For the purpose of our study,
cross-sectional imaging of treated Head and Neck malignancies was used,
comprising of CT and MR acquired from May 2013 until May 2015.
128 slice CT or 4 slice CT and 1.5 T MR were used.
Most of the patients (77%) included in the study were histopathologicaly proven oropharyngeal and laryngeal malignancies (mostly SCC).
Then nasopharyngeal carcinoma (9%),
adenocarcinomas (4%) and thyroid cancers (2%) followed.
The imaged changes of the tissue were classified into 2 groups: early (in the first 6 months after treatment),
and late changes (more than a year after treatment).
In the early post-treatment period patients showed up with:
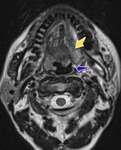
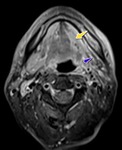
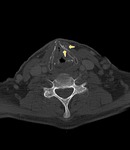
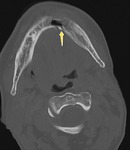
1. Iatrogenic asymmetry of the normal anatomy (particularly at the place of anastomosis/reconstruction where asymmetric thickness of mucosa could be seen),
Figure 1-2.
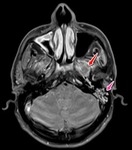
Early fibrose and granulomatose tissue is most prominent and simulates a mass in the early post-treatment period (Figure 3-5) especially in the patients with definitive radiotherapy,
where the conventional 6 month follow up can be misdirecting;
2. Inflammation due to iatrogenic infection Figure 6-8,
dehiscence Figure 9-11 or post radiotherapy seroma/abscess Figure 12.
(This was also mostly seen at the places of anastomosis or surgical approach);
3. Inflammation of congenital anomalies (brachial cyst,
thyroglossal cyst,
cystic hygroma/lymphangioma) (Figure 13-18).
This places are considered as focal points for developing infective or noninfective inflammations,
and oncologicaly treated patients are more prone to present with such findings due to vascular insufficiency and reactive inflammation.
Difficult to discern from direct spread (Figure 19-20) or cystic malignant lymph nodes (Figure 20-21),
early follow up (2-4 weeks) and clinical info can be most helpful.
The patients in the late post-treatment period showed up with the following findings:
1. The developed asymmetry is better defined,
and can easily be discerned from recurrence;
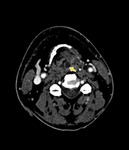
2. Inflammation of the chondroid and bone that were in the zone of radiotherapy,
resulting in osteonecrosis and chondronecrosis.
Usually this group of patients underwent a previous surgical/dental procedure or were treated with bisphosphonates (Figure 23-28) ;
3. Inflammation of congenital anomalies were rare in this group of patients;
4. Extensive fibrosis and desmoplastic changes (Figure 29-31)were equally present in the late post-treatment period obscuring the normal and pathologic tissues thus lowering the sensitivity of conventional imaging.
In our study as clinically significant early radiology mimicker presented seromatose,
limphocele or inflammatory activation of congenital anomalies while fat stranding and homogenous linear enlargement of the fascia and mucosa resulted in inconclusive reports.
The late mimickers that resulted in false positive or false negative,
included desmoplastic changes,
chondronecrosis and osteonecrosis.