This poster is published under an
open license. Please read the
disclaimer for further details.
Keywords:
Thorax, Computer applications, Radioprotection / Radiation dose, CT, Comparative studies, Computer Applications-Detection, diagnosis, Technology assessment, Image registration, Image verification
Authors:
M. Ohana1, A. Labani1, M.-Y. Jeung1, C. Ludes1, C. Roy1, C. Collet2, F. Heitz2, F. Rousseau2, V. Noblet2; 1Strasbourg/FR, 2Illkirch/FR
DOI:
10.1594/ecr2016/C-2126
Methods and materials
ULD CT examinations
25 normal or subnormal examinations were selected by one chest radiologist from a previous IRB-approved prospective study.
All 25 patients underwent two successive unenhanced chest CT acquisitions on a second-generation 320-row scanner (Aquilion One Vision Edition,
Toshiba Medical Systems,
Japan) with:
- one standard "full dose" acquisition: 120kV and auto-mA (80-700)
- one ULD acquisition: 135kV and 10mA
- both acquired with a pitch of 0.813,
a tube rotation of 0.275sec,
a collimation of 0.5*80mm and reconstructed at a slice-thickness of 1mm every 0.8mm with a lung kernel and an iterative algorithm (AIDR-3D set in standard mode).
Post-processing
Standard-dose and ULD DICOM images were elastically registered using a validated non-rigid diffeomorphic registration algorithm (ANTs -  Advanced Normalization Tools).
The full dose examination was registered over the ULD one.
Advanced Normalization Tools).
The full dose examination was registered over the ULD one.
An advanced image-domain denoising process (Non-Local Means,
NLM) was applied to the ULD acquisitions,
using 3x3x3 patch,
15x15x15 searching window and 7 levels of denoising strength (β coefficient varying from 0.1 to 10: β0.1,
β0.5,
β1,
β1.5,
β2,
β5 and β10).
Mean computational time for each denoised set was around 30 minutes on a 24-cores server.
Image evaluation
Quantitative evaluation was done by pixel-to-pixel comparison to the registered standard-dose acquisition,
with computation of the peak signal-to-noise ratio (PSNR).
Qualitative evaluation was blindly and independently performed by two senior chest radiologists,
with subjective ranking of all ULD examinations (the original and the 7 denoised ones) for each 25 patients,
starting from a random order.

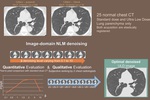
Fig. 2: Flowchart of the study design