CT Protocol:
- The field of view must cover the entire aorta and the iliac axes.
- Higher concentrations (iodine,
350–370 mg/ml) of intravenous contrast material must be used to improve diagnostic accuracy.
- Rapid injection rate: the infusion rate should be at least 5 ml/sec.
- Unenhanced acquisition.
- Early arterial phase acquisition: Bolus tracking of the descending thoracic aorta,
imaging should be triggered at 200 HU with a 64-section scanner or 230–250 HU with a 128-section scanner for the early arterial phase.
- Delayed contrast enhanced acquisition.
The unenhanced acquisition enables calcification or surgical material within the aneurysm sac to be distinguished and may help depict an intramural or peri aortic hematoma.
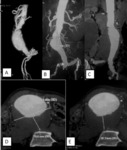
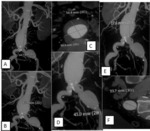
CT images processing:
Thin reconstructions and use of soft tissue filter are important enabling detailed evaluation in preoperative patients.
CT images with multiplanar reformation and three dimensional rendering techniques are the standard of care for accurate aneurysm analysis.
The size of the aneurysm and the mural thrombus are better analyzed on axial sections than on the 3D representations,
which display only the enhanced vascular lumen.
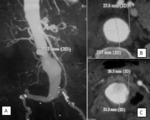
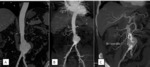
Two-dimensional MPR reconstructions (sagittal,
frontal and oblique) will be more reliable for measuring the extent of the aneurysm (Fig.3).
2D curved reconstructions allow a better study of the vascular wall and quantification of stenosis by using image processing software.
Using VR 3D reconstructions shows an anatomical view of vascular structures and allows general morphological and topographical evaluation of the arterial axis.
First of all radiologist should look for signs of of aortic instability such as the hyper attenuating crescent sign,
wall irregularity,
peri aortic hematoma adjacent to an abdominal aortic or a new saccular out pouching.
AAA size and morphology:
Axial CT images have been the reference method for aneurysms and mural thrombus measuring.
The most accurate bidimensional aneurysm measurements are diameters perpendicular to a center line through the aorta on coronal or sagittal images.
Two-dimensional MPR reconstructions (sagittal,
frontal and oblique) are used for measuring the extent of the aneurysm.
Iliac artery involvement is important to mention since it makes endovascular repair more complex.
We should specify the circulating or partially thrombosed character of the aneurysm as well as its morphology (fusiform or saccular).
Aortic Aneurysm Thrombus is classified in increments of 25%.
Aneurysm Branch Vessels: inferior mesenteric,
lumbar and accessory renal arteries.
Patency of the celiac and superior mesenteric arteries should be carefully assessed preoperatively.
Pelvic perfusion based on patency of the internal iliac arteries is also important to mention.
AAA location
An AAA is at first defined by its location relative to the renal arteries.
Suprarenal AAA involves the renal arteries and extends superiorly so that the superior mesenteric artery and celiac arteries arise from the aneurismal aorta.
Juxtarenal AAA extends to the renal arteries,
with a normal sized aorta superiorly.
Infrarenal AAA arises at least 10 mm below the renal arteries.
Aortic Neck morphology and measurements:
Aortic neck is the proximal fixation site for the stent-graft and its morphology is the most important factor in determining a successful endovascular aneurysm repair.
Proximal aortic neck diameter and length,
aortic neck calcification or thrombus,
aortic neck tortuosity index and aortic neck angle should be specified.
Proximal Aortic neck diameter:
Proximal aortic neck diameter is measured in axial plan.
A diameter greater than 28 mm is considered severe.
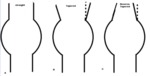
The shape of the neck may be straight,
tapered,
or reverse tapered.
(Fig.4)
Proximal Aortic Neck Calcification or Thrombus:
Aortic neck calcification or thrombus is graded by the percentage of circumferential involvement by calcification or thrombus thickness of at least 2 mm.
Proximal Aortic Neck Length:
Proximal aortic neck length is measured from the lowest renal artery to the top of the aortic aneurysm.
This measurement is important since it determinates suprarenal or infra renal fixation (Fig.5).
Proximal Aortic Neck Angle:
The aortic neck angle is drawn between the flow axis of the suprarenal aorta and the infrarenal neck.
Angles greater than 150° are most favorable and angles less than 120° are most difficult with delivering and deploying the device to the correct location.
Distal aortic neck:
Distance between the distal aortic neck and the iliac bifurcation is measured (for aneurysms that don’t extend to iliac arteries): a minimum of 15 mm is required.
Aortic Aneurysm Angle:
Aortic aneurysm angle is the most acute angle in the line through the central lumen between the lowest renal artery and the aortic bifurcation.
Measurements:
Measurements to be made included:
1 – Aortic neck diameter.
2 – Aortic neck diameter 15 mm distal to the lowest renal artery.
3 – Aortic neck length.
4 – Aneurysm diameter.
5 – Lowest renal artery to aortic bifurcation length.
6 – Aortic bifurcation diameter.
7 – Common iliac arteries diameters.
8 – External iliac arteries diameters.
9 – Lower renal to right and left internal iliac artery length
10 – Iliac arteries sealing lengths
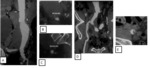
Iliac and common femoral artery:
The morphology of the iliac and common femoral arteries is important.
Iliac and common femoral arteries calcification,
diameter,
tortuosity ,
angle and length have to be mentioned (Fig.
6,7).
Stenotic or occlusive disease is also to mention.
A minimal outer diameter of 7 mm is usually needed.
Anatomic variants to mention:
Accessory renal arteries: number,
location and course (Fig.
8).
Kidney and renal vein variants: horseshoe kidney,
multiple renal veins,
retroaortic left renal vein,
circumaortic left renal vein.
Vena cava variants: double inferior vena cava,
left inferior vena cava.