This poster is published under an
open license. Please read the
disclaimer for further details.
Keywords:
Vascular, MR-Angiography, MR, Embolisation
Authors:
N. K. Majewska, A. Kociemba, M. Pyda, M. Wykretowicz, M. Stajgis, K. Katulska; Poznan/PL
DOI:
10.1594/ecr2016/C-2297
Methods and materials
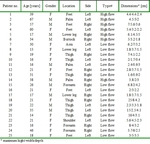
We evaluated data for 25 consecutive patients with diagnosed vascular malformations who were examined in our MRI faculty between January 2011 and December 2013.
A detailed description of the study group is given in Table 2.
On the basis of selective digital subtraction angiography (DSA) examinations and patient clinical data (including color doppler imaging results),
malformations were divided into two groups: high flow and low flow.
MR imaging Technique
The MR examinations were performed on a 1.5-T scanner.
The study protocol consisted of T1-weighted,
turbo spin-echo (SE) imaging,
volume interpolated breath-hold examination (VIBE) with fat saturation,
short τ inversion recovery (STIR),
and contrast-enhanced angiography (time-resolved angiography with interleaved stochastic trajectories; TWIST).
T1-weighted,
VIBE,
and STIR imaging was performed prior to the administration of contrast agent in two orthogonal planes.
TWIST was performed after the administration of contrast agent (0.1 mmol/kg).
The injection rate,
using a power injector,
was 3.5 mL/s and the injection of contrast agent was followed immediately by a 20-mL saline flush administered at the same rate.
To obtain delayed venous phase scans,
we used 28 consecutive measurements.
The temporal resolution,
and consequently overall angiography time,
depended on the size and location of the lesion and varied between 3 and 4.5 s and between 84 and 126 s,
respectively.
T1-weighted imaging and VIBE sequences were repeated after administration of the contrast agent.
Two observers independently reviewed the images for each patient.
The observers were blinded to the clinical data,
as well as to the results of other imaging modalities.
MR Image Analysis
Each malformation was evaluated on the basis of T1- and T2-weighted imaging.
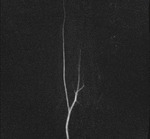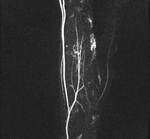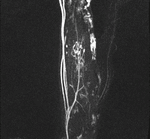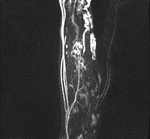
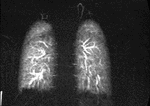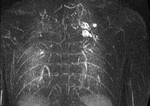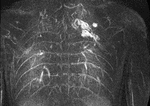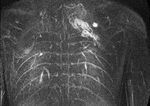
MIP images generated from the time-resolved MR angiography images were used for further analysis (Fig.
1,2).
Each malformation was contoured on the MIP image where it had the largest dimensions.
The region of interest (ROI) was copied to all other MIP images and the mean signal intensity was measured.
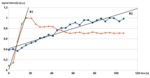
Next,
we plotted signal intensity versus scanning time (MIP image number).
The signal enhancement curves were analyzed to determine the time of maximum lesion enhancement,
the artery–lesion time,
and the slope of the enhancement curve in the interval between the beginning of the rise of the curve and its maximum.
(Fig.
3).
The beginning of arterial enhancement was evaluated in an artery that was not part of the lesion.
Thus,
the malformations were classified as high-flow or low-flow lesions using the following criteria: (I) findings on T1- and T2-weighted imaging (signal voids,
signal intensity); (II) the artery–lesion time; (III) the time of maximum lesion enhancement; and (IV) analysis of the slope of the enhancement curve.
Statistical analysis
Continuous variables are expressed as the median (range).
Normality was confirmed or excluded using the Shapiro–Wilk test.
Continuous variables were compared using the Mann–Whitney U-test.
Statistical significance was set at P < 0.05.
Receiver operating characteristic (ROC) analysis was used to determine the artery–lesion time,
maximum enhancement time,
and slope for differentiation of high- and low-flow malformations.
In addition,
sensitivity and specificity were determined for all methods evaluated.