The most dangerous complication of cholecystitis may show early findings both in CT than in US,
with possible evolutions in necrosis,
perforations,
abscess,
intraluminal haemorrhage and parietal emphysema.
In the suspicion of such complicances gallbladder wall should be carefully examined in search of gas,
abscess,
focal defects,
sloughed membranes,
and haemorrhage.
Another important complication is the gallbladder perforation.
Gallbladder perforation is a potentially life-threatening condition commonly seen as a complication of acute cholecystitis.
Urgent surgical intervention is often needed to reduce serious morbidity and mortality. It presents a diagnostic challenge due to nonspecific symptoms,
leading to a delay in diagnosis.
Imaging plays a vital role in early identification of this potentially fatal condition and evaluation by more than one imaging modality may be required to make the diagnosis.
Knowledge of specific and ancillary imaging findings is crucial to avoid misdiagnosis.
In this case report,
we will review the pathophysiology and surgical classification of gallbladder complication with particular focus on perforation and discuss the role of multimodality imaging in its diagnosis in a case of perforated gallbladder.
We present a case report of a perforated gallbladder.
GALLBLADDER DISEASE AND ITS COMPLICATION
Gallstones are implicated in over 90% of cases of acute cholecystitis.
Gallstones obstruct the cystic duct or gallbladder neck and irritate the gallbladder mucosa,
leading to the release of several inflammatory mediators and progressive gallbladder wall inflammation.
The pathogenesis of gallstones is related to supersaturation of bile constituents,
most notably cholesterol,
and defects in biliary lipid metabolism.
Biliary dysmotility and prolonged intestinal transit also play a role.
Acute acalculous cholecystitis is the cause in 5%–10% of cases of acute cholecystitis.
This condition typically occurs in severely ill patients and is associated with higher mortality and morbidity.
US findings of acute cholecystitis include gallbladder wall thickening (> 3 mm),
wall edema,
gallbladder distention (> 40 mm),
positive sonographic Murphy sign,
and pericholecystic and perihepatic (C sign) fluid.
Ultrasound is the method of choice (with high sensitivity and accuracy),
to assess the presence of gallstones,
being inexpensive,
repeatable,
even at the patient's bedside; furthermore the patient is not exposed to ionizing radiation.
Gallstones can be seen as echogenic mass with shadowing,
usually mobile; the mass is occasionally adherent (non mobile).
Gallbladder Mass Seen at US can be also cholesterol polyp,
adenomyomatosis,
tumefactive sludge,
gallbladder carcinoma,
metastasis,
adenoma,
ectopic pancreas,
haematoma.
CT findings of acute cholecystitis include gallstones,
gallbladder wall thickening more than 3 mm,
gallbladder distention more than 5 cm in the short axis or more than 8 cm in the long axis,
pericholecystic fluid,
inflammatory stranding,
and adiacent aedema .
Imaging performed in the late arterial or early portal venous phase may show transient curvilinear increased hepatic parenchymal enhancement adjacent to the inflamed gallbladder,
a finding caused by reactive hepatic arterial hyperemia.
COMPLICATION AND RARE FORM OF CHOLECYSTITIS
Emphysematous Cholecystitis: is a rare form of acute cholecystitis.
There is a sex predilection with males being affected in 71 %of cases.
Predisposing risk factors are diabetes (up to 50%),
debilitating disease,
cystic duct obstruction,
and peripheral atherosclerotic disease causing vascular compromise to the cystic artery.
US findings are very bright reflections from a nondependent portion of
the gallbladder wall with associated dirty shadowing,
and in many cases with a ring-down artifact that is a reliablesign of gas.
The pitfall on ultrasound is that gas may mimic a gallbladder full of stones or porcelain
gallbladder.
However,
gas may change in position with patient movement,
thus helping to reach the correct diagnosis
CT findings of Emphysematous cholecystitis radiographically are characterized by the presence of air within the lumen of gallbladder,
gallbladder wall,
or pericholecystic tissue in the absence of an abnormal communication between the biliary system and gastrointestinal tract.
CT is the most sensitive and specific imaging modality for identification of gas in the gallbladder lumen or wall. In severe cases,
acute emphysematous cholecystitis may progress to gangrene and perforation.
Other nonspecific CT findings include pneumobilia,
irregularity or discontinuity of the gallbladder wall,
pericholecystic fluid,
abscess formation,
and free intraperitoneal air,
a finding indicative of perforation.
Gangrenous Cholecystitis: is a relatively common but severe complication of acute cholecystitis,
affecting up to 26% of patients with acute cholecystitis.
Gangrenous cholecystitis carries high morbidity and mortality and tends to occur in elderly patients or patients with diabetes.
US findings of gangrenous cholecystitis can be suspected if one detects intraluminal membranes and marked asymmetry of the gallbladder wall sometimes with irregular mass-like protrusions into the gallbladder lumen or frank discontinuation of the mucosa
CT is highly specific for the diagnosis of acute gangrenous cholecystitis.
CT findings are: intramural or intraluminal gas,
intraluminal membranes,
irregular or absent gallbladder wall,
lack of gallbladder wall enhancement,
and pericholecystic abscess formation.
Transient adjacent hepatic parenchymal enhancement,
pericholecystic fluid,
and striation of the gallbladder wall are less specific findings that may be seen with acute gangrenous or nongangrenous cholecystitis.
These findings may indicate severe acute cholecystitis with possible gallbladder necrosis
Hemorrhagic Cholecystitis: rare complication of acute calculous or acalculous cholecystitis and may be caused by trauma,
anticoagulation,
malignancy,
or iatrogenic or other causes .
Pathologically,
hemorrhage may be caused by mural inflammation and subsequent mucosal infarction and erosion.
Intraluminal hemorrhage may accumulate in the cystic duct and cause obstruction with subsequent inflammatory changes typical of acute calculous cholecystitis.
Clinical symptoms of hemorrhagic and uncomplicated acute cholecystitis may be identical.
Hemobilia caused by hemorrhagic cholecystitis may manifest as hematemesis or melena,
uncommon findings not seen in uncomplicated acute cholecystitis.
US findings include a distended gallbladder with focal wall thickening and irregularity ,
intraluminal membranes,
nonshadowing,
and nonmobile avascular echogenic intraluminal material .
The echogenicity of the blood products is very similar but typically slightly more heterogeneous than tumefactive sludge
CT findings include hyperattenuating bile with possible fluid-fluid level as well as typical findings of acute cholecystitis .
Active contrast agent extravasation,
a finding indicative of active bleeding,
may be seen at arterial phase CT.
Hemorrhage in the gallbladder should be differentiated from other causes of hyperattenuating bile,
such as vicarious excretion from prior intravenous contrast agent administration,
biliary sludge or layering gallstones,
and milk of calcium bile.
Gallbladder perforation: One of the most severe complications of acute cholecystitis,
with mortality rates of up to 15%.
Emphysematous,
gangrenous,
and hemorrhagic cholecystitis may progress to gallbladder perforation.
Diagnosis is often difficult because the clinical symptoms of gallbladder perforation and variants of acute cholecystitis overlap.
The high morbidity and mortality are attributed to delayed diagnosis and subsequent late surgical intervention.
Gallbladder perforation is more common in men than in women and occurs at an average age of 60 years.
The most common mechanism of gallbladder perforation involves cystic duct obstruction leading to gallbladder distention,
vascular compromise,
ischemia,
necrosis,
and ultimately perforation.
Gallbladder perforation in the absence of gallbladder distention is likely related to infection of the Rokitansky-Aschoff sinuses with subsequent necrosis and rupture.
Because of its poor blood supply,
the fundus of the gallbladder is the most common site of perforation.
Acute gallbladder perforation may also result from trauma.
An extraluminal gallstone is a finding specific for gallbladder perforation.
Although it was originally described for US,
the “hole sign,” which refers to a focal gallbladder defect,
is more commonly seen at CT and is a reliable sign of gallbladder perforation.
-Complication of gallbladder perforation include: free intraperitoneal air; bile leak; abscess formation in the liver,
gallbladder fossa,
or peritoneum; and small bowel obstruction.
Treatment of gallbladder perforation includes cholecystectomy,
abscess drainage,
peritoneal lavage,
and antibiotic therapy.
Type III gallbladder perforation may require additional surgery to close the cholecystoenteric fistula.
Cholecystostomy and antibiotic therapy may be used if cholecystectomy is not possible because of the patient’s high surgical risk.
Classification of perforated gall bladder:
In 1934,
Neimeier proposed a classification for GB perforation that is still used today and has prognostic implications
- Type I,
acute free perforation of the GB into the peritoneal cavity without protective adhesions
- Type II,
subacute perforation surrounded by a pericholecystic abscess walled off by adhesions
- Type III,
chronic perforation with presence of a fistulous communication between GB and a viscus
Subacute (type II) perforations are the most common type in most reported series ,
accounting for 60% of all cases.
Chronic (type III) perforation seen in 30% and acute perforation (type I) in 10%.
Type I perforations usually carry a higher mortality.
Pathophysiology: One proposed mechanism of GB perforation is impaction of a gallstone in the cystic duct that leads to obstruction and accumulation of bile within the
GB causing distension.
The presence of intraluminal bile salts causes chemical inflammatory reaction of the GB mucosa.
Progressively worsening distension
will compromise the vascular supply leading to gangrene,
necrosis and perforation of the GB wall.
Focal ischemia of unknown etiology has also been proposed as a mechanism of GB rupture,
especially in cases without acute inflammation or gallstones.
Perforation can be found in the fundus,
body,
and the neck of GB although fundus is the most commonly perforated site secondary to its relatively poor blood supply (farthest from the cystic artery thus most prone to
ischemic injury).
Imaging findings: Utrasound (US) is usually the initial method of investigation of choice in patients with suspected acute cholecystitis or its complications though findings may be non-specific.
Chau et al.
first described the ‘‘sonographic-hole’’ sign,
which is the direct visualization of a GB wall defect on US .
It is a very specific sign of GB perforation that can be seen
on US,
computed tomography (CT),
or magnetic resonance (MR) imaging but is not always visualized.
CT is superior to US for the diagnosis of GB perforation because of its ability to better demonstrate a focal wall defect.
Finding gallstones outside of the GB is also specific for GB perforation in the correct clinical setting.
Interruption of the GB wall and extraluminal gallstones is usually better seen on CT gas within gallstones (‘‘Mercedes Benz’’ sign) outside of the GB may be present and can facilitate the diagnosis of GB perforation on CT or MR imaging.
A focal bulge in the GB wall has been described as a sign of GB rupture.
Mesenteric or omental fat streaking is another ancillary finding of GB perforation seen on CT.
Subacute GB perforations (Type II) are usually contained by a pericholecystic abscesses.
They appear as complex echogenic pericholecystic fluid collections on US usually in the presence of a thickened hypoechoic edematous GB wall and cholelithiasis.
CT further helps to identify and evaluate the location and extent of such Abscesses.
CASE REPORT
We report a case of an old man who presented a complicated cholecystitis framework.
The patient presented with the following symptoms: major pain associated with onset of bleeding.
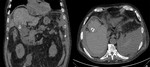
Ultrasound were present both lithiasic and hemorrhagic areas.
The CT also highlighted the presence of a distended gallbladder.
The patient also had hemarthrosis bone of right shoulder; he was suffering from coagulopathy,
probably acquired haemophilia.
The acquired haemophilia is a disease characterized by the onset of hemorrhagic manifestations and alterations of coagulation tests in subjects without previous personal or family of coagulation disorder.
It is an autoimmune condition,
since the presence of auto-antibodies directed specifically against a clotting factor (inhibitors) determines an interference in the coagulation function,
bringing laboratory abnormality and hemorrhagic manifestations.
In the great majority of cases are produced anti-Factor VIII antibodies (FVIII),
for which notes aPTT elongation and a deficiency of FVIII: therefore generally when we speak of acquired hemophilia,
it refers to a hemophilia A.
It affects about one person per million per year and is characterized by a high mortality rate
In congenital hemophilia bleedings are primarily in joints,
while in hemophilia experience bleeding are mainly dependent on the muscles,
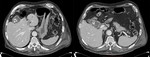
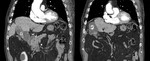
skin and gastrointestinal tract.The CT Total body showed a strongly stretched gallbladder,
hydropic,
with blood components,
the presence of septa and multiple gallstones.
In relation to haemophilic pathology of the patient and after surgical consultation,
we opted for a conservative therapy.
This resulted in an unfavorable context and allowed to view the most serious complication that is the perforation.
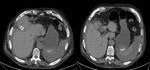
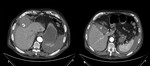
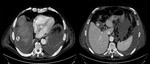
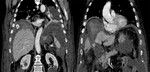
The CT control executed after a month showed perforation of the gallbladder wall,
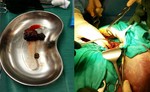
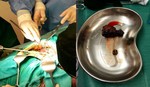
abdominal effusion and the presence of a gallstone in the right subphrenic space; the patient was therefore subjected to surgery in urgency.The patient has been subjected to surgical removal of the gallstone and infected gallbladder.