A literature review has been performed.
Both clinical and radiological characteristics of MTS will be presented,
including a classification system.
Clinical presentation
Acutely,
presentation includes,
left lower extremity DVT in the absence of differential causes of iliofemoral thrombosis.
Chronically,
patients may note venous claudication,
post thrombotic syndrome,
and chronic venous insufficiency which often doesn't respond to conventional management.
Positive clinical outcomes often rely on early diagnosis and treatment.
However,
this represents a challenge due to the significant proportion of patients with asymptomatic disease.
Classification
- Stage I: No structural venous changes. Asymptomatic
- Stage II: venous spur development
- Stage III: symptomatic obstruction; left lower limb DVT
Imaging findings
The bedrock of diagnosis remains within a plethora of imaging modalities including,
doppler ultrasound (DUS),
computed tomography venography (CTV),
conventional venography,
magnetic resonance venography (MRV),
and intravascular ultrasound (IVUS).
1.
Doppler Ultrasonography
This imaging modality is commonly performed initially to assess venous anatomy due to its non-invasive nature and lack of patient risk.
However,
DUS is limited in its assessment of suprainguinal anatomy due to the relatively deep location.
It is also unable to comment on some specific elements of MTS anatomy,
e.g.
intra-luminal venous spurs.
Therefore,
a negative finding should not preclude further pelvic vein imaging in the context of unilateral leg swelling and pain.
2.
CT Venography
CT with intravenous contrast can effectively detect MTS,
venous collaterals,
decipher thrombotic and non-thrombotic MTS,
and exclude other causes for external compression [5].
Depending on the CT slice thickness,
iliac spurs may not be accurately visualised.

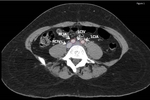
Fig. 1: CT venography below the level of the common iliac artery and vein bifurcation. Note the reduced enhancement of the left common iliac vein (LCIV) compared to the right (RCIV), indicating thrombosis, and its position below the right common iliac artery (RCIA). The left common iliac artery is marked (LCIA).
3.
Magnetic Resonance Venography
MRV is also capable of non-invasively diagnosing MTS,
even without contrast.
It can detect intra-luminal iliac venous spurs in patients with normal DUS,
and assess the degree of collateral flow.
[6]

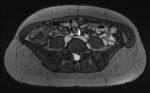
Fig. 3: T2-weighted MRI demonstrating compression of the left common iliac vein (white arrow) by the overlying right common iliac artery (black arrow)
4.
Constrast venography
Contrast is injected into the femoral or politeal veins.
This modality can evaluate the degree of stenosis as well as pelvic venous collaterals indicative of haemodynamic compromise.
Therapeutic intervention may occur concurrently in the form of stenting (Fig.
4).
However,
venography can underestimate the magnitude of stenosis by 30% compared to IVUS.
[7]

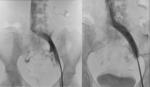
Fig. 4: Venogram demonstrating a high-grade stenosis of the proximal left common iliac vein. There is associated pelvic collaterisation. This compression was corroborated with subsequent intravascular ultrasound.
Right hand image: the same patient subsequently underwent balloon angioplasty and stenting. Post-procedure, there was good in line flow and intravascular ultrasound showed a patent left common iliac vein.
5.
Intravascular ultrasound

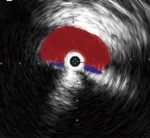
Fig. 5: Intravascular ultrasound with the transducer within the left common iliac vein (blue) demonstrates near complete obliteration of the vessel’s lumen due to compression by the right common iliac artery (red)
References: Brinegar K et al. (2015) Iliac vein compression syndrome: Clinical, imaging and pathologic findings. World J Radiol 7(11): 375–381
IVUS may be used alongside venography and to guide endovascular management.
Further studies are required to more thoroughly assess its utility in MTS diagnosis.
Diagnostic challenges
MTS can present asymptomatically as an anatomical variant and is not necessarily pathological.
A single imaging study may not be sufficient; it has been shown that the degree of LCIV compression significantly differs in the same patient when undergoing repeated MRV and CTV imaging within a short period of time.
[4]
- These are anatomical investigations usually performed whilst supine,
and may not reflect haemodynamic characteristics exacerbated by the standing position.
- Patient volume status also affects findings
Furthermore,
no established diagnostic criteria for imaging exist,
and it is unlikely that a single LCIV stenosis threshold is useful.
- A threshold of visualising 70% narrowing has been proposed by several groups.
[8] However,
there is considerable overlap in the degree of narrowing in patients with left lower limb DVT,
and asymptomatic controls.
- Pelvic venous collaterals are suggestive of a significant occlusion.