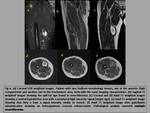
We searched our hospital’s database for cases from the last 5 years,
with a confirmed neurogenic tumor diagnosis,
describing their MR imaging features.
We correlated them with the tumor pathology analysis.
- Schwannomas.
Schwannomas or neurilemomas stands for approximately 5% of benign soft tissue tumors.
They have a predilection for sensory nerves.
They are usually slow growth tumors,
presenting as a 5 cm or less painless mass.
Commonly,
only the larger ones are symptomatic,
due to direct nerve compression.
These tumors have a capsule made of epineurium,
because they grow inside the sheath of the nerve.
Because of this they have a fusiform morphology,
and the nerve entering and exiting the lesion may be seen.
The tumor grows eccentrically from the nerve axis,
what makes its surgical removal easier.
On MRI imaging they present intermediate signal intensity in T1 sequences,
similar to muscle,
and in T2 sequences,
they show a high-intensity signal.
However,
other peripheral nerve tumors may have similar signal intensity.
There are other MRI findings more specific:
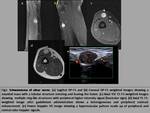
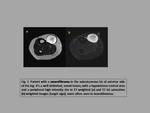
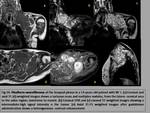
-Split-fat sign: A rim of fat around the tumor,
best seen in T1-weighted images,
suggests that the origin of the tumor is in the intermuscular space above the neurovascular bundle,
location in which these neoplasms are the most frequent (fig.2).
- Target sign: It’s an image formed by a central low-signal intensity zone in T2-weighted images,
with a peripheral high-intensity signal ring.
This can be seen in schwannomas,
although it is more frequent in neurofibromas.
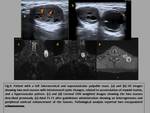
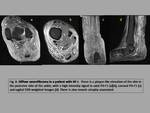
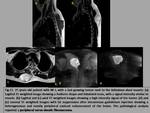
- Fascicular sign: Multiple small ring-shaped structures,
better seen in T2-weighted images,
with peripheral higher intensity signal (fig.3). This sign is more often seen in schwannomas.
The pattern of contrast enhancement is variable and heterogeneous,
but schwannomas often have a diffuse and predominantly peripheral enhancement pattern.
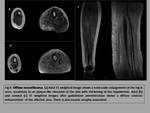
A heterogeneous appearance due to cystic degeneration is more frequent in schwannomas (fig.4) than neurofibromas.
Also central necrosis and calcifications can be observed in ancients schwannomas subtype.
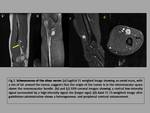
Muscle atrophy with increased striated fat content is observed in this type of tumors,
affecting the innervated muscle by the affected nerve,
better visualized in T1-weighted sequences (fig.5).
- Neurofibroma.
Neurofibroma accounts for 5% of benign soft tissue tumors.
Three types are described: localized,
diffuse and plexiform,
being the first one the most frequent and standing for a 90%.
They are mostly sporadic and not associated with neurofibromatosis type 1 (NF1).
Localized neurofibromas usually affect superficial cutaneous nerves.
They are slow-growing tumors,
measuring less than 5cm and painless at the time of presentation.
Neurofibromas are usually solitary,
although they may be multiple (fig.6). They present a fusiform grow-pattern,
with the nerve "entering and leaving" the tumor.
They are not encapsulated.
Differentiation between schwannoma and a neurofibroma is possible,
if the central nerve is visualized within the neurofibroma (and eccentric to the tumor in the schwannoma),
but it is only identified in a 65% of cases.
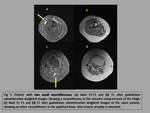
There are other signs that may help making the differential diagnosis between these two entities.
These are the target sign (fig.7), fascicular sign and split-fat sign that we already described.
The pattern of contrast enhancement is variable,
however,
neurofibromas often have a more intense central enhancement.
Muscular atrophy is also common.
Diffuse neurofibroma affects children and young adults more frequently.
They are usually located in the subcutaneous fat of the head and neck.
Clinically,
neurofibromas produce an elevation in the form of plaque,
affecting the skin with thickening of the hypodermis,
in an ill-defined manner (fig.8).
When this affection is significant,
a noticeable enlargement of the affected limb may be seen (fig.9).
The treatment of localized and diffuse neurofibromas is usually complex,
due to the tendency of these tumors to grow intraneurally.
This can make surgical resection harder,
and a complete excision of the tumor not be possible,
having to damage the nerve,
performing a partial excision of it.
The other treatment option is having a conservative attitude.
Plexiform neurofibromas are practically pathognomonic of neurofibromatosis type 1 (NF1).
The development of these lesions usually occurs during childhood and precedes cutaneous neurofibromas.
Neurofibromas associated with NF1 often affect the deep nerves and are usually multiple and large.
The plexiform neurofibroma represents a diffuse affectation of a long segment of a nerve and its branches,
with a tortuous expansion; described macroscopically as a bag of worms (fig.10). It can be associated with a massive and disfiguring enlargement of a limb (elephantiasis).
It usually leads to bone hypertrophy due to chronic hyperemia.
- Malignant tumors of the peripheral nerve sheath.
The incidence of malignant transformation of peripheral nerve sheath tumor ranges from 2% to 29% in patients with NF1.
When they become malignant,
patients manifest pain and neurological symptoms,
or a rapid increase of size of a previous neurofibroma.
The morphological distinction with benign tumors may be difficult,
but there are certain characteristics that may suggest malignancy: diameter more than 5cm,
prominent vascularization,
heterogeneity,
central necrosis,
rapid growth,
contrast enhancement and infiltrating borders (fig.
11). It is important to identify these findings because they may condition the patient’s treatment.
A complete surgical excision with wide borders of resection is the treatment of choice.
Others:
- Nerve-sheath Ganglion.
The nerve-sheath ganglion is also considered a tumor originated from the nerve.
Most of these lesions are located inside the external popliteal nerve next to the fibular head,
caused by chronic friction.
This produces myxoid changes and secondary cystic formation.
In MRI,
the nerve-shealth ganglion is shown as a cystic mass with septa,
with a slight increase in signal intensity on T1-weighted images,
due to protein content. Peripheral and septa enhancement may also be seen.
Treatment consists on local excision.
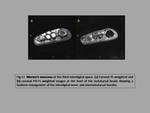
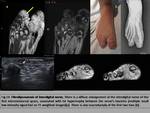
- Morton's Neuroma
Morton's neuroma is an interdigital plantar nerve fibrosis,
which may produce paroxysmal pain between the 3rd and 4th metatarsal head.
It’s a fusiform enlargement of the interdigital plantar nerve at its bifurcation and perineural fibrosis.
It is well delimited.
In T1 weighted images they are isointense to muscle,
and hypo-intense than fat in T2 weighted images,
because of the collagen and fibrosis content (fig.12).
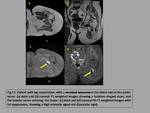
- Traumatic neuroma
Traumatic neuroma develops from a non-neoplastic proliferation of the proximal end of a nerve,
damaged by trauma or surgery (amputation).
Pain is the most common symptom.
Traumatic neuromas may have a fusiform morphology or being like a bulbous nerve’s end.
It develops after 1-12 months of injury or surgery,
with a disruption of neurogenic tissue,
and multidirectional tumor proliferation.
They usually have signal intensity similar to muscle on T1-weighted images,
and intermediate-high signal intensity on T2-weighted sequences.
The signal intensity is usually heterogeneous,
with a ring-shaped pattern (fascicular sign) that correlates with the histological appearance of the nerve fascicles (fig.
13). Sometimes it shows contrast enhancement,
but this finding is variable and not very specific.
-Fibrolipoma of the nerve.
The nerve’s fibrolipoma or fibrolipomatous hamartoma of the nerve is produced by hypertrophy of mature fat and fibroblasts of the nerve’s epineurum.
They usually appear during childhood,
as a soft mass that slowly grows on the margin of the hand or foot.
It may be painfull or cause neurological symptoms.
It can be associated with macrodactyly due to lipomatous macrodistrophy.
In MRI it has a characteristic appearance of multiple small low-intensity signal foci (representing the fascicles of the nerves) surrounded by fat-intensity signal (fig.14). Treatment is controversial because of the extent of the affected nerve tumor and the presence of macrodactyly.