1- Computed tomography imaging protocol
We use a General electric 64 slices VCT machine.
The exams are aquired with the following imaging parameters: 120 kV, 250 mAs,
collimation 0.5 mm or 0.625 mm,
scan time 1s.
After acquiring,
the raw dataset images are reconstructed with a slice thickness of 1 mm ,
by using an ultra high resolution reconstruction mode.
The reconstructions of the axial images are made in a plane parallel to the lateral semicircular canal.
The coronal imaging set is reconstructed exactly perpendicular to this axial set of images
Images are viewed using a window width of 4000 HU and a window level of 400 to 800 HU.
2-Magnetic resonance imaging protocol
We use a 3-T MR imaging system " Siemens Magnetom verio 3T" .
A thin-section gradient-echo sequence that is heavily T2 weighted is best suited for evaluation of the fluid-filled spaces of the membranous labyrinth and the eighth cranial nerve (T2 CISS 3D).
Axial and coronal T2 and T1 weighted sequences before and after gadolinium injection are also performed to study the signal and to search an enhancement of the labyrintic structurs.
Routine axial T2-weighted and T1-weighted enhanced imaging of the brain is performed in all patients.
3-Normal anatomy of the inner ear
The anatomy of the temporal bone is complicated.
The most important featuers of the inner ear will be described (1).
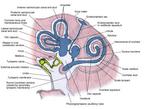
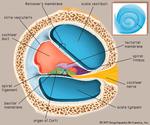
The inner ear consists of an osseous labyrinth that encloses a membranous labyrinth(fig1).
The osseous labyrinth consists of the vestibule,
cochlea,
semicircular canals,
vestibular aqueduct,
and cochlear aqueduct .
The space between the osseous labyrinth and membranous labyrinth is filled with a fluid known as perilymph.
A similar fluid (endolymph) fills the space within the membranous labyrinth.
-The vestibule: is the central,
rounded portion of the osseous labyrinth.
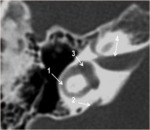
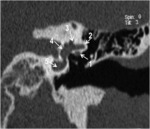
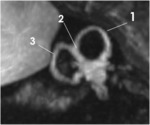
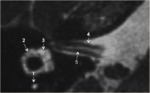
It is continuous anteroinferiorly with the cochlea and posteriorly with the semicircular canals and the vestibular aqueduct (fig2,3).
The vestibule contains the utricle and the saccule,
which are integral components of the membranous labyrinth.
There are never physiological calcifications on the vestibule and its size is considered pathological to a minor axis> 3.8 mm and a major axis> 6.9 mm.
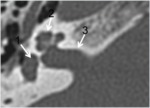
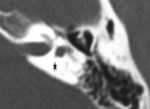
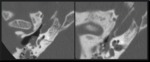
-The vestibular aqueduct: is a tubular structure that arises from the vestibule and runs along the posteroinferior aspect of the petrous temporal bone (fig2).
It contains the endolymphatic duct and sac,
which are connected to the utricle and saccule of the vestibule.The aqueduct,
which normally measures less than 1.5 mm in diameter,
approximates the size of the posterior semicircular canal,
which runs anterior and parallel to the aqueduct.
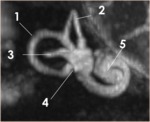
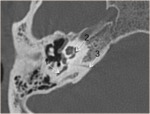
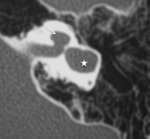
-The semicircular canals: they are named as lateral,
posterior and superior semicircular canals (fig4).
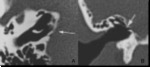
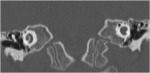
The posterior end of the superior semicircular canal joins the upper end of the posterior semicircular canal to form a common limb known as the common crus (fig5).
-The cochlea (fig 6) consists of a canal that spirals from 2 and1/2 to 2 and ¾ times around a central cloumn of bone (the modiolus).
A delicate osseous spiral lamina that projects from the modiolus divides the cochlear canal into an upper compartment (scala vestibuli) and a lower compartment (scala tympani).These two compartments communicate through an opening called the helicotrema,
at the cochlear apex (fig 7).
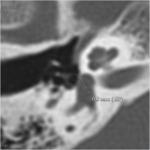
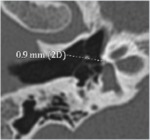
-The cochlear aqueduct (fig8) goes from the basal turn of the cochlea to the superior part of internal jugular fossa .It provides a communication between the subarachnoid spaces and the perilymph and is incriminated in the diffusion of bacterial meningitis to the labyrintheThe diameter of the cochlear aqueduct is important to precise.
When inferiour to 1.6 mm or superior to 3 mm it must be considered as patent.
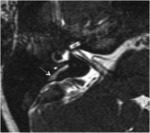
-The inner auditoy canal (IAC) extends from the labyrinth to the cerebellopntine angle and contains the seventh and the eighth cranial nerves (fig 9).
-The eighth nerve (vestibulo cochlear nerve): is composed of three branches (FIG10):
-The superior and inferior vestibular branches of the nerve: occupy the postero-superior and postero-inferior quadrants of the IAC respectively.
-the cochlear branch: located in the antero-inferior quadrant.
-The facial nerve (seventh nerve): occupies the antero-superior part of the IAC.
4-Labyrinthic pathologies
a-Congenital malformations of the inner ear :
Congenital inner ear abnormalities is a major cause of hearing loss in children.
CT temporal bone imging is the modality of choice in the investigation of hearing loss but high-resolution MR imaging is used to study the membranous labyrinth and eighth cranial nerve. An MR imaging examination of the brain,
if performed at the same time as the inner ear examination,
offers the advantage of allowing the evaluation of any coexistent brain parenchymal abnormalities (2).
The calssification of Jackler et al (3) which is based on a liner developmental modal towards normal anatomy and the most likely time at which developmental arrest occurs during enbyogenesis is the most commonly used.
-Michel aplasia :
Most sever form of inner ear deformity caused by evelopmental arrest of otic placod early during the third week of gestational age.
It consists on complete absence of inner ear structures (fig 11).
In patients with unilateral complete labyrinthine aplasia,
the contralateral inner ear structures are often dysplastic and many lesions may be associated (Hypoplasia of the petrous bone ,absence of the round and oval windows,
skull base and vascular anomalies,
anomalous courses of the facial nerve).
-Cochlear aplasia :
Cochlear aplasia,
or complete absence of the cochlea is due to arrested development of the inner ear in the later part of the 3rd week of gestation.
It is a rare anomaly.
the vestibule and semicircular canals are often malformed but may be normal and dense otic bone is present at the site where the cochlea would be normally.
-Common cavity :
The arrest of development occurs at the fouth week of gestation and is defined as a single cavity that represents the undifferentiated cochlea and vestibule.
-Incomplete partition I : (cystic cochleovestibular malformations)
The arrest of development happens at the fifth week of gestation.The cochlea has no bony modiolus and appears us an empty cystic cochlea.
This deformitie is accompanied by a dilated cystic vestibule (fig12).
-Cochlear Hypoplasia :
Failure of cochlea development late in the sixth week of gestation.
This abnormality accounts for 15% of cochlear malformations.
Although the cochlea is visible,
it has only one turn or a partial turn (fig13).
A small cochlear bud of variable length (usually 1–3 mm) is seen protruding from the vestibule ,
and an abnormally small IAC may be seen.
The vestibule and semicircular canals are usually malformed but may be normal.
-Incomplete partition II: (Mondini deformity)
It is the most common type of cochlear malformation which accounting for more than 50% of all cochlear deformities.
it is caused by developmental arrest that occurs at the seventh week of gestation.
The cochlea consists of 1 and a half turns and the interscalar septum and osseous spiral lamina are absent.
The basal cochlear turn appears normal,
but the middle and apical turns coalesce to form a cystic apex.
The modiolus is present only at the level of the basal turn.
This deformity is often associated with an enlarged vestibular aqueduct.
-Semicircular canal abnormalities :
The semicircular canals develop at 6 to 8 weeks gestation and are completed between the 19th and 22nd weeks.
The semicricular canals can either be absent,
hypoplastic or enlarged.
-Enlarged vestibular aqueduct :
This deformity is the result of a developmental anomaly in the 7th week of gestation but in some cases,
the malformation may actually be acquired and not congenital.
It consists on a vestibular aqueduct that having a width larger than with 1.5 mm measured midway between the common crus and the external aperture (fig14).
It is the most frequent CT or MR imaging finding in patients with early-onset sensorineural hearing loss.
The abnormality is bilateral in as many as 90% of cases but may be asymmetric,
and is slightly more frequent in females.
Cochlear abnormalities are associated in most cases (76%).
b-Otodystrophic pathology : Osteosclerosis
Otosclerosis or otospongiosis is a unique autosomal dominant otodystrophy of the otic capsule.
it is characterised by replacement of the normal ivory-like enchondral bone by spongy vascular bone(4).
It a causes a conductive,
mixed or sensorineural hearing loss in the 2nd to 4th decades of life.
Pre-operative high-resolution CT imaging is mandatory to confirm the diagnosis ,
to evaluate the extent of the disease and t detect potential causes of operative failure such as disease extension to the round window and abnormal ossicular chain morphology.
The Veillon classification is used to evaluate the extent of the desease (5).
Stage 1 :
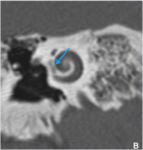
1a footplate thikened >0,6 mm (fig15).
1b prestapedienne hypodenstity < 1mm (fig16).
Stage 2 :
prestapedienne hypodenstity > 1mm
Stage 3 :
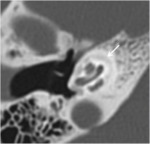
Prestapedienne hypodensity> 1 mm, hypodensity extends to the endosteum of cochlea.(fig17)
Stage 4 :
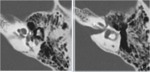
4a: Hypodense foci in the entire middle layer of the otic capsule: pericochlear hypodensity,
internal auditory canal hypodensity (fig 18).
4b: Involvement of the entire otic capsule including the vestibule and semicircular canals (fig19)
c-Inflammatory pathology : Labyrinthitis
Labyrinthitis is an inflammatory disorder of the inner ear.
May affect one or both ears.
It can be a cause of vertigo and hearloss.
The aetiology of labyrinthitis appear to be viral,
bacterial ,
autoimmune and can be associated with cochlear trauma,
vertebrobasilar ischaemia,
meningitis,
Ménière’s disease and medication (aminoglycoside) .
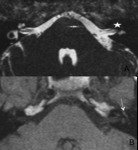
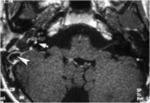
The role of the CT is actually very limited and the diagnosis is based on MRI images where T2 weighted images shows an amputation of the normal labyrinthic signal and T1 weighted images shows an enhancement of the labyrintic sryctures due to gadolinium accumulation on the membranous labyrinth caused by breakdown of the blood perilymph barrier (6) (fig20,
21).
The healing process may lead to a labyrinthine ossification (fig 22).
d-Tumoral pathology of the inner ear :
-Intralabyrinthine schwannomas :
Intralabyrinthine schwannomas are defined as tumours arising primarily from the terminal vestibulo-cochlear nerve within the membranous labyrinth in the cochlear,
vestibule,
or semicircular canals(7)
MRI represents the modality of choice for the diagnosis and the follow up of intra labyrinthine schannomas.
This lesion appears on T2-weighted images as a sharp focal filling defect replacing the normal high-signal intensity of the intralabyrinthine fluid that enhances intensely and homogeneously on T1- weighted enhanced images (fig 23).
The most important differential diagnosis for intra labyrinthine schannomas is labyrinthitis.
On MRI,
labyrinthitis enhances diffusely,
involving the complete cochlear or vestibular system (fig 20,21),
no focal filling defects will be seen in T2-weighted images and the enhancement may also disappear on follow-up imaging.
-Intravestibular lipoma
Intravestibular lipoma is a rare congenital lesion that is often associated with lipoma in the cerebellopontine angle (8).
The imaging diagnosis of intravestibular lipoma consists of a nonenhancing intravestibular lesion that is hyperintense on T1-weighted images and suppresses completely with fat saturation.
The differential diagnosis ar the other sources for hyperintensity within the vestibule on T1-weighted images including hemorrhage or highly proteinaceous fluid That are easily differentiated from a lipoma because of their lack of signal intensity suppression with fat saturation.
e-Traumatic injuries of the inner ear :
Temporal bone fractures are mostely a result of high-energy blunt head trauma.
Multidetector CT with MPR is a fundamental tool for determining the extent of injuries.
MRI is useful for identifying vestibular hemorrhage (fig24),
determining the extent of brainstem injury,
and demonstrating nerve compression.
There is many classifications of the temporal bone (9) .The traditional classification system indicates the relationship of the fracture line with the long axis of the petrous portion of the temporal and classify temporal bone fractures as transverse or longitudinal .
Brodie et al (10) described a classification of temporal bone fractures on the basis of whether the otic capsule is involved or spared and they discribe otic capsule violiting and otic capsule sparing fractures (fig 25).
When the fracture course is through the labyrinth (the cochlea,
vestibule,
or semicircular canals) it’s often associated with complications such as sensorineural hearing loss,
cerebrospinal fluid otorrhea,
and facial nerve injury (11).