INDICATIONS
- Wide neck Saccular aneurysms (fundus-to-neck ratio > 2 or neck diameter > 4mm)
- Fusiform or circunferential aneurysms
- Dissecting aneurysms
- Blister-like aneurysms
- Large (10-25 mm) and Giant aneurysms (≥ 25 mm) or those presenting with mass effect
- Incorporation of side branches
- Post-treatment recanalization
- Incomplete coiling and reperfusion of the aneurysm
- Recurrent aneurysm
- In very small aneurysm untreatable by standard coiling technique
INTERVENTIONAL METHOD
Transfemoral approach with the patient under general anesthesia.
Guiding catheter was introduced through a femoral sheath into the carotid or vertebral artery.
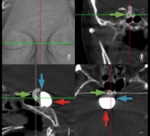
Radiologic examination of the target vessel is performed by using a biplane angiographic system and 3D rotational angiography.
Flow diverter length was chosen according to the length of the aneurysm neck with the procedural goal to ensure arterial wall coverage with the inner mesh extending to at least 2 mm beyond both the distal and proximal limits of the neck.
For flow diverter delivery,
a microcatheter is navigated past the aneurysm neck with a microguidewire or radiofocus guide wire.
Under roadmap guidance,
unsheath the flow diverter by slowly withdrawing the delivery microcatheter for 2–3 minutes while the delivery wire is gently pushed on to facilitate complete opening and wall apposition of the flow diverter.
An in-stent percutaneous transluminal angioplasty is performed with a balloon microcatheter if incomplete opening is observed on 2D angiography or 3D.
In those cases in which additional aneurysm coiling is performed,
a microcatheter is initially positioned inside the aneurysmal sac followed by jailing of the microcatheter between the parent vessel wall and the flow diverter at deployment.
ANTICOAGULATION AND ANTIPLATELET THERAPY
Patients are prepared; with aspirin,
100 mg,
and clopidogrel,
75 mg (loading dose of 300 mg),
5 days before treatment.
During the procedure; anticoagulation is initiated with a bolus of standard heparin (70 –100 IU/kg) followed by intravenous administration to maintain an activated clotting time of standard heparin (70 –100 IU/kg) followed by intravenous administration to maintain an activated clotting time of standard heparin (70 - 100 IU/kg) followed by intravenous administration to maintain in activated clotting time of 250 seconds.
After the procedure; a daily dose of clopidrogrel (75 mg) and aspirin (100mg) is given for 3 and 6 months,
respectively.
Platelet inhibition is tested by using the light transmission aggregometry (LTA) method on the day before or inmediately before starting the procedure.
- If according to this test,
the patient is considered a non-responder (LTA result of 6),
an LTA test with 2-MeS-AMP (selective P2Y12-adenosine diphosphate receptor antagonist) is performed.
- In cae of an LTA result with 2-MeS-AMP 5,
a pharmacokinetic response is suspected and a reloading dose of clopidrogrel (300 mg) is administered.
- In the case of repeated tet failure even after reloading or an LTA result with 2-MeS-AMP 5,
pharmacodynamic resistance is assumed and prasugrel is sibstituted for clopidogrel.
Patient with ruptured aneurysms,
tirofiban is administrated intravenously during the endovascular procedure before FD deployment and aspirin and clopidogrel are started after the procedure.
FOLLOW UP
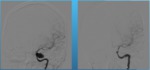
Detailed follow-up examinations were performed with both DSA (Digital subtraction angiography) and MRI imaging at 3 months.
After 6 months,
MRI was exclusively performed.
To evaluate thrombosis of the aneurysm and shrinkage of the aneurysm sac,
measure the maximum diameters of all lesions on preprocedural MRI images in the axial plane with 2 additional orthogonal planes and compare them with MR imaging at 3 and 6 months.
Aneurysm morphometry on MR imaging categorized into 3 groups:
1) complete or partial decrease
2) stable
3) progressive
COMLICATIONS
Peri-procedural death or major stroke
Hemorrhages
- Early aneurysm rupture during the latency period or post treatment delayed ruptures.
- Intracerebral hemorrhages
Thromboembolic complications
- Ischemic stroke
- Occlusion of perforating arteries or other side branches,
with secondary ischemic complications.
Minor neurologic complications
- Transient ischemic attack
- Small cerebral infarction
- Cranial nerve palsy
Late complications are usually related to device occlusion,
although exceptionally delayed hemorrhages have been observed up to 5 months after flow diversion.
Technical complications included inadequate device opposition against the parent artery wall,
a factor that may predispose to device thrombosis or late stenosis,
and proximal migration of the device with subsequent “diversion” of flow within the aneurysm with resultant delayed rupture.