Arterial aneurism is a focal and permanent dilation of the artery greater than 50% of its normal diameter with loss of parallelism of its edges.
Abdominal aortic aneurysm (AAA) represents 60% of all arterial aneurysms.
AAA prevalence increases with age up to 7-8% of patients over 65 years old.
They are six times more common in men than in women.
The major risk factors are age,
smoking,
family history of AAA and atherosclerosis disease.
Concomitant aneurysm of the thoracic aorta is seen in 20% of cases and extension to the iliac arteries in 40% of cases.
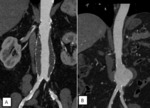
As the transverse diameter of normal abdominal aorta is around 2 cm,
we often speak of an AAA in case of a pathologic dilation of the abdominal aorta to more than 3 cm in the greatest diameter (Fig.1).
Because of its lower concentration of both elastin and vasa vasorum,
infra renal aorta is more vulnerable to aneurysm formation and infra renal aorta’s location is the most common of AAA (80% of cases).
Due to their shape,
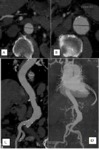
AAA are classified as fusiform aneurysm or sacuular aneurysm.
Fusiform abdominal aneurysms are most common (accounting for 80% of cases) and are due to atherosclerotic degeneration (Fig.
2).
Saccular aneurysms are less common,
are more spherical with a narrower neck,
and may be secondary to an inflammatory or infectious origin (Fig.
2).
Aneurysms are also classified as true aneurysms,
usually fusiform,
involving all three arterial layers and pseudoaneurysms,
usually saccular,
involving fewer than three walls.
In 90% of cases,
the aneurysm is due to degenerative changes of the media.
Indeed,
because of a reduction in number of elastic fibers and fragmentation of collagen fibers the aortic wall is weakened and rendered more susceptible to dilatation.
Pseudoaneurysms are often due to infectious,
post traumatic and iatrogenic conditions.
Otherwise,
AAA can be due to others causes such as:
- Aortic dissection.
- Hereditary disorders of connective tissue: Marfan syndrome,
Ehlers–Danlos syndrome (EDS).
- Systemic inflammatory diseases: Takayasu arteritis,
Behçet's disease and exceptionally giant cell arteritis (GCA).
The risk for aneurysm rupture is correlated to both the aneurysm size and rate of growth.
Therefore,
surgical repair is indicated for a larger aneurysm size than 5 cm and a rapid increase in size (aneurysms that enlarge more than 5–7 mm within 6 months or 1 cm or more within 1 year)
Nowadays,
there are two options for the treatment of AAA: conventional surgical repair and endovascular aneurysm repair.
CT angiography with three-dimensional and multiplanar reformations is the imaging modality of choice for diagnosis and pre operative assessment in patients with non complicated abdominal aortic aneurysm.
Indeed ,the choice of one or another technique is made according to aneurysm size,
measurements and anatomic informations obtained with preoperative CT angiography.