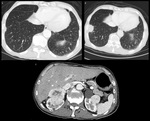
Rounded atelectasis
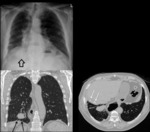
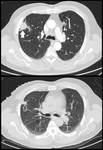
Rounded atelectasis,
also known as folded lung or Blesovsky syndrome is typically found in patients with a past history of asbestos exposure or a pleural effusion.
It is caused by infolding of redundant pleura which may give a false mass-like appearance on CT and particularly,
plain radiographs.
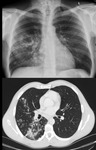
Such a ‘mass’ is almost always seen adjacent to a pleural surface; associated pleural thickening and pulling of bronchovascular bundles gives rise to the typical shape of a crow’s foot or comet tail on CT distinguishing it from malignancy (Fig 1).1
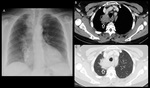
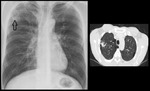
Pneumonia
Pneumonia is a common mimicker of lung cancer,
particularly when it atypically manifests as a focal opacity on a chest x-ray and/or CT.
This may lead to unnecessary investigation by CT and even PET CT with the misconception that it represents lung cancer.
The more important features favoring an infectious etiology as opposed to malignancy include presenting complaints of fever and productive cough,
acute onset of symptoms and laboratory findings such as high white cell count and raised inflammatory markers.
A recent normal chest x-ray is a useful diagnostic tool.
On cross-sectional imaging,
an enhancing consolidated lung with an air bronchogram is more suggestive of pneumonia.
Air bronchogram,
however,
may also be seen in peripheral adenocarcinoma of the lung.
An irregular outline does not distinguish between infection and tumor.
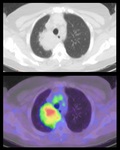
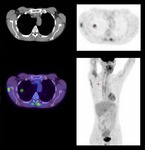
FDG-PET CT has evolved as a useful tool for oncologic diagnoses.
False positives may however arise: glycolytic metabolism is increased in the leukocytic infiltration associated with inflammatory processes resulting in elevated FDG uptake in pneumonia and abscesses,
mimicking malignancy.
Pneumonia typically causes diffuse,
relatively uniform FDG activity; however when there is cavitation of necrotic tissue,
it can be indistinguishable from cavitating neoplasms or solid neoplasms with decreased central metabolism or necrosis.
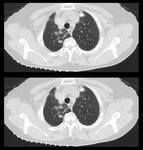
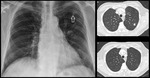
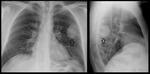
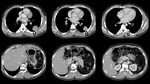
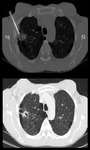
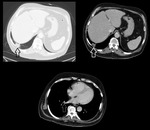
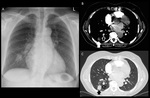
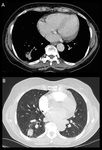
The premature use of FDG PET can therefore easily result in the misdiagnosis of malignancy.2 (Fig 2,
3 and 4)
Specific examples where pneumonia can be particularly difficult to distinguish from a tumor include lung abscess formation and a round pneumonia.
Round pneumonia is a rare benign cause of a coin lesion on chest radiography and accounts for less than 1% of coin lesions of the lung.
It typically occurs in children under the age of twelve since the lack of fully developed interalveolar pathways limits the spread of the organism leading to the typical rounded appearance.
In children,
malignancy would be unlikely to be the cause of such a lesion,
however a round pneumonia can also occur in adults (Fig 5).
Such a condition is difficult to diagnose on radiology alone and a trial of antibiotics with a repeat chest radiograph may be necessary.3-5
Cryptogenic organising pneumonia
Cryptogenic organizing pneumonia (COP),
previously termed bronchiolitis obliterans organizing pneumonia (BOOP),
is a non-infectious pneumonia which results from the organization of inflammatory exudates involving the bronchioles and alveoli resulting in the formation of intra-alveolar fibrosis and granulation tissue.
The cause is often not known (hence the term cryptogenic),
however it has often been reported as a complication of chronic inflammatory disease such as rheumatoid arthritis or as a side effect of certain medications such as amiodarone.
The condition can result in a multitude of radiologic findings on both radiography and CT.
Plain radiographs often show migratory consolidations.
However COP can,
unusually,
appear as a solitary (as seen in figure 6,
image A) or multiple lung nodules.
The most common CT findings include patchy ground-glass opacities in a subpleural and/or peribronchovascular distribution (80%) as well as bilateral basal airspace shadowing (71%).
However,
in a minority of cases,
COP may present with small nodular opacities of variable size,
as seen in figure 6,
which are typically ill-defined,
making this condition very difficult to distinguish from malignancy.
CT guided biopsy is often required in order to obtain the correct diagnosis in such cases.6-8
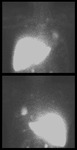
Thoracic splenosis
Ectopic splenic tissue can be congenital or acquired.
Splenosis refers to the acquired form and is defined as ‘autotransplantation of viable splenic tissue throughout different anatomic compartments of the body’ and occurs after traumatic or iatrogenic rupture of the spleen.
Thoracic splenosis has only been reported within the left hemithorax and occurs secondary to a tear or hiatus within the left hemidiaphragm allowing seeding of splenic tissue into the thorax with subsequent formation of a pleuritic mass.
Rarely,
seeding can also occur into the lung parenchyma if there is a history of lung laceration.9,10
Although this condition is benign,
it may on occasion be misdiagnosed as malignancy: cytology of splenosis reveals small and medium-sized lymphocytes which may give an impression of a lymphoproliferative disorder.
Therefore,
the best approach to diagnosing such a condition involves the use of nuclear imaging studies such as the 99mTechnetium (Tc) sulfur colloid,
indium 111-labeled platelet,
99mTc heat-damaged erythrocyte,
or 99mTc white blood cell scan.
Ferumoxide MRI is another technique which may be used to diagnose thoracic splenosis with the advantage of combining a higher spatial resolution with a physiological test of reticuloendothelial cell uptake as ferumoxide is a superparamagnetic iron oxide which is metabolized by the reticuloendothelial system.11 (Fig 7,
8,
and 9).
Aspergilloma
An aspergilloma is caused by Aspergillus infection without tissue invasion.
In patients with a preexisting lung cavity or ectatic bronchus (for a variety of reasons including pulmonary tuberculosis,
sarcoidosis or pneumoconiosis),
Aspergillus hyphae admixed with mucinous and cellular debris can colonize and grow into the cavity to form a pulmonary aspergilloma (fungus ball).
The typical appearance of an aspergilloma on CT is that of a solid,
spherical or ovoid mass with soft-tissue opacity within a lung cavity.
This can increase in size with time.
FDG-PET is often positive.
The monad sign (also known as air crescent sign or meniscus sign),
describes a sickle-shaped lucency on CT or chest radiography,
which is partially surrounding a soft tissue mass in a pulmonary cavity.
The key to diagnosis is by demonstrating that the mass is mobile,
always lying in the dependent part of the cavity,
distinguishing it from a cavitating neoplasm.12-14 These typical radiological findings may,
however,
not be present,
in which case it may be very difficult to distinguish aspergilloma from lung cancer (Fig 10,
11,
and 12).
Mycobacterium tuberculosis infection
Pulmonary tuberculosis,
among other chronic infections,
may simulate or co-exist with bronchogenic neoplasms on imaging studies.
Tuberculomas can appear mass-like and tend to be mistaken for malignancy if typical characteristics,
such as upper lobe involvement and calcification,
are absent.15 Figure 13 shows a cavitating lung mass in a smoker; this can be difficult to distinguish from a primary lung malignancy on CXR alone.
CT findings of tree-in-bud change,
caused by endobronchial inflammation,
make a diagnosis of Tuberculosis more likely.
Pulmonary embolism
Pulmonary embolism and infarction can closely mimic the radiological features of lung cancer.
Furthermore,
cytologic changes occurring in pulmonary infarctions may also produce malignant-appearing cells in respiratory secretions and needle aspiration biopsy specimens,
likely secondary to the regenerating terminal bronchioles and the alveolar lining cells occurring in the periphery of the infarcted lung.
Typically,
pulmonary infarction appears as a hump-shaped opacity with its base applied to a pleural surface,
however associated hemorrhage and edema can lead to various other shapes – including sold and cavitating mass lesions.16 Recognizing the presence of filling defects is essential in order to arrive to the correct diagnosis (Fig 14); however follow up imaging is important in equivocal cases since malignancy is a well-known risk factor for pulmonary embolism (Fig 15 and 16).
Sarcoidosis
Sarcoidosis is a multisystem inflammatory disease of unknown etiology that is characterized by non-caseating granulomas,
predominantly in the lungs and intrathoracic lymph nodes.
Chest radiography plays a central role in the diagnosis of sarcoidosis with approximately 60-70% of patients having characteristic radiographic appearances.
Radiography is also used in staging the disease depending on whether there is lymph node enlargement or pulmonary abnormalities,
or both.
Cross-sectional imaging is helpful as it is more sensitive in the detection of mediastinal lymphadenopathy and in demonstrating subtle parenchymal lung abnormalities including subpleural/peribronchovascular nodules,
fibrosis and bullae and cyst formation.17,18
Rarely,
sarcoidosis can manifest as a dominant mass-like nodularity or isolated nodules,
mimicking malignancy17.
The nature of the disease may result in a wide variety of presentations,
sometimes atypical,
which may lead the radiologist away from a diagnosis of sarcoidosis giving it its reputation as the great mimicker.
Figure 17 shows a solitary pleural nodule in right lung base that grew over a period of 5 months in a patient with large bilateral,
solid renal masses.
A tentative diagnosis of metastatic renal cell carcinoma was made on the available radiology; however,
biopsy of the pleural nodule revealed the presence of non-caseating granulomas in keeping with sarcoidosis.
The renal lesions were also eventually biopsied and both proved to be oncocytomas.