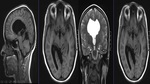
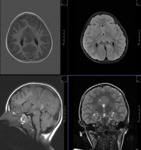
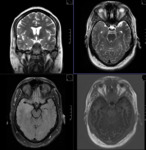
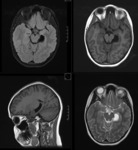
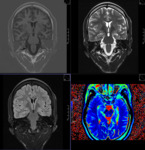
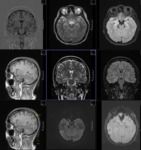
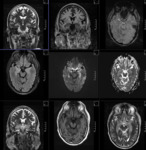
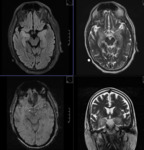
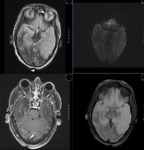
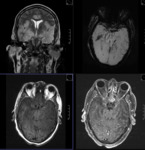
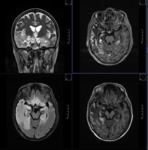
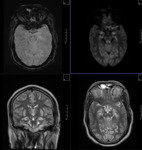
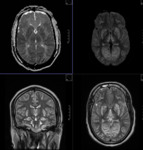
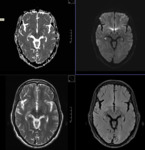
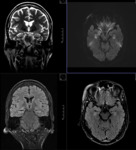
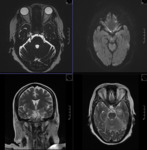
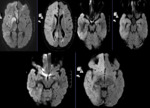
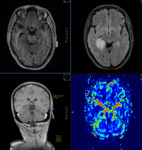
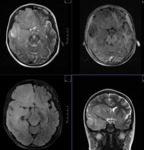
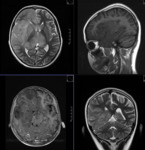
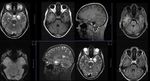
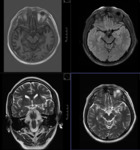
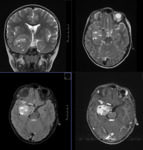
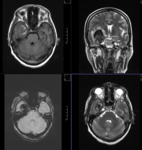
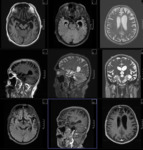
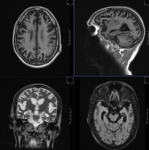
MR TECHNIQUE:
Most patients were scanned on a 3.0 T MRI system using a head matrix coil,
while a few cases were performed on a 1.5 T MRI system using a head sense coil.
The following sequences were acquired:
T2 AXIAL AND CORONAL/ T1 AXIAL/ T1MPRAGE/ T1 IR/ SWI/ T2 CORONAL/ FLAIR AXIAL routine imaging.
Additional sequences are:
T1 MPRAGE sequence was acquired in sagittal plane with a slice thickness (ST) of 0.95 mm,
and reconstructed in all three (axial,
coronal and sagittal) planes.
Coronal high resolution oblique sequences in T1 (TR/TE/TI/FOV- 2500/9.4/499ms/ 220mm,
T2 (TR/TE/FOV- 4000/94ms/ 220mm) and FLAIR (TR/TE/TI/FOV- 9000/81/2499.1ms/ 220mm) with a slice thickness of 3mm.
Diffusion-weighted three-scan trace in the transverse plane by using echo-planar imaging was performed with b-values of 0,1000 and 2000.
5–6 ml of intravenous gadolinium (1 ml per 10 kg of body weight) contrast agent was used for the contrast-enhanced study.
MRS was performed by using a mutivoxel point resolved spectroscopy acquisition technique (ST515 mm; TR/TE,
1590/30).
T2- weighted images are most useful although signal change within the hippocampus may be more easily confirmed on FLAIR images.
T1-weighted images may allow better grey-white matter discrimination and aid in identifying coexisting cortical dysplasias and heterotopias.
The axial plane gives a useful overview of the temporal lobe and may reveal gross lesions or variations.
Unless the possibility of temporal lobe pathology or epilepsy has been raised clinically,
coronal studies are unlikely to have been performed,
and the axial image may therefore give the only clue to a lesion.
Coronal T2-weighted MRI is the mainstay of temporal lobe imaging.
- Coronal imaging is particularly useful in hippocampal (or mesial temporal) sclerosis.
The axis for coronal imaging is slightly perpendicular to the long axis of the hippocampus and is the best sequence for imaging.
-It is important to begin reading anteriorly at the temporal poles to check for symmetry in positioning of the patient otherwise spurious differences in the size of the hippocampi may be encountered.
-Behind the temporal pole,
the first mesial temporal structure is the large rounded grey matter mass of the amygdala,
after which the hippocampal head body and tail are progressively revealed.
Sagittal images of the hippocampus are useful to identify the whole extent of the hippocampus and the pathology can be assessed directly without reference to the contralateral side.
In the investigation of complex partial seizures,
especially if surgery is contemplated,
MRI findings must be correlated with other investigations including EEG,
and often SPECT or PET as well.
METHODS AND MATERIALS:
A retrospective study (2012- 2016) was conducted comprising a collection of all the pathologies affecting the hippocampus.
The study includes both males and females ranging from 1-70 years with varying clinical presentations.
We found 27 different clinical entities on the basis of clinical history,
laboratory results and MRI findings.
Neoplastic pathology was the most frequent in this series.
IMAGING FINDINGS
In the present study,
we came across the following pathological conditions affecting the hippocampus and aim to discuss the unique MRI features for each clinical entity which help in characterisation and final diagnosis.
1) DEVELOPMENTAL
A) Anomalies of hippocampal formation-
include incomplete rotation,
atrophy,
round hippocampi,
an abnormally medial location,
and are either isolated or associated with corpus callosal dysgenesis,
lissencephaly,
holoprosencephaly,
heterotopias,
cortical dysplasias,
schizencephaly,
tuberous sclerosis,
and Fukuyama muscular dystrophy.
This is due to an arrest of the normal process of hippocampal inversion.
The HF is the first cortical area to differentiate and appears at 10 weeks’ gestation.
By 18 to 20 weeks,
the hippocampal fissure becomes reoriented from vertical to horizontal.
Because hippocampal neurons have to migrate from a germinal zone to their final location,
we presume that the abnormal hippocampal configurations are a result of abnormal hippocampal neuronal migration.
-Agenesis of the corpus callosum,
lissencephaly,
holoprosencephaly- Incomplete inversion of the HF / vertical hippocampi that are normal in size.
-Tuberous sclerosis- small and vertically oriented HFs
-Fukuyama muscular dystrophy- straight perpendicular HFs without hippocampal sulci/ an abnormal globular-shaped HF.
-high association of vertical or globular HF with cortical/ migrational disorders.
If there is a unilateral abnormal HF,
a focal cortical disorder would be located on the same side,
causing epilepsy and/or developmental delay.
-HF is a visible component of a more extensive disorder,
and the evaluation of HF on MR images may help in the detection of these abnormalities.
B) Focal cortical dysplasia affecting the hippocampus.
C) Choroid fissural cysts- nonneoplastic epithelial-lined cysts of the choroid plexus in the lateral ventricular atria.
Signal intensity on MR images is variable and are iso- or hyperintense on T1-weighted MR images compared with CSF and show rim or nodular contrast enhancement.
CPCs are hyperintense to CSF on T2-weighted images.
The majority are mildly FLAIR hyperintense.
Two-thirds show restricted diffusion.
2) MESIAL TEMPORAL SCLEROSIS-
Uni or bilateral (10%) and is the most common pathological abnormality in temporal lobe epilepsy.
Most patients present with complex partial seizure.
Primary MRI findings include volume loss,
loss of internal architecture or interdigitations and an abnormal increased T2/ FLAIR signal of the hippocampus as a result of underlying gliosis and the subsequent increase in free water content.
Secondary findings include loss of grey white matter interface at the anterior temporal lobe,
associated atrophy of parahippocampus gyrus,
collateral white matter,
mamillary body and fornix and a dilated temporal horn of the lateral ventricle.
Optimised high resolution oblique coronal thin sections taken perpendicular to the long axis of the hippocampus are highly sensitive and specific for detection of mesial temporal sclerosis.
Additional 3D volumetric studies can be performed,
and although time consuming to post-process may be more sensitive to subtle hippocampal volume loss.
Gadolinium is not required.
T2 relaxometry may also be useful in detecting cases of hippocampal sclerosis.
3) LIMBIC ENCEPHALITIS
Most common inflammatory disease affecting the hippocampus and the amygdala is limbic encephalitis and occurs in three major forms:
A) paraneoplastic subtype
-Mechanism: systemic neoplasia that expresses onconeuronal antigens which results in the production of antibodies that target neoplastic tissue and normal brain tissue.
-Small cell lung carcinoma,
testicular germ cell tumors and hodgkins lymphoma being the most common.
-MRI features: unilateral or bilateral T2/ FLAIR hyperintensity in the medial temporal lobes,
amygdala,
cingulate gyrus,
insula,
subfrontal cortex and inferior frontal white matter with no mass effect or enhancement.
·Cerebellitis,
striatal abnormalities,
and brain stem encephalitis may be associated.
-Cancer control is a crucial step in the management of PLE,
which is usually followed by the remission of the paraneoplastic syndrome.
-Differential is mainly HSV encephalitis; but a more acute history of febrile illness,
increased gyral swelling with mass effect,
increased prevalence of restricted diffusion,
haemorrhages and gyriform enhancement on MRI along with viral titres in serum or CSF confirm the diagnosis.
B) non paraneoplastic subtype
-Mechanism: antibodies against neuronal cell surface or synaptic receptors as in hashimotos thyroiditis,
SLE,
behcets.
-MRI features: T2/ FLAIR hyperintensities and mild swelling predominantly in the amygdala and hippocampus,
without haemorrhages or contrast enhancement and milder diffusion restriction.
It may resolve or progress to mesial temporal sclerosis on follow-up imaging.
In paraneoplastic and non paraneoplastic limbic encephalitis,
only a few case reports detected hippocampal DWI abnormalities,
and it is unclear whether these represented cytotoxic changes in water distribution or mainly a T2 shine-through effect.
C) infectious subtype
-Caused by herpesvirus (HSV AND HHV-6,
the former being more common).
The clinical picture remains the same but the rapidity of onset and sudden progression support the early administration of antiviral therapy.
-Herpes simplex virus encephalitis is a common form of viral encephalitis affecting the young and those of middle age.
MRI features include gyral swelling with T2/ FLAIR hyperintensity and a specific predilection for medial temporal lobes and limbic structures such as insula,
cingulate gyrus and inferior frontal lobes with characteristic sparing of lentiform nucleus.
Basal ganglia involvement on MR imaging favors nonherpetic etiologies.
Diffusion-weighted MRI is a very sensitive tool for early detection and diagnosis of this entity when conventional MRI is normal.
Additional MRI sequences such as SWI for early haemorrhagic foci and post-gadolinium study to look for gyriform enhancement are useful.
In clinically suspected encephalitis these imaging features are diagnostic of this entity that can be supported by detection of HSV antibodies in the CSF along with characteristic EEG changes.
-HHV-6 encephalitis has been increasingly recognized in immunocompromised patients,
after allogeneic hematopoietic stem cell transplantation in hematologic malignancies.
MRI features include T2 and DWI hyperintensities within the uncus,
amygdala,
and the hippocampus,
extending to the entorhinal cortex and subiculum with/ without enhancement.
In comparison to the widespread signal abnormalities in herpes simplex encephalitis including the hippocampal formation and amygdala but also other brain regions,
such as the insular,
frontal,
temporal or parietooccipital cortices,
increased signal intensity is limited to the hippocampus and amygdala in patients with human herpes virus-6 encephalitis.
4) METABOLIC
Osmotic Demyelination Syndrome CPM and EPM (ODS) are classically described as clinical and radiologic manifestations of osmotic myelinolysis,
affecting different brain regions,
confined to the pons in cases of CPM (trident shaped T2 hyperintensity and early restricted diffusion) and extrapontine sites in cases of EPM.
In cases of EPM,
the sites such as the internal capsule,
basal ganglia,
hippocampus,
cerebellum,
and cerebrum are involved.
The presence of an indirect CNS comorbid condition (hepatic or renal failure) presented with more hippocampal lesions.
The high hippocampal involvement may be related to its high vulnerability to the neurotoxic effects of osmotic derangements and systemic stresses in general.
Imaging shows signal changes on the DWI early in the course,
T2 hyperintensity and mild swelling without any haemorrhages or enhancement.
Almost always accompanied by other sites of involvement.
5) VASCULAR
A) Acute ischemic stroke- the arterial supply is by the PCA.
On DWI,
four typical patterns of hippocampal infarction were recognized and distinguished: involvement of (1) the complete,
(2) the lateral,
or (3) the dorsal hippocampus and (4) circumscribed small lesions in the lateral hippocampus.
These infarction patterns correspond well with the vascular anatomy of the hippocampus.
Additional ischemic lesions in the posterior circulation,
suggesting that isolated hippocampal stroke is a rare finding.
Bilateral hippocampal infarction,
which has been shown to be associated with a pronounced amnesic syndrome is very rare.
B) Transient global amnesia (TGA)- is a neurological disorder characterized by sudden onset of antero- and retrograde amnesia,
and complete recovery from this cognitive disturbance within 24 h.
The underlying etiology is unknown,
but cortical spreading depression,
ischemic stroke and venous congestion have been proposed as possible pathomechanisms.
MR does not reveal any DWI/ T2 changes in the acute phase,
but the subacute phase (after 48hrs) reveals very small,
dot-like (1-2mm) T2/ DWI hyperintense lesions with corresponding low signal on ADC maps in the lateral aspect of the hippocampus affecting the CA1 sector of the hippocampal formation.
Time between onset and MRI seems to be crucial for detecting DWI lesions in TGA as about 70–80% of the patients displayed punctate hippocampal DWI changes after 24– 48 hrs.
C) Global Anoxic Encephalopathy-
According to pathophysiology can be subdivided into:
-hypoxic-ischemic encephalopathy (e.g.
caused by cardiac arrest)- DWI demonstrates widespread restriction with T2 signal abnormalities in the basal ganglia,
caudate nucleus,
striate nucleus and thalamus,
followed by the cortex and subcortical white matter,
cerebellum and hippocampus.
Moderate to severe DWI signal changes and low ADC signal in the hippocampal formation resulted in a poorer outcome.
Post cardiac arrest resuscitation,
increased ADC signal in the hippocampus suggests mild vasogenic edema caused by transient increased blood-brain barrier permeability and a better prognosis.
-hypoxic hypoxia (e.g.
caused by suicide by hanging)- After attempted suicidal hanging,
hippocampal DWI lesions can be observed in addition to widespread lesions in the striate nucleus,
thalamus,
and occipital and parietal cortices.
-histotoxic hypoxia (e.g.
caused by carbon monoxide poisoning)- MR signal changes are seen with predilection for the globus pallidus and the temporal lobes particularly the hippocampus.
It may result in a transient vasogenic edema with T2 hyperintensity and swelling or a frank ischaemic necrosis causing cytotoxic edema with restricted diffusion,
low ADC signal and T2 hyperintensity.
T1 hyperintensity may be seen in the globus pallidus signifying haemorrhage.
A differentiation of pathophysiology in anoxic encephalopathy based on DWI findings is not supported by the literature.
6) MISCELLANEOUS
A) Seizure and status epilepticus-
Transient cortical and subcortical T2/ FLAIR hyperintensity,
restricted diffusion with low ADC and mild cortical swelling without any enhancement are seen affecting the hippocampal head,
body,
tail and/ or the parahippocampal gyrus in patients with status epilepticus and in the periictal period.
There may also be a focal increase in the MR perfusion in the periictal period.
Unlike ischaemia where DWI abnormalities take 30 minutes to appear,
the signal changes on DWI and T2 occur simultaneously with the status suggesting a different pathophysiology.
These changes are also reversible unlike ischaemia.
The seizures induced vasogenic edema in the white matter due to focally increased perfusion and vascular permeability and cytotoxic edema in the grey matter due to focal ischemia and other metabolic abnormalities.
The case of status epilepticus progressing to hippocampal sclerosis suggests that prolonged seizure-induced damage to the hippocampus is an initial step in hippocampal sclerosis and periictal diffusion-weighted imaging may be a noninvasive diagnostic tool useful for localization of seizure-induced brain damage.
B) Radiation induced changes-
The temporal lobe/ hippocampus is particularly vulnerable to radiation induced changes after radiotherapy for a nasopharyngeal carcinoma,
post radiation treatment for a previous high grade tumor involving the temporal lobe (primary/ secondary) and localised cyberknife/ radiotherapy for trigeminal neuralgia.
Early changes include edema/ swelling with T2 hyperintensity and mild restricted diffusion,
subacute stage includes patchy enhancement,
resolution of the diffusion restriction,
development of intralesional necrotic foci and the chronic stage includes focal cystic gliotic changes.
C) Hemiplegia hemiconvulsant epilepsy syndrome (HHE)-
Hemiplegia hemiconvulsion epilepsy (HHE) syndrome is a rare epileptic syndrome with prolonged unilateral convulsions,
followed by ipsilateral hemiplegia.
They are usually associated with a febrile illness in children aged less then 4 years.
Subsequently hemiplegia of varying intensities develop which can be permanent.
MR imaging reveals unilateral cerebral hemispheric abnormalities with swelling and edema affecting the cortex and the underlying subcortical white matter.
Corresponding T2/ FLAIR hyperintensity and restricted diffusion are seen affecting the entire hemispheric cortex,
the underlying subcortical white matter and the deep grey matter structures including the basal ganglia and the thalami.
On follow up imaging,
these changes evolve into a unilateral hemispheric cerebral atrophy.
Hippocampal involvement is seen both in the acute and the chronic stages with swelling and acute hippocampal injury and subsequent hippocampal atrophy respectively.
In particular,
it has been shown that the patients with hippocampal involvement are more prone to subsequent unilateral mesial temporal sclerosis.
7) NEOPLASMS tumors with special predilection for the temporal lobe include the following:
A) Low-grade diffuse infiltrative astrocytomas (WHO grade II),
may progress slowly,
with seizures or even focal deficits.
They present with diffuse infiltration and ill-defined grey white matter interface with gyral thickening and signal changes involving the cortex and the underlying subcortical white matter with minimal/ no enhancement.
B) High-grade gliomas (type III and IV) present as heterogeneous mass lesions with haemorrhages,
heterogenous enhancement with internal areas of patchy necrosis and widespread perilesional edema.
In this setting,
MR-perfusion (increased CBF,
CBV) and MR-spectroscopy (elevated peaks of choline,
lactate and reduced NAA) techniques are useful.
C) Gliomatosis cerebri is characterised by diffuse expansion of brain parenchyma with maintained architecture in the absence of a discrete mass or perceivable enhancement.
It has characteristic multilobar involvement,
most commonly frontotemporal,
along with BG and thalami.
MRS is a non-invasive diagnostic method for characterisation of this tumour,
and most reveals decreased N-acetylaspartate,
elevated myoinositol and a normal choline level.
Patients with gliomatosis cerebri are often clinically problematic,
with vague and generalised symptoms.
D) Ganglioglioma are low grade (WHO grade I) tumours and are neuronal- glial tumors.
Epilepsy is a common clinical presentation and this tumour has a typical occurrence in the temporal lobes.
The most common imaging appearance is that of a solid cystic mass lesion with an enhancing mural nodule.
Others include a solid mass expanding the overlying gyrus.
There is minimal perilesional edema.
The solid portion is T1 hypo and T2 hyperintense with variable contrast enhancement and the cystic portion is of variable signal intensity on the conventional MR sequences depending on cystic/ proteinaceous contents.
Internal calcific foci are seen in the majority.
E) Pleomorphic xanthoastrocytomas (PXA)- low-grade astrocytoma (WHO grade II) found in young patients who typically present with temporal lobe epilepsy (approximately 50% in the temporal lobe).
They are cortical tumours with solid and cystic components with vivid contrast enhancement of the solid portion.
There is minimal/ no surrounding oedema.
Slow growth is indicated by the presence of scalloping of the overlying bone.
A reactive dural involvement is seen in the majority.
Calcifications are rare.
F) Dysembryoplastic neuroepithelial tumours (DNET)- are benign (WHO Grade I) slow growing tumours arising from the cortex or the deep grey matter.
The majority are centred in cortical grey matter and are frequently associated with cortical dysplasia (80%).
They are most common in the temporal lobe cortex and characteristically cause intractable partial seizures.
On imaging,
they have a characteristic bubbly appearance with internal cystic spaces on T2,
hypointense on T1 with a variable post contrast enhancement and no perilesional edema.
FLAIR is specifically useful in identification and it may appear as a focal cortical hyperintense focus with a peripheral bright rim sign and suppression of some of the bubbly,
cystic spaces.
Calcification may be seen in 30%.
G) Cavernomas- benign cavernous vascular malformation with characteristic imaging appearance of a multicystic lesion with cysts containing blood products of various ages and therefore various signal intensities on T1 and T2 imaging.
A rim of hemosiderin should also be identified on T2 and SWI sequences.
There is no contrast enhancement and no surrounding edema unless there has been a recent associated parenchymal hemorrhage.
Strong evidence supports cortical involvement and archicortical/mesiotemporal localization as a main risk factor for epilepsy as compared to the subcortical/ neocortical location.
In patients with dominant mesiotemporal location,
the structural and functional assessment of the hippocampal formation is critical for the surgical strategy,
whether to perform pure lesionectomy,
extended lesionectomy,
or lesionectomy plus amygdala-hippocampectomy.
In patients with mesiotemporal cavernoma and additional ipsilateral hippocampal sclerosis,
removal of both lesions is recommended.
H) Metastasis
8) NEURODEGENERATIVE
A) Alzheimer’s disease-
It is a progressive neurodegenerative disorder of the hippocampus in the sixth to seventh decade,
characterised by memory loss,
cognitive impairment and personality changes.
White matter changes in AD present as confluent periventricular hyperintensity,
which involves the temporal lobes.
This hyperintensity is seen as a smooth periventricular halo,
which is more specific for AD than irregular periventricular hyperintensity seen in multi-infarct dementia.
Marked temporal cortical atrophy with disproportionate medial temporal volume loss,
predominantly the hippocampi and parahippocampal gyri with corresponding enlargement of parahippocampal fissures and temporal horns,
is diagnostic of this entity.
Presenile AD- Although there usually is some mild hippocampal atrophy,
the most striking finding is parietal atrophy with atrophy of the posterior cingulum and the precuneus; the hippocampus can be normal.
At an early stage before the evolution of temporo-parietal atrophy,
MRS at short TE with voxel placed in the posterior cingulate gyrus will show a decreased N-acetylaspartate and elevated myoinositol.
B) Frontotemporal dementia-
This is also known as Pick’s disease occurring in the fifth to sixth decade with gradual language,
personality and behavioural changes.
In comparison with AD,
FTD has relatively preserved memory and visuospatial skills late in the disease course.
FTD has a predilection for fronto-temporal lobes in contrast to the temporoparietal volume loss in AD.
Characteristic disproportionate fronto-temporal atrophy with gliosis of underlying white matter on MR confirms the clinical diagnosis.
C) Cerebral Autosomal Dominant Arteriopathy with Subcortical Infarcts and Leukoencehalopathy (CADASIL)
Presenting symptoms include dementia,
migraines,
stroke-like episodes and behavioural disturbances.
Confluent white matter hyperintensity in the frontal and especially anterior temporal lobes in combination with (lacunar) infarcts and microbleeds are seen on imaging.
FLAIR images show classic findings in CADASIL - confluent white matter hyperintensities with lacunar cavitatory infarcts in the subcortical white matter and involvement of the anterior temporal lobes.