Liver hemangiomas have an estimated prevalence of 0.4 to 20%.
Being devoid of malignant potential,
they are usually discovered between that fourth and fifth decade of life during an abdominal imaging workup.1
Hemangiomas have been classified according to pathology into three varieties: capillary hemangioma,
cavernous hemangioma,
and mixed type hemangioma.2
Most liver hemangiomas in adults are cavernous hemangiomas3.
Their imaging features are well known,
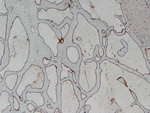
as their pathological examination (Fig.1) that reveals a characteristic focal tender mass formed by multiple vascular channels limited by a single layer of endothelial cells within a thin fibrous stroma.
In general,
the blood circulation within these tumor vessels is slow.
Morphologically,
it is a well-defined lesion possessing round or lobulated margins.
Although it may occur anywhere in the liver parenchyma,
it is more commonly seen at peripheral and sub-capsular locations,
mostly in the posterior segments of the right lobe6,
7,9.
Their size usually remains stable and can vary from a few millimeters to more than 20 cm,
a feature that has been used for its classification into small (<15 mm),
medium (15–50 mm) and large hemangiomas (>50 mm)7.
Large hemangiomas may be associated with complications in 4.5 to 19.7% of cases,
consisting of bleeding,
compressive effect on adjacent structures and torsion if pedunculated.
Liver hemangiomas have specific imaging features,
allowing its confident diagnose with cross-sectional imaging techniques.
There is,
however,
a wide range of findings that fall out of their typical description,
which are,
essentially,
due to modifications of the tumor structure or flow dynamics.
Current state of-the-art imaging techniques are more prone to demonstrating these findings,
thus,
increasing their diagnostic confidence level.