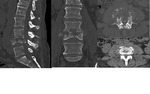
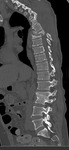
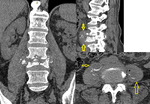
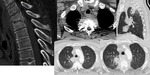
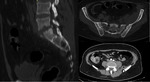
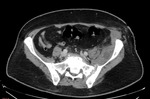
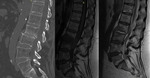
The main imaging findings of spondylodiscitis on CT:
On the early stages:
-reduction of the intervertebral disc height;
- decrease in the density of the intervertebral disc.
After 1-3 weeks:
-thickening of the paravertebral soft tissues,
which can lead to compression of the nerve roots at the neural foramen;
-destruction of adjacent end plates;
-deossification of bone with loss of normal architectures of the trabecular bone
Also may be seen:
-soft tissue replacement of the bone
After treatment:
-osteosclerosis;
-the formation of a bone block from the adjacent vertebral bodies.
Normal 0 false false false RU X-NONE X-NONE MicrosoftInternetExplorer4
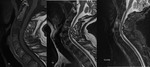
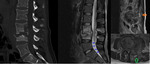
The main imaging findings of spondylodiscitis on MRI:
T1
· low(fluidlike) signal in disc space
· low signal in adjacent endplates
T2: (fat sat or STIR)
· High (fluidlike) signal in disc space
· Vertebral bodies with high signal intensity
· loss of low signal cortex at endplates
· paravertebral tissues have high signal intensity
DWI (can help to distinguish the acute stage from the chronic stage of the disease)
· hyperintense in the acute stage
· hypointense in the chronic stage
The table number 1 shows the comparison of some types of spondylodiscitis depending on their etiology.
|
Infection organism
|
Characteristics
|
|
Bacterial
|
§ The process often grabs the disc and two adjacent vertebrae in the lumbar,
thoracic and cervical spine,
relatively rarely observed in craniospinal,
thoracolumbar and lumbosacral junctions;
§ Rarely can be seen defeat of one vertebra,
combined with a primary lesion of the posterior portions of the vertebrae (intervertebral joints,
arches,
transverse process);
§ Occasionally there is multiple vertebral osteomyelitis involving the body and discs on multiple levels |
|
Tuberculosis
|
§ Progresses indolently,
without acute pain and leukocytosis;
§ Involves adjacent vertebrae(subligamentous spread);
§ Foci of rarefaction predominantly occurs in the anterior parts of two adjacent vertebral bodies;
§ More often infection spreads subligamentally with the formation of large paravertebral abscess;
§ The evident reactive sclerosis can’t be seen at the edges of the vertebral bodies and ligaments;
§ Most often in the thoracic spine;
§ Frequent damage of arches and other parts of the back structures;
§ In the late stage - formation of angulate kyphosis deformation.
|
|
Fungal
|
§ Multiple foci of destruction in the bodies of the vertebrae,
which are surrounded by a ring of sclerotic tissue
§ Consistent involvement of several vertebrae,
transverse and spinous processes,
ribs and other bones
§ A significant incidence of pathological fractures and the relative safety of intervertebral space
§ Chronic disease progression with an increase in the number of foci of destruction
|
|
Parasitic(Echinococcosis)
|
Cysts grow in the vertebral body,
gradually destroying it.
Then,
when the cortex is lysed,
compound cysts spread in paravertebral soft tissue.
Also in the process are involved the transverse process and the edge.
Some cysts penetrate into the spinal canal and compresses the spinal cord. Damage is demarcated from healthy tissue with thin sclerotic rim.
The disease progresses over the years,
gradually increasing ossification of ligaments,
periosteal reaction.
More often discs are intact.
|
Complications of spondylodiscitis on Computed Tomography and Magnetic Resonance Imaging:
Epidural abscess:
-CT
CT even with contrast can struggle to demonstrate smaller collections
-MRI
Gadolinium-enhanced MRI is the imaging choice for diagnosis of spinal epidural infection.
Two main patterns can be seen:
1. phlegmonous stage of infection results in homogeneous enhancement of the abnormal area which correlates to granulomatous-thickened tissue with embedded micro-abscess without a significant pus collection
2. liquid abscess surrounded by inflammatory tissue which shows varying degree of peripheral enhancement with gadolinium
Non-contrast MRI can show liquid abscess too - it is the presence of a region of high T2 signal,
with low T1 signal and without enhancement (usually surrounded by a rim of enhancement).
Paravertebral abscess:
Changes in paravertebral tissues can be characterized on CT-imaging as follows:
· relatively low attenuation central necrotic component with thick capsula circumferentially
· capsular ring enhancement with contrast
· surrounding inflammatory changes (i.e. fat seal)
Differential diagnosis
Possible imaging differential considerations include:
- Modic type 1 degenerative change (It can resemble spondylodiscities because of the presence of bone marrow edema which has high signal intensity on T2WI.
These bone marrow changes may show enhancement on post-contrast images. But such changes as endplate destruction,
increased disk signal intensity on T2-weighted images,
paravertebral or epidural abscess are specific to spondylodiscitis.
- Charcot joint. ( On T2-weighted images,
the presence a high-signal intensity concentric ring surrounding a cartilaginous node may help distinguish an edematous node from infectious spondylitis)
- Schmorl nodes - intravertebral disc herniations(MRI-imagesusually exhibit the same signal characteristics as the adjacent disc,
with a thin rim of sclerosis at the margins.
Acute form can demonstrate the surrounding bone marrow oedema and peripheral enhancement.
These acute features evolve gradually over months).
- Langerhans cell histiocytosis is a rare multi-system disease with a wide and heterogeneous clinical spectrum and variable extent of involvement (sometimes on diagnostic images may be seen changes from another systems which are typical for LCH and that can help to make the correct diagnosis).
On images the first stage presents formation of focus of the lytic destruction,
the second stage leads to the formation of pathological fractures and the third corresponds to the stage of repair.
The LCH is not characterized by reduced height of the intervertebral disc,
and the presence of pronounced osteoporosis.
Often differential diagnosis is difficult and the correct diagnosis can be made only after a biopsy).