI and hyperintense on T2/FLAIR.
They show striking enhancement following contrast administration and specially heterogeneous enhancement of the nodule.
Enhancement of the cyst wall itself varies from none to moderate (Figure 11).
Our case show the variant pattern in which the solid component predominates,
and it was described in pathology to have a high index of proliferation despite the low grade of the lesion which might probably account for the spread and signal changes seen extending downward to medulla and spine.
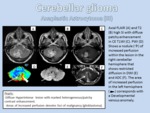
CEREBELLAR GLIOMAS
- Definition: adult cerebellar gliomas are an uncommon entity often second to the more frequent brainstem gliomas.
- Epidemiology: the most common are the malignant grade III WHO anaplastic astrocytoma,
and the grade IV WHO glioblastoma multiforme.
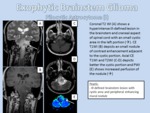
ANAPLASTIC ASTROCYTOMA (GRADE III WHO)
- Definition: it is a diffusely infiltrating WHO grade III astrocytoma that has an intrinsic propensity to undergo further malignant degeneration into glioblastoma multiforme (GBM) and can either develop de novo or arise from malignant degeneration of grade II lesions.
- Location: Posterior fossa location is rare in adults,
they are mostly found in the brainstem and less often in the cerebellum.
- Epidemiology: peak presentation is between 40-50 years.
There is a slight male predominance.
- Imaging Findings: In MRI most AAs are hypointense on T1WI and hyperintense on T2/FLAIR.
The margins may appear grossly discrete,
but tumor cells invariably infiltrate adjacent brain.
Hemorrhage and calcification are uncommon,
so T2* (GRE/SWI) “blooming” is typically absent.
Contrast enhancement varies from none to moderate.
Between 50-70% of AAs show some degree of enhancement in different nonspecific patterns may indicate a more malignant astrocytoma,
with foci tending toward glioblastoma (grade IV) (Figure 12).
AAs generally do not restrict on DWI.
MRS shows elevated choline and decreased NAA.
The mI:Cr ratio is generally lower than that of LGAs.
Perfusion MR shows increased rCBV in the most malignant parts of the tumor.
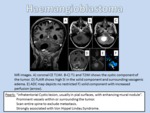
HEMANGIOBLASTOMA
- Definition: Hemangioblastoma is also known as capillary hemangioma,
it is a benign,
slow-growing,
relatively indolent vascular neoplasms that occurs in both sporadic and multiple forms,
the last of which are almost always associated with the autosomal-dominant inherited cancer syndrome von Hippel-Lindau disease (VHL).
- Epidemiology: It is generally a tumor of adults between the ages of 30 and 65 years and are rare in the pediatric population.
- Location: It accounts for 1-2.5% of primary CNS neoplasms and approximately 7% of all primary posterior fossa tumors in adults and It is the second most common infratentorial parenchymal mass in adults (after metastasis).
- Imaging Findings: The most common appearance is a well delineated iso to slightly hyperdense nodule associated with a hypodense cyst.
Calcification and gross hemorrhage are absent.
The nodule enhances strongly and uniformly following contrast administration.
In MRI an isointense nodule with prominent “flow voids” is seen on T1WI.
If an associated peritumoral cyst is present,
it is typically hypointense to parenchyma on T1WI but hyperintense compared to CSF.
Compared to brain parenchyma,
the tumor nodule is moderately hyperintense on T2WI and FLAIR.
Intratumoral cysts and prominent “flow voids” are common.
The cyst fluid is very hyperintense on both T2WI and FLAIR (Figure 13).
It occasionally has areas of hemorrhages which present with “blooming” on T2* (GRE/SWI).
Intense enhancement of the nodule but not of the cyst itself is typical and cyst wall enhancement should raise the possibility of tumor involvement as compressed,
non neoplastic brain does not enhance.
Non cystic Hemangioblastomas enhance strongly but often heterogeneously and multiple are seen in VHL and vary from tiny punctate to large solid tumors.
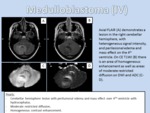
MEDULLOBLASTOMA
- Definition: Medulloblastoma (MB) is a grade IV WHO neoplasm of embryonal origin.
- Epidemiology: they are accounted to cause 10% of all pediatric brain tumors,
but there is a second,
smaller peak in adults aged 20-40 years.
- Location: Medulloblastomas in adults are often eccentric,
arising from the cerebellar hemisphere rather than the vermis (unlike children).
Lateral medulloblastomas my remain intraaxial,
and should be considered along with astrocytomas and hemangioblastomas in the differential diagnosis.
- Imaging Findings: MBs have relatively defined margins on imaging studies but despite this appearance,
40-50% have CSF dissemination at the time of initial diagnosis,
therefore preoperative contrast-enhanced MR imaging of the entire neural axis is recommended.
CT scans may show cysts and calcifications (20%).
Almost all MBs are hypointense relative to gray matter on T1WI and slightly hyperintense on T2WI,
with peritumoral edema present in one-third of cases and obstructive hydrocephalus with transependymal CSF migration being common and best delineated on FLAIR.
Enhancement patterns show striking variation,
ranging from minimal to patchy to marked.
Because of their dense cellularity,
MBs often show moderate restriction on DWI (Figure 14).
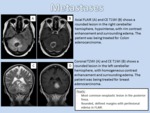
METASTASES
- Definition: The most common tumors metastasizing to the brain originate from tumors of the lung,
breast,
malignant melanoma,
gastrointestinal and genitourinary tumors.
- Location: Although 85% of metastatic lesions are supratentorial,
metastasis is still the most common intraaxial neoplasm of the adult posterior fossa.
About 20% of all intracranial metastases occur in the posterior fossa.
Multiple lesions are the hallmark,
but in the posterior fossa there is a high incidence of solitary lesions (25-50%).
- Imaging Findings: They are round and better circumscribed than primary tumors.
They mostly incite a large zone of peritumoral cerebral edema commensurate with a rapidly growing mass,
that is hyperintense on T2 and FLAIR images.
On T1 images most metastases are iso-to hypointense even though in case of hemorrhage T1 hyperintensity is seen.
On T2 metastases are more frequently hyperintense,
but iso- to hypointense lesions can be sometimes detected as well.
Metastases can be solitary and very large with a necrotic central portion mimicking aggressive primary tumors,
the pattern of contrast enhancement can be homogeneous,
nodular,
inhomogeneous or ring-like.
The amount of peritumoral edema is variable.
In small cortical lesions,
edema may be absent but the degree of edema is greater with metastatic lesions than with primary tumors ((Figure 15).
There no pathognomonic signs and diagnosis is almost always made in the presence of a known primary tumor,
nevertheless,
around 20% of them can be hemorraghic and narrowed down to melanoma,
choriocarcinoma,
thyroid and renal cell carcinoma as possible primaries,
likewise,
a calcified lesion suggest a colonic primary tumour.
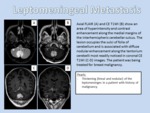
LEPTOMENINGEAL CARCINOMATOSIS
- Definition: Leptomeningeal carcinomatosis (LC) refers to diffuse seeding of the leptomeninges by tumor metastases.
- Epidemiology: it occurs in an estimated 20% of patients diagnosed with cancer and is most commonly found in breast carcinoma,
lung carcinoma,
and melanoma in adults and hematogenous malignancies and primitive neuroectodermal tumor (PNET) in children.
- Location: Leptomeningeal tumor has a spectrum of appearances on MRI ranging from diffuse leptomeningeal enhancement to bulky extra-axial tumor foci.
The most common appearance is diffuse non-nodular enhancement of the basilar cisterns and/or supratentorial cortex,
although this MRI appearance is not specific for LC.
Hydrocephalus without discernible enhancement also is commonly seen,
but the appearance is nonspecific.
- Imaging findings: Multiple enhancing leptomeningeal nodules also can be visualized in patients with LC,
with scans typically demonstrating larger tumor deposits in the basilar cisterns than in the supratentorial sulci.
These nodules may form large clumps of tumor that cause a mass effect on the adjacent brain.
Cranial nerves often are involved clinically in LC,
although many of these cases are radiologically occult.
High-resolution contrast-enhanced techniques with fat saturation aid in the detection of cranial nerve tumor deposits,
but close attention to the nerves is often necessary to detect the subtle abnormalities in these cases.
Involved cranial nerves may have mild peripheral enhancement,
which may be easily missed,
as the only MRI abnormality.
More grossly involved nerves may be enlarged and irregular,
with nodular enhancement,
making detection easier (Figure 16).
VASCULAR DISEASE
ACUTE ISCHEMIC INFARCTION (+ HEMORRHAGIC TRANSFORMATION)
- Definition: it is characterized by the sudden loss of blood circulation to an area of the brain,
resulting in a corresponding loss of neurologic function.
Acute ischemic stroke is caused by thrombotic or embolic occlusion of a cerebral artery and is more common than hemorrhagic stroke.
They are classified in four groups: atherosclerotic,
small vessel disease,
cardioembolic,
and other.
- Hemorrhagic transformation: generally over half of all cerebral infarcts at some stage develop some hemorrhagic component,
although the majority (89%) are petechial hemorrhages,
and a minority (11%) hematomas with Importantly cardioembolic strokes,
especially large ones,
being more likely to undergo hemorrhagic transformation as well as the strokes occurring in patients who receive anticoagulant and thrombolytic therapy.
The overall rate of spontaneous hemorrhagic transformation (with hematoma) has been reported to be as high as 5%.
- Location: Posterior circulation ischemia can range from fluctuating brainstem symptoms,
caused by intermittent insufficiency of the posterior circulation (so-called VBI),
to the “locked-in syndrome," which is caused by basilar artery or bilateral vertebral artery occlusion.
Stroke syndromes of the posterior circulation account for approximately 20% of all strokes.
Basilar artery occlusion represents 8-14% of all posterior circulation strokes and carries mortality of over 90%.
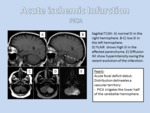
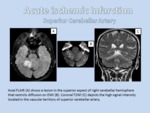
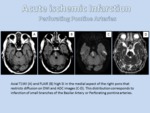
- Imaging Findings: diffusion restriction in DWI may be seen within minutes following the onset of ischemia and correlates well with infarct core.
T2WI and FLAIR is less sensitive than DWI in the first few hours to parenchymal change,
it might show loss of normal signal void in large arteries and the infarcted tissue shows high signal intensity after 6-12 hours.
In T1WI the infarcted tissue becomes hypointense,
although a ribbon of high signal intensity representing cortical laminar necrosis can be seen within 2 weeks.
CE T1WI can show very subtle foci of intra-arterial enhancement within 3 days,
as well as some degree of parenchymal enhancement that begins towards the end of the first week and can last for up to 12 weeks (Figures 17,
18,
19).
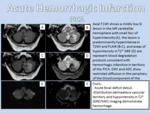
In the case of hemorrhagic infarctions,
hypointense foci with vascular distribution in T2* (GRE/SWI) demonstrate blood degradation products in the case of hemorrhagic transformation (Figure 20).
CAVERNOUS MALFORMATIONS
- Definition: Cavernous malformations are composed of a "mulberry-like" cluster of dilated thin-walled capillaries,
with surrounding hemosiderin.
- Epidemiology: Most patients who present symptomatically do so at 40-60 years of age. Most patients have single lesions and some of them may be familial.
They are commonly seen after therapeutic irradiation of the brain,
along with capillary telangiectasias.
The majority of lesions remain asymptomatic throughout life and are found incidentally.
- Location: they tend to be supratentorial (80% cases) but can be found anywhere including the brainstem. They are usually solitary,
although up to one-third of patients with sporadic lesions have more than one.
- Imaging Findings: MRI is the modality of choice,
demonstrating a characteristic “popcorn” or "berry" appearance with a rim of signal loss due to hemosiderin,
which demonstrates prominent blooming on T2* (GRE/SWI).
T1 and T2 signal is varied internally depending on the age of the blood produces and small fluid-fluid levels may be evident.
T2* (GRE/SWI) sequences in patients with familial or multiple cavernous angiomas are very important in identifying the number of lesions missed by other sequences (Figure 21).
Susceptibility weighted imaging (SWI) may have sensitivity equal to that of GRE in detecting these capillary telangiectasias in brain with the difference that SWI can differentiate them from calcium containing lesions.
If a recent bleed has occurred then surrounding edema may be present.
The lesions generally do not enhance,
although enhancement is possible.
DEVELOPMENTAL VENOUS ANOMALY (DVA)
- Definition: is an umbrella shaped congenital cerebral vascular malformation composed of angiogenically mature venous elements.
Dilated,
thin-walled venous channels lie within (and are separated by) normal brain parenchyma.
- Epidemiology: DVA is the most common intracranial vascular malformation,
accounting for 60% of all cerebrovascular malformations.
Estimated prevalence on contrast-enhanced MR scans ranges from 2.5-9% and are found in patients of all ages without gender predilection.
- Imaging Findings: If the DVA is small,
it may be undetectable unless contrast-enhanced scans are obtained.
CE T1WI sequences show a stellate collection of linear enhancing structures converging on the transparenchymal or subependymal collector vein.
The collector vein may show variable high-velocity signal loss.
Because flow in the venous radicles of a DVA is typically slow,
blood deoxygenates and T2* (GRE/SWI) show striking linear hypointensities (Figure 21,
12). If a DVA is mixed with a cavernous malformation,
blood products in various stages of degradation may be present and show the characteristic blooming artifact on this sequence.
CAPILLARY TELANGIECTASIA
- Definition: they are small,
low flow vascular malformations of the brain comprised of dilated capillaries and are interspersed with normal brain parenchyma with a thin endothelial lining.
- Epidemiology: Capillary telangiectasias account for 16%–20% of all intracerebral vascular malformations at autopsy and are being increasingly recognized by imaging.
Most are incidental findings,
as these malformations are nearly always asymptomatic.
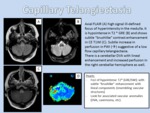
- Location: Most capillary telangiectasias are in the pons,
but they may also be found in the cerebral and cerebellar hemispheres and in the spinal cord.
- Imaging Findings: CT findings are normal in most cases but MR imaging shows capillary telangiectasia to be hypo- or isointense to brain on T1WI images.
On T2WI and FLAIR they are nearly always slightly hyperintense.
T2* (GRE/SWI) shows them to be of low signal intensity.
Macroscopic hemorrhage and calcifications are rare in capillary telangiectasia,
suggesting that the findings T2* (GRE/SWI) images are probably related to the presence of deoxyhemoglobin in the slow-flowing blood.
Capillary telangiectasias are devoid of mass effect,
and enhance faintly in a “brush like” or “stipple” pattern.
Curiously,
about two thirds of capillary telangiectasias show an enlarged vessel believed to represent a draining vein (Figure 22).
METABOLIC DISEASE
CENTRAL PONTINE MYELINOLYSIS (CPM)
- Definition: CPM is an acute de myelinating process affecting the brainstem.
- Epidemiology: It can occurred in alcoholic or malnourished patients and commonly associated with rapid correction of hyponatremiain. Additional comorbid factors include prolonged use of diuretics; liver failure; organ transplantation,
particularly liver trans plantation with cyclosporine use; and extensive burns. Patients typically present with severe electrolyte disturbances,
which lead to seizures or encephalopathy.
- Imaging findings: A symmetric trident-shaped area in the central pons is a characteristic finding on T2 and FLAIR.
The ventrolateral pons and the pontine portion of the corticospinal tracts typically are spared.
Decreased signal intensity throughout affected areas,
with no mass effect,
is a classic finding on T1-WI.
Lesions typically do not enhance after the administration of contrast material .
Restricted diffusion may be seen earlier than the classic findings in areas of osmotic demyelination on T2-WI.
Signal abnormalities also were seen within the basal ganglia,
thalami these findings are indicative of extrapontine myelinolysis.
They are typically bilateral and symmetric.
TRAUMATIC INJURY
DIFFUSE AXONAL INJURY
- Definition: Diffuse axonal injury (DAI) is a brain injury in which damage in the form of extensive lesions in white matter tracts occurs over a widespread area.
DAI is one of the most common and devastating types of traumatic brain injury and is a major cause of unconsciousness and persistent vegetative state after head trauma.
- Epidemiology: It occurs in about half of all cases of severe head trauma.
The outcome is frequently coma,
with over 90% of patients with severe DAI never regaining consciousness.
Those who do wake up often remain significantly impaired.
Most DAIs are caused by high-velocity auto accidents and are non-impact injuries resulting from the inertial forces of rotation generated by sudden changes in acceleration/deceleration resulting in axonal stretching.
- Location: The Adams and Gennarelli classification defines mild,
moderate,
and severe grades according to the location.
+ Mild: lesions are seen in the frontotemporal gray white matter interfaces.
+ Moderate: when the lobar white matter and corpus callosum are affected.
+ Severe: lesions are present in the dorsolateral midbrain and upper pons.
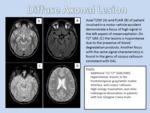
- Imaging Findings: DAI typically evolves with time,
so lesions are usually more apparent on follow-up scans.
Between 10-20% evolve to gross hemorrhages with edema and mass effect.
As most DAIs are non hemorrhagic,
T1 scans are often normal,
especially in the early stages of DAI.
T2WI and FLAIR may show hyperintense foci in the subcortical white matter and corpus callosum.
Multiple lesions are the rule,
and a combination of DAI and contusions or hematomas is very common.
T2* (GRE/SWI) scans are very sensitive to the micro bleeds of DAI and typically show multifocal ovoid and linear hypointensities (Figure 23).
SWI sequences typically demonstrate more lesions than GRE.
Residua from DAI may persist for years following the traumatic episode.
DWI may show restricted diffusion,
particularly within the corpus callosum.
DTI tractography may be useful in depicting white matter disruption.
MRS shows widespread decrease of NAA with increased Cho.