This poster is published under an
open license. Please read the
disclaimer for further details.
Type:
Educational Exhibit
Keywords:
Musculoskeletal spine, Neuroradiology spine, CT, MR, Contrast agent-intravenous, Inflammation, Abscess
Authors:
M. Veselova, V. Mazaev, M. Molodtsov; Moscow/RU
DOI:
10.1594/ecr2017/C-1536
Background
Spondylodiscitis - an inflammatory disease of the spine that affects the intervertebral disc and the adjacent vertebral body.
It is clinically manifested by fever and back pain.
Discitis exhibits a bimodal age distribution,
with peaks in early childhood and after age of 50. Male predominance can be observed.
Risk factors for discitis include diabetes,
old age,
immunosuppression,
drug use,
alcoholism,
and renal failure.
Etiology
The most common causes of spondylodiscitis:
- Hematogenous penetration of infection to intervertebral disc from other sources of infection (urogenital system,
respiratory system)
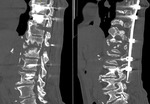
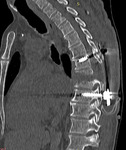
- Development of spondylodiscitis as complications after injuries and surgeries on the spine.
(Fig.1,
Fig.2).
Infectious agents can be classified as follows:
- Bacterial (the most frequent pathogens - staphilococcus aureus (about 50% of cases) -pseudomonas aeruginosa (drug addicts),
streptococcus (often patients with bacterial endocarditis),
H.fluenzae)
- Tuberculosis
- Parasitic (Echinococcus,
Toxoplasma)
- Fungal
Pathogenesis
In adults infection is thought to begin at the vertebral body endplate,
extending into the intervertebral disc space and then into the adjacent vertebral body endplate.
In the paediatric age group infection often starts in the intervertebral disc itself
As the disease progresses,
the infection may spread to the area of the spinal canal and paravertebral soft tissue and can cause such complications as:
- Epidural abscess
- Paravertebral abscess
- Spread of infection to articular,
transverse and spinous processes,
causing their destruction
Disease outcome
Progression of the spondylodiscitis leads to the destruction of the vertebral body and deformation of the spine (most frequently kyphosis ) and gross neurological disorders.
In untreated cases,
bony sclerosis may begin to appear in 10-12 weeks.
Bone block occurs between the vertebral bodies as an outcome of the disease .
Under the effect of anti-inflammatory therapy detectable changes are often limited to a decrease in disc height,
osteoporosis of the end plates,
without development of the bone block.
These changes are often falsely taken for osteochondrosis which leads to diagnostic errors.