Anatomy

Fig. 1: Diagram representing extensor tendons, tendon sheaths and retinacula.
Tibialis anterior muscle
The tibialis anterior muscle is part of the extensor (anterior) compartment of the leg,
arising in the lateral condyle of the tibia,
proximal lateral tibial shaft,
anterior surface of the interosseous membrane,
deep surface of the fascia cruris and intermuscular septum [1].
Its functions are dorsiflexion,
adduction and inversion of the foot.
It is innervated by the deep peroneal nerve.
Tibialis anterior tendon
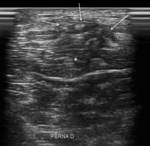
The tibialis anterior tendon Fig. 1 Fig. 2 courses inferiorly and inserts with two bands of variable width on the first metatarsal base and the medial cuneiform bone. It is the most medial tendon of the extensor tendons of the ankle,
and is covered anteriorly by the extensor retinaculum.
The synovial tendon sheath of the tibialis anterior extends from above the proximal arm of the inferior extensor retinaculum to the level of the talonavicular joint [2].

Fig. 2: MR image PD weighted with fat saturation just above the ankle showing normal regional anatomy of the tendons.
Bursa
The main synovial bursa can be found in between the tendon and the cuneo-metatarsal joint / medial cuneiform - tibialis anterior subtendinous bursa Fig. 1.
Extensor retinaculum
The extensor retinaculum comprehends two components: superior and inferior.
The superior extensor retinaculum covers the extensor tendons in the distal leg / proximal ankle,
inserting laterally in the distal fibular lateral crest / lateral malleolus,
and medially in the anterior crest of the distal tibia / medial malleolus.
The inferior extensor retinaculum has four components arranged in a "Y" shape: the stem / frondiform ligament,
the oblique superomedial limb,
the oblique inferomedial limb and the oblique superolateral limb [3].
Lateral insertions involve the tarsal sinus and canal,
and medial insertions involve the medial malleolus superiorly and the cuneonavicular joint inferiorly.
Muscle disorders
Muscle herniation
Trauma,
especially of the penetrating type can disrupt the fascial layers,
allowing muscle belly to herniate into the subcutaneous tissue.
Other causes include areas of fascial weakness due to perforating vessels,
occupational activities and sports which stress the lower leg muscles and chronic compartment syndrome.
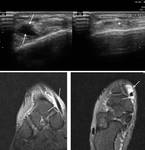
Ultrasound and MR show a fascial defect through which there is muscle tissue herniation,
after provocative maneuvers Fig. 3 Fig. 4 .
Dynamic assessment in ultrasound evaluation is most useful for diagnosis.
It is important to create as little pressure as possible with the ultrasound probe in order to facilitate herniation during dynamic assessment Fig. 5 .

Fig. 5: Video 1 - Ultrasound examination showing dynamic assessment (muscle contraction and relaxation) of tibialis anterior herniation.
Atrophy
Muscle atrophy can occur in several conditions,
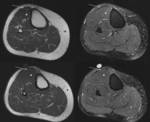
such as neuromuscular disorders and any kind of lesion to the peroneal nerve Fig. 6 which motivates muscle denervation.
It also occurs in a generalized manner due to underuse,
for example in bed-laden patients.
Ultrasound shows hyperechogenicity of the muscle tissue,
as well as an apparent loss of muscle volume.
MR shows variable signal hyperintensity on T1 weighted imaging,
due to fat infiltration.
Vascular malformation
These are congenital lesions,
sometimes asymptomatic but may cause discomfort.
Asymptomatic lesions do not require therapy,
unless for cosmetic reasons.
Ultrasound shows an intramuscular heterogeneous lesion,
sometimes with dilated vessels inside.
Phlebolits can be present,
identified as echogenic foci with acoustic shadowing.
Doppler is most useful,
confirming the vascular nature of the lesion Fig. 7 .
MR also shows a heterogeneous lesion,
usually hypo- or isointense at T1 weighted and high signal intensity at T2 weighted imaging Fig. 8 .
T2 weighted images usually better depict the lesions contours and relation to adjacent structures.
Gadolinium enhanced T1 weighted imaging can be useful for demonstrating the vascular enhancement of the lesion.

Fig. 7: Ultrasound evaluation of tibialis anterior vascular malformation - There is an intramuscular heterogeneous lesion (white arrows). Compare with the contralateral normal muscle echostructure (asterisk).
On the right, Doppler ultrasound shows numerous vessels in the lesion (yellow arrow).

Fig. 8: MR evaluation of tibialis anterior vascular malformation - There is an heterogeneous intramuscular lesion (white arrows), showing high signal intensity on T2 weighted imaging with fat saturation (upper images) and slightly higher signal intensity than muscle tissue on T1 weighted imaging (lower images). The high singal intensity on T2 is due to the slow flow in the vessels of the lesion.
Tendon abnormalities
Tendinosis
Seen less frequently than other tendinopathies around the ankle,
tibialis anterior tendinosis is predominantely found in overweight women of 50-70 years of age [4].
Clinically,
there is pain on the medial side of the midfoot,
exacerbated by dorsiflexion of the foot,
passive tendon tension or by palpation of the insertion point.
Ultrasound findings are similar to tendinosis in other sites of the body,
consisting of tendon thickening,
hypoechogenicity and heterogeneity Fig. 9 Fig. 10 .
There is usually increased vascularization of the tendon and the surrounding tissue,
and tendon tears are also a possible finding.
MR also shows tendon thickening,
heterogeneity and increased signal intensity in fluid-sensitive sequences,
such as STIR ,
T2 or PD,
preferably with fat saturation Fig. 11 .
It is important to keep in mind that subtendinous bursitis or tenosynovitis can also be associated findings.

Fig. 9: Ultrasound evaluation of tibialis anterior tendinosis - note the tendon thickening and hypoechogenicity (arrows), compared to the contralateral normal tendon (interrupted arrows).
Doppler ultrasound on the lower image shows slightly increase peri-tendon vascularity (arrowhead).

Fig. 11: MR images of tibialis anterior tendinosis - PD (upper left) and PD with fat saturation (upper right and lower images). There is thickening and hypersignal of the tibialis anterior tendon (arrows). There is also a small partial rupture of the tendon, noted by higher signal intensity in the center of the tendon, similar to fluid signal.
Tenosynovitis
Clinically difficult to differentiate from tendinosis,
this condition is diagnosed by typical imaging findings of tendon sheath thickening and fluid distention involving the tendon,
clearly seen on ultrasound and MR Fig. 12 Fig. 13 .
Peritendinous edema is also seen sometimes.
Conservative therapy is usually successful.
Penetrating trauma involving the tendon sheath is infrequent,
but a possible cause for tenosynovitis Fig. 14 ,
occasionally infectious in origin.
Clinical history along with image proven tendon sheath disruption are diagnostic.

Fig. 12: Ultrasound evaluation of tibialis anterior tenosynovitis - there is synovial sheath thickening (blue arrows) and synovial fluid distension (white arrows) surrounding the tendon (asterisks). Compare these findings to the contralateral normal synovial sheath (arrowheads).
Lower images of Doppler evaluation show increased synovial sheath vascularity (yellow arrows).

Fig. 13: MR evaluation of tibialis anterior tenosynovitis - There is fluid distenion involving the full circumference of the tibialis anterior tendon (white arrows). Note the normal tendon just proximal to its insertion (yellow arrow).
Tendon tear
These occur quite infrequently,
and the diagnosis is sometimes delayed.
Tears can be full or partial thickness,
and traumatic or spontaneous in origin.
Spontaneous tears are usually caused by repeated microtrauma on a weakened tendon in middle-aged and older patients,
and are frequently well tolerated.
Normal aging is associated with a decrease in tendon strength,
and other causes for decreased tendon strenght include corticosteroid use,
Diabetes Mellitus,
hyperparathyroidism and gout [5].
Traumatic tears are caused by local blunt or penetrating trauma,
usually requiring surgical intervention.
Clinically,
there is evidence of tendon retraction with a soft tissue mass arising in the anterior lower leg after muscle contraction,
in cases of full-thickness tears.
Partial thickness tears are clinically similar to tendinosis (which may also coexist).
Typical imaging findings of tendon disruption,
seen on ultrasound or MR as fluid-like echogenicity / signal,
are diagnostic Fig. 10 Fig. 11 Fig. 15 .
Dynamic assessment during ultrasound evaluation is quite useful for determining tendon retraction as the cause for the clinically evident soft tissue mass in cases of full thickness tears.
Fluid distension of the tendon sheath is a frequently associated finding.

Fig. 15: Tibialis anterior full-thickess tear - on the left, note the radiographic appearance of a soft-tissue swelling anterior to the distal tibia (white arrows). MR images (T1 weighted and T2 weighted with fat saturation) show the soft tissue mass to correspond to the retracted tendon (blue arrows) and fluid (red arrows). There is complete tendon disruption, confirming full-thickness tear.
Bursal pathology
Subtendinous bursitis
This condition is clinically difficult do diagnose,
as it mimics several peri-articular and muscle lesions.
However,
imaging findings of bursal fluid distension should make for a clear diagnosis Fig. 16 .
Note that the subtendinous location of the bursa and a partial inferior fluid involvement of the tendon are key for differentiating from tenosynovitis.

Fig. 16: Tibialis anterior subtendinous bursitis - Note fluid distension only partially involing the tendon (white arrows), in its distal portion, compared to the contralateral normal tendon (asterisk). This partial involvement is necessary to differentiate from tenosynovitis.