Procedure details
The procedure is performed in a private room,
before the injection we take a short medical history,
we explain every detail concerning the injection and the possible complications including priapism and we signed an informed consent form.
The patient is positioned supine upon the examination bed,
the penis must be placed in its anatomical position along the anterior abdominal wall and the injection of 20 microgram of Alprostadil with a 28 G needle is made at the dorsal margin of the base of penis.
Two radiologists performed the studies with high frequency transducer in a LOGIQ E9 ultrasound system.
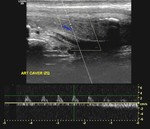
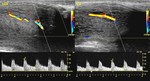
Before the injection a grey scale ultrasound is performed in both longitudinal (Fig.
1) and transverse (Fig.
2) sections to see any structural abnormality.
The scanning is performed on the ventral surface of the penis.
We evaluate the cavernosal arteries and take spectral waveforms and baseline peak systolic and end diastolic velocities (Fig.
3).
Measurements should be taken at the base of the penis were they are most reliable and most easily reproduced,
using an oblique–longitudinal approach with a Doppler angle of 60°,
or less.
After the injection we measure peak systolic and end-diastolic velocities in each cavernosal artery at 5-minute intervals for a total of 30 minutes.
Between measurements the patient is advice to self-stimulation.
Normal Doppler findings
Before the injection the penis is in flaccid state,
the systolic waveform is damped with monophasic flow and minimal diastolic component (Fig.
3).
After injection there is a normal progression of hemodynamics events and associated Doppler waveform patterns of the cavernosal arteries.
These findings must be correlated with the status of the erection.
The quality of the erection is assessed by the radiologist as no erection/flaccid,
latent,
tumescent,
full erection without rigidity and rigid.
It is also assessed by the patient as either satisfactory or not,
and recorded in the final report.
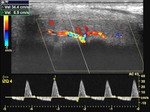
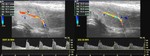
During the initial latent state,
there is a rapid increase in systolic and diastolic blood flow in the cavernosal arteries.
This flow is unidirectional,
with a pronounced forward diastolic component,
and reflects the low resistance to flow within the sinusoidal spaces (Fig.
4).
There is minimal tumescence in this phase.
Afterward,
there is an increase in blood flow with subsequent increase in pressure in the corpora cavernosa.
These changes are demonstrated with the appearance of a dichrotic notch at end systole and decline of diastolic flow (Fig.
5).
When intracavernosal and diastolic pressures are the same,
diastolic flow ceases and there is only systolic flow.
Increasing tumescence occurs in this stage.
During full erection,
intracavernosal pressure becomes greater than the arterial pressure during diastole because of the veno-oclussive mechanism.
The systolic waveform narrows and the maximal systolic velocity is achieved,
flow reversal may be seen during diastole (Fig.
6).
In the rigid phase,
intracavernosal pressure may equal or exceed arterial systolic pressure causing further narrowing of systolic envelope and normally decrease in systolic velocity.
Both systolic and diastolic flow may cease completely as the pressure in the corporal bodies approaches systolic blood pressure.
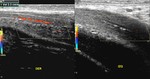
Arterial variants
Detailed scanning from the crura to the glans of the penis should be made in order to detect anatomical variations among the arterial supply.
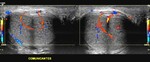
Communications between the cavernosal,
dorsal and spongiosal arteries are often found along the shaft of the penis (Fig.
7).
Although these anatomical variations do not necessarily result in arterial insufficiency they may affect arterial Doppler flow profiles with subsequent inaccurate interpretation.
For example,
systolic peak velocities of the cavernosal arteries may be significantly lower in men with a full erection if arterial collateral communications are present.
Definitions
Arterial insufficiency
Erectile dysfunction may be secondary to arterial disease,
such as focal stenosis (Fig.
8),
occlusion,
or collateral flow between arteries.
The peak systolic flow velocity is the most accurate indicator of arterial disease and the primary diagnostic criteria.
We defined Arterial insufficiency,
as a peak systolic velocity of less than 30 cm/sec (Fig.
9); there is a grey zone in the literature between 25-35 cm/sec.
Secondary diagnostic criteria for Arterial insufficiency includes asymmetry of >10 cm/s in peak systolic velocities between right and left cavernosal arteries (Fig.
10) and retrograde arterial flow.
We do not use criteria concerning the diameter of the cavernosal artery,
because it is an inaccurate method with high interobserver variability.
Veno-occlusive insufficiency (Venous leak)
Parameters to assess veno-occlusive function are end-diastolic volume and resistance index (RI).
Diagnosis of venous insufficiency on the basis of Doppler ultrasound can be made only if a patient has normal arterial function,
defined as mean peak systolic velocities above 30 cm/s.
Adequate arterial inflow,
a short duration erection,
with persistent antegrade diastolic flow >5cm/s throughout all phases is suggestive of venous leak (Fig.
11).
Resistive index is another criteria used to diagnose venous leak.
At 20 min post-injection,
RI of <0.75 is associated with venous leak (Fig.
11) in 95% of patients,
and RI >0.9 is associated with normal results in 90%.
Cavernosography is essential in patients with RI b etween 0.75 and 0.9.
Venous insufficiency can be further evaluated by using cavernosography (Fig.
12).
The demonstration of early blood flow and persistence of flow in the dorsal vein and vesicoprostatic plexus reflects veno-occlusive insufficiency.
This has 80% sensitivity and 100% specificity for venous leakage at dynamic infusion cavernosography.
Indeterminate results (Mixed)
When arterial inflow is normal but the erectile response is poor and there is antegrade diastolic flow throughout the examination,
this is called an indeterminate result or a mixed arterial and venous ED (Fig.
13).
The diagnosis of mixed arterial and venous insufficiency cannot be made using duplex Doppler sonography because venous competence cannot be assessed in a patient with arterial insufficiency.
Peyronie’s disease
It is a localized connective tissue disorder of the penis involving the tunica albuginea and erectile tissue and is characterized by the formation of fibrous tissue plaques within the tunica albuginea,
causing the penis to angulate towards the inelastic scar tissue on erection (Fig.
14,
Fig.
15).
Ultrasonography demonstrates the presence and extent of fibrotic plaques and calcification.
Sonographic findings include hyperechogenic thickening of the tunica albuginea with or without calcification.
It is well recognized that many men with Peyronie’s disease have coexistent ED,
and the pathophysiological factors include both Arterial and veno-occlusive insufficiency,
in addition to psychogenic factors and issues relating to the deformity itself.
Findings
We reviewed 148 Penile Doppler ultrasounds made between January 2015 to September 2016 and we described the imaging findings.
Among them,
45 (30%) patients had a diagnosis of Arterial insufficiency,
15 (10%) had Venous Incompetence and 6 had mixed insufficiency.
The rest of the patients had normal ultrasounds (42 cases) or structural abnormalities (40 patients).
Most patients with structural abnormalities had findings of Peyronie’s disease (16 patients); the other causes include penile fibrosis and fractures.