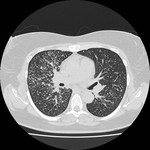
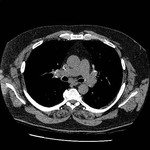
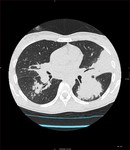
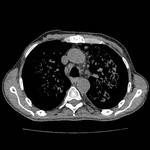
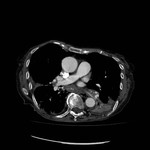
Pulmonary Tuberculosis
Pulmonary tuberculosis is the manisfestation of pulmonary infection by the organism Mycobacterium tuberculosis.
Although mycobacterium tuberculosis can cause infection everywhere within the body,
by far the most commonly affected area are the lungs.
There are 3 manifestations of pulmonary tuberculosis:
- primary infection.
- post-primary infections
- miliary tuberculosis
Computed tomography (CT) is a useful imaging modality in the assessment of pulmonary tuberculosis in the detection and characterisation of subtle localised or disseminated parenchymal disease and mediastinal lymphadenopathy.
Primary tuberculosis:
Lymph node enlargement
o 90% in paediatric age; 30% in adults
o Ipsilateral; right-sided hilar contiguous with mediastinal lymphadenopathy
o Central low attenuation and peripheral enhancement
o May be large enough to compress adjacent airways
o Calcification of nodes in 35%
Air space consolidation
o No predilection for lung zone
o Non-specific appearance from undetectable to patchy or lobar consolidations.
o Cavitation uncommon,
in only 10-30% of cases
o Infection will become localised with caseating granuloma formation and eventually calcifies.
Pleural effusion
o More frequent in adults,
30-40% cases,
5-10% in paediatric cases
Post-primary tuberculosis (reactivation or secondary tuberculosis):
Air space consolidation
o Most common sign
o Focal or patchy
o Apical posterior upper lobes or apical lower lobes
o Bilateral in 2/3
Poorly defined nodules and linear opacities
o Centrilobular in endobronchial spread
o Randomly distributed in haematogenous spread
o Tree-in-bud sign
o Marker of disease activity
Cavities
o Hallmark of post-primary tuberculosis
o Associated with active disease
o Heals as linear or fibrotic lesions
Interlobular septal thickening
o Impairment of lymphatic drainage
Tuberculoma
o Round or oval consolidation
o Sharply marginated
o 20-30% calcified
o Satellite nodules in ~80%
Lymphadenopathies
o 1/3 cases
Pleural effusion
Miliary pulmonary tuberculosis:
- Haematogenous spread
- Small 2-3 mm nodules
- Random distribution
- Thickening of interlobular and intra-lobular septa
- Diffuse or localised ground glass opacities
Sarcoidosis
Sarcoidosis is a non-caseating granulomatous multi-system disease with a wide range of clinical and radiographic manifestations. Pulmonary and mediastinal involvement of sarcoidosis is extremely common and is seen in over 90% of patients.
Radiographic features are variable depending on the stage of the disease.
Lymphadenopathy
- Typically,
bilateral hilar and paratracheal distribution.
Classically known as the Garland triad
- Less common locations include aorto-pulmonary window,
subcarinal region and anterior mediastinum
- Atypical appearances include calcification,
asymmetric distribution and absence hilar adenopathy
- Calcification of lymph nodes is related to duration of disease,
3% calcified after 5 years and 20% after 10 years
- Calcification maybe focal,
diffuse or egg-shell
Parenchymal
- Reticulonodular opacities
- Small nodules in perilymphatic distribution (90-100%)
- Smooth/irregular margins,
well-defined,
2-5 mm in diameter
- Mainly upper and middle lobes
- Nodules increase in size (macronodules,
>5 mm) with disease progression
- Coalescence of macronodules in further progression
- Perihilar opacities,
commonly bilateral which are irregular areas of consolidation radiating towards the periphery from the hilum
- Less commonly,
large conglomerate lesions of fibrotic tissue mimicking progressive massive fibrosis
- Air space consolidation (10-20%)
- Airway disease presentation as mosaic attenuation.
- Fibrosis in end-stage disease with irregular linear and septal thickening,
traction bronchiectasis.
Honeycombing is rare.
Silicosis
Silicosis is a fibrotic pneumoconiosis caused by the inhalation of fine particles of crystalline silicon dioxide (silica). Occupations such as mining,
quarrying,
and tunneling are associated with silicosis.
Silicosis can be classified into two clinical forms based on the time of exposure to the silica.
Acute silicosis:
- Bilateral nodular opacities in centrilobular distribution
- Multifocal patchy ground glass opacities
- Consolidation
- Crazy-paving pattern
Classic silicosis:
- Multiple small nodules 2-5 mm in diameter
- Normally in upper/posterior lobes and perihilar region in a centrilobular,
paraseptal and subpleural pattern with perilymphatic distribution.
- Nodules can be calcified.
- Hilar and mediastinal lymph nodes can precede parenchymal lesions with peripheral and egg-shell calcification pattern of the lymph nodes highly suggestive of silicosis
Complicated Classic Silicosis:
- Develops as expansion and confluence of individual nodules
- Final stage of silicosis
- Large focal masses with irregular dull margins and punctate calcification,
surrounded by emphysematous tissue (progressive massive fibrosis)
- Cavitation may occur in mass larger than 5 cm
- Distortion of pulmonary architecture and vessel distribution
- Large mediastinal and perihilar nodes are visible in 1/3 cases
Pneumocystis Pneumonia (PCP)
Pneumocystis pneumonia is an atypical pulmonary infection and the most common opportunistic infection in patients with acquired immunodeficiency syndrome (AIDS) or immunocompromised patients.
This is caused by the organism pneumocystis jirovecii (previously known as pneumocystis carinii)
High resolution CT (HRCT) may be used to exclude (PCP) in patients with clinical suspicious.
HRCT findings:
- Ground-glass pattern predominantly involving perihilar or midzones
- Reticular opacities or septal thickening may be present
- Crazy-paving pattern can be seen when both ground glass and septal thickening are present
- Pneumatocoeles of varying shape,
size and wall thickness in up to 30%
- Pleural effusions are rare
- Lymphadenopathy uncommon (10%)
Amyloidosis
Amyloidosis is a heterogenous disease characterised by extracellular deposition of amyloid fibrils.
This deposition can be localized and restricted to one organ or site of the body or it can be systemic which leads to various organs and tissue involvement throughout the body.
Pulmonary amyloidosis is a rare manifestation of amyloidosis.
The disease is characterised by extracellular deposition of fibrillary protein in the lungs.
Two types of pulmonary involvement are present:
Diffuse Amyloidosis:
- Thickening of interlobular septal lines (smooth or irregular) and subpleural interstitial
- Multiple small nodules in a perilymphatic distribution
- Variable calcified,
well-defined nodules
- Heterogenous ground-glass changes
- Usually bilateral with basal or subpleural predominance
- Honeycombing
- Calcified lymphadenopathy
Localised Nodular Amyloidosis
- Single or multiple nodules,
masses or consolidations
- Nodules or masses are often calcified with variable shape and sizes
Castleman Disease
Castleman disease, also known as angiofollicular lymph node hyperplasia or giant lymph node hyperplasia,
is an uncommon benign B-cell lymphoproliferative condition.
It can affect several regions of the body although commonly described as a solitary mediastinal mass.
Two distinct subtype are unicentric,
which is more common,
localised and have minimal symptoms; and multicentric which occurs usually in immunocompromised patients causing diffuse lymphadenopathy,
anaemia,
splenomegaly and systemic inflammatory symptoms
Manifestation within the mediastinum on CT:
- solitary mediastinal mass,
infiltrative mass,
multiple lymph nodes or rarely as matted lymphadenopathy (with or without a dominant mass) in a single mediastinal compartment
- Calcification within mass in 15%
- Intense homogenous enhancement with contrast
- bilateral hilar and mediastinal lymphadenopathy
- centrilobular nodules