Cases presented were collected between January 2013 and July 2016.
Chest radiography has a low diagnostic value in the detection of postoperative complications [1].
Therefore,
Computed Tomography (CT) is the imaging modality of choice in evaluating the postoperative patient.
Normal postoperative findings,
both early and late,
will be illustrated.
Familiarity with normal postoperative findings is crucial for recognizing complications and disease recurrence.
Postoperative complications can be divided in early and late complications (Table 1),
including pulmonary edema, empyema,
cardiac herniation,
hemothorax,
chylothorax,
bronchopleural fistula,
eosphagopleural fistula,
postpneumonectomy syndrome,
… Detection of systemic recurrence is often straightforward,
but recognition of early local recurrence can be challenging.
Tips and tricks for making the correct diagnosis will be discussed.
1.
Normal postoperative changes:
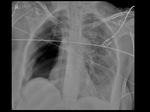
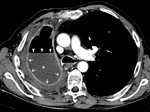
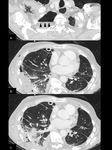
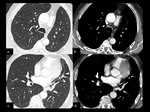
Initial findings after pneumonectomy should comprise a midline position of the trachea,
a postpneumonectomy space filled with air and/or a slight congestion of the remaining lung (Fig.
1).
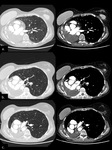
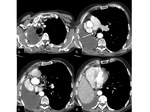
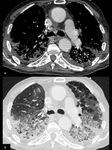
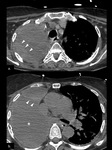
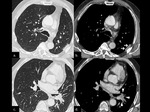
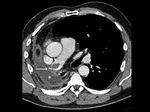
After 1 week,
the postpneumonectomy space gradually fills with fluid whereas the mediastinum gradually shifts towards the postpneumonectomy space as a result of air reabsorption from the surgical site and a hyperinflation of the remaining lung.
The degree of mediastinal shifting depends on the elasticity of the remaining lung (Figs.
2 and 3).
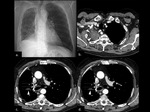
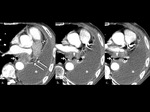
Initial findings after lobectomy or limited excision include a volume loss of the lung and the presence of fluid within the surgical site (Fig.
4).
2.
Early postoperative complications:
2.1.
Pulmonary edema
Pulmonary edema is a possible life-threatening complication with a mortality rate of 80–100% [2].
The etiology remains largely unknown although an increase in hydrostatic pressure and an altered capillary permeability are known to be causing factors.
Pulmonary edema occurs more frequently after right pneumonectomy.
This entity can be diagnosed when all other causes of a postoperative ground-glass and consolidation are excluded including aspiration infection,
heart failure,
bronchopleural fistula and ARDS [2].
2.2.
Empyema
Althoug this is an uncommon complication after thoracic surgery,
it remains a potentially fatal complication with a mortality rate of 16-71% [1].
This complication can occur in both the early and late postoperative stage.
In the early postoperative period it is caused by intraoperative contamination and/or a residual infection in the pleural cavity,
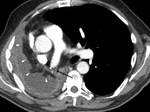
whereas in the late postoperative period it is caused by hematogeneous spread of an infection (Fig.
5).
Furthermore,
postoperative empyema can be seen secondary to a bronchopleural or esophagopleural fistula.
Postoperative empyema should be considered when the postoperative space fills rapidly with fluid and is accompanied by a mediastinal shift toward the remaining lung.
Empyema is also characterized by an irregular thickening of the remaining parietal pleura.
Furthermore,
the presence of a bronchopleural or esophagopleural fistula can be depicted as the cause of empyema.
2.3.
Cardiac herniation
A very rare complication after pneumonectomy (and in rare cases after lobectomy) which requires immediate surgical reduction.
During surgery,
a pericardial defect is created to visualise the hilar vessels.
Cardiac herniation is defined as a prolaps of cardiac muscle through this defect.
A right-sided herniation comprises a counterclockwise rotation of the heart around the superior vena cava,
producing a superior vena cava syndrome.
In a left-sided herniation,
the ventricles herniate into the left thoracic cavity and are strangulated by the epicardial defect.
A cardiac herniation should be thought of when a cardiac displacement is present without the presence of a large pleural effusion or a tension pneumothorax accounting for this displacement.
2.4.
Dehiscence of the anastomosis
Dehiscence of the anastomosis may present as an early complication in cases of extended lymph node resection which increases the risk of bronchial wall ischemia.
This may result in excessive tension of the suture line,
leading to anastomotic dehiscence.
This complication is particularly seen after a sleeve lobectomy and may lead to bronchopleural fistulas.
At CT,
an anastomotic dehiscence is seen as a defect of the bronchial wall or as extraluminal air surrounding the suture line [1].
Furthermore,
a bronchopleural fistula may be discerned when present.
2.5.
Bronchopleural fistula
A bronchopleural fistula is a potentially fatal complication with a mortality rate of 16-23% (when associated with aspiration pneumonia and subsequent ARDS).
It occurs more common after right pneumonectomy due to the fact that the right main bronchus is shorter (and can therefore be concealed less effective during surgery) and is more vulnerable to ischemia (one bronchial artery compaired to the two bronchial arteries on the left side) [4].
A bronchopleural fistula can be diagnosed by monitoring the air-fluid ratio after pneumonectomy.
Indirect CT-findings that should raise suspicion of a bronchopleural fistula:
- Failure to fill the postpneumonectomy space
- Reappearance of air in the postpneumonectomy space after opacification.
- A 1,5 to 2 cm drop of the air-fluid level in the postpneumonectomy space.
- Persisting pneumothorax despite the presence of chest tubes.
- Progressive mediastinal and subcutaneous emphysema.
Obviously,
a bronchopleural fistula can also be diagnosed by identifying an actual bronchopleural tract (Figs.
6 and 7).
The risk of this complication can be reduced by covering the bronchial stump using a free or pedicled pericardial fat pad which can also be appreciated on CT [5,6] (Fig.
8).
2.6.
Pneumonia
Pneumonia after lung surgery has a mortality rate of 25% [2] and is mainly caused by apiration of gastric and/or tracheobronchial secretions (intubation and mechanical ventilation) or by colonization of bacteria in an atelectatic lung.
Another,
less frequent cause,
is the transbronchial spill of secretions through a bronchopleural fistula [1,
2].
CT features are [3]:
- Parenchymal consolidation,
with or without an airbronchogram (Fig.
9)
- Centrilobular consolidation
- Ground glass opacity,
with or without crazy paving
CT is also a useful imaging modality to identify a bronchopleural fistula as a cause of postoperative pneumonia [2].
2.7.
Acute lung injury/ARDS
Acute respiratory distress syndrome (ARDS) is a life-threatening complication with a mortality rate of more than 80% in patients after a pneumonectomy [2].
After pneumonectomy,
there is an increased blood flow through the remaining lung which may cause disruption in the barrier between the capillary endothelial cells and the alveoli.
Alterations in the respiratory mechanics -resulting in a barotrauma of the lung parenchyma- may also be a cause of ARDS.
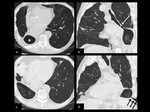
The CT-features of ARDS/acute lung injury are (Fig.
10):
- Ground glass opacity with some consolidation in the dependent parts of the lung resulting in a opacity gradient (from ventral to dorsal)
- Cystic destruction in the ventral lung areas as a result of ventilation induced barotrauma
- Symmetry of these abnormalities is an important finding (in case of a limited resection)
2.8.
Hemothorax
A postoperative hemothorax has an overal mortality of less than 0,1% [1].
This bleeding is mostly originating from a bronchial artery or a systemic vessel.
Less frequently it originates from a major pulmonary vessel or a systemic vein.
This complication manifests as a rapidly evolving and enlarging pleural effusion.
CT findings include a pleural effusion with higher and more heterogeneous attenuation (Fig.
11) or a heterogeneous pleural effusion with a layered appearance (fluid-hematocrit level).
2.9.
Chylothorax
This complication is defined as an accumulation of chyle in the pleural cavity and is the result of a disrupted thoracic duct.
This complication has an incidence of 0,5-1% after pneumonectomy.
As in a hemothorax,
there is a rapidly emerging pleural effusion within the postoperative space.
The attenuation of this chylous accumulation can be variable on CT,
depending on the fat or protein content.
Analysis of the fluid after thoracentesis showing a high triglyceride concentration,
can be considered diagnostic.
2.10.
Esophagopleural fistula
This is a rare and often fatal complication [7] that occurs in 0,2 – 1 % of patients after a pneumonectomy [1].
There are three different mechanisms which result in an esophagopleural fistula: surgical induced injury,
mediastinal cancer recurrence and chronic infection
Due to these different mechanisms,
this complication can occur in both the early and late postoperative period.
The diagnosis is usually confirmed at imaging (Fig.
12).
Both CT and esophagography are useful imaging modalities.
However,
small fistulous trajects can often be missed during an esophagography.
Administration of oral contrast right before the CT is performed,
can certainly be helpful in depicting a possible fistula.
Furthermore,
CT is often useful in detecting the cause of this complication (infection,
tumor recurrence,
…) and evaluate the presence of other complications.
3.
Late postoperative complications
3.1.
Postpneumonectomy syndrome
This complication is mostly seen in children and young adults within a year after surgery [2] and consists of major airway compression as a result of some compensatory mechanisms after lung resection [1].
During these compensatory mechanisms the intrathoracic airways are stretched against fixed mediastinal structures.
It occurs more often after right pneumonectomy in which the overexpanded left lung displaces the mediastinum towards the right side resulting in a right-sided cardiac herniation and a displacement of the trachea with resultant compression of the left main bronchus by the aortic arch and left main pulmonary artery [2].
CT imaging illustrates a displacement of the heart and trachea and a compression of the left main bronchus.
A postpneumonectomy syndrome is primarily seen in young patients,
which is related to the increased elasticity and compliance of lungs and mediastinum,
and is rarely seen after surgery in the older lung cancer patient.
3.2.
Complications related to postoperative treatment
3.2.1.
Radiation induced cryptogenic organizing pneumonia (COP)
This usually occurs 6 to 10 weeks after therapy and is an inflammatory healing process which is characeterized by organization of an exudate.
On CT COP is characterized by sharply demarcated,
migratory consolidationes with peribronchial or subpleural location.
COP differs from the normal radiation induced pneumonitis by the presence of migratory consolidations and the absence of chronic radiation sequelae [2].
3.2.2.
Radiation induced pneumonitis
These findings are usually confined to the mediastinal radiation field and occur 4 to 12 weeks after therapy [2].
As a result of the postoperative retrosternal pulmonary shift (in pneumonectomy),
a portion of the remaining lung is included within the radiation field.
In the early phase,
ground glass opacities and/or consolidations can be appreciated on CT.
In a later phase both traction bronchiectasis and volume loss can be discerned.
3.3.
Local tumor recurrence
Local recurrence is defined as (a) tumoral recurrence in the chest wall and/or parietal pleura,
(b) tumoral recurrence at the surgical margin and/or bronchial stump and (c) the presence ipsilateral mediastinal lymph node metastases.
This definition corresponds to the anatomic sites which are included in a typical postoperative radiation field [8].
Recurrence after curative resection implies the presence of micrometastases or hidden cancer cells [2] and the detection of these recurrent tumors can often be difficult.
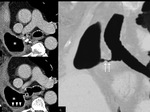
CT imaging can depict tumoral recurrence at the surgical margin or the bronchial stump (Figs.
13 and 14) and can detect pleural seeding and the presence of enlarged mediastinal lymph nodes.
Differentiation between tumor recurrence and postoperative fibrosis can be very challenging,
especially when the recurrent lesion is small,
ill-defined or has no mass effect at the surrounding structures.
Therefore,
when in doubt,
a repeat CT may be performed to evaluate the growth of a lesion [1].
3.4.
Pulmonary artery stump thrombosis
Formation of a thrombus within the pulmonary artery stump occurs in the early days after a pneumonectomy [9].
Little is known about the incidence and natural history of a postpneumonectomy pulmonary artery thrombosis.
However,
a retrospective review study of 147 postpneumonectomy patients [10] found a filling defect in the arterial stump in about 12% of the patients,
suggesting that this is not a rare phenomenon.
This finding was once thought to be a part of a tumor recurrence or a thromoboembolic event and was assumed to be a lethal complication after pneumonectomy [10].
Nowadays,
a pulmonary artery thrombosis is thought to be an in situ thrombosis and is likely a consequence of flow dynamic changes within the arterial stump.
Obviously,
this finding can be appreciated on a CT-scan as a filling defect in the arterial stump which can persist for years after the surgical procedure (Fig.
15).
There is an equal frequency of arterial stump thrombus formation following either a left or right pneumonectomy.
Furthermore,
the length of the arterial stump is the only determing factor in the formation of a thrombosis.