This poster is published under an
open license. Please read the
disclaimer for further details.
Keywords:
Interventional vascular, Neuroradiology brain, Catheter arteriography, MR-Angiography, MR, Catheters, Aneurysms
Authors:
M. Zaitoun; Zagazig/EG
DOI:
10.1594/ecr2016/C-2019
Results
Immediate Anatomical Results:
All aneurysms were successfully treated through endovascular coil embolization using simple coiling technique and multiple microcatheters technique.
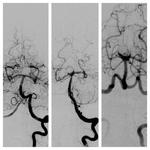
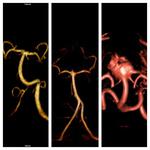
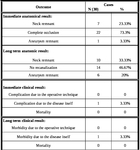
As shown in Table (2) and Figure (3),
the immediate anatomical results showed complete occlusion in 22 aneurysms (73.34%).
Immediate Clinical Results:
As shown in Table (2),
2 cases (6.67%) showed thromboembolic events intraoperatively treated with eptifibatide with no clinical impact.
These 2 aneurysms were of wide neck and were treated with multiple microcatheter technique.
1 case (3.33%) treated by simple coiling showed vasospasm with subsequent cerebral infarction,
this patient with big probably dissecting basilar tip aneurysm presented with bleeding and brainstem ischemia and although the patient developed subsequently a small right fronto-opercular ischemia due to vasospasm,
his morbidity was linked to the brainstem presenting infarction .
No morbidity or mortality was related to the operative technique.
Longterm Anatomical Results:
As shown in Table (2) and Figure (4),
the longterm anatomical results in the follow-up (mean 33.6 months) showed no recanalization in 14 aneurysms (46.67%),
neck remnant in 10 aneurysms (33.33%) and aneurysm remnant in 6 aneurysms (20%).
Five aneurysms (16.67%) were re-embolized,
3 of them (60%) were due to regrowth and the other 2 (40%) were due to coil compaction.
Four of them (80%) were aneurysms of wide neck with only one (20%) was being completely occluded.
Longterm Clinical Results:
As shown in Table (2),
1 case (3.33%) showed moderate disability due to the presenting brainstem infarction and not related to the operative technique and 29 cases (96.67%) were clinically intact.
No mortality.
In our results,
we found significant correlation (p-value=0.039) between the aneurysm neck size and the immediate anatomical results namely,
the larger the aneurysm neck size,
the more likely the neck remnant and aneurysm remnant after embolization.
There were no significant correlation between the outcomes (clinical & anatomical) and techniques of embolization and no significant correlation between the outcomes (clinical & anatomical) and history of aneurysm rupture.