The patient age is essential,
not only regarding the recommended imaging modality for the initial workup,
as well as choosing suitable treatment.
Different screening strategies have been described,
including clinical examination alone,
selective ultrasound screening,
and universal ultrasound screening.
Selective ultrasound is indicated in patients with associated risk factors or abnormal clinical examinations (14).
Ultrasound (US) is the investigation of choice to evaluate DDH in infants younger than four to six months of age,
when capital femoral epiphyseal ossification usually occurs,
and is useful to diagnose more subtle forms of the disorder when clinical exam is equivocal (15).
It is a nonionizing,
quick,
and portable examination that furthermore offers the advantage of dynamic imaging in addition to standard static views.
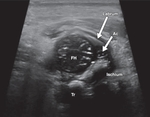
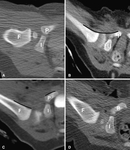
The American College of Radiology recommends that a standard US examination should be performed in two orthogonal planes: a coronal view in the standard plane at rest,
and a transverse view of the flexed hip with and without stress.
Due to the presence of physiologic laxity,
hip sonography is not performed on patients younger than 3 to 4 weeks of age,
unless there are clinical findings indicative of dislocation or significant instability (16).
(Fig.1)
As mentioned before,
it is recommended for immature hip,
and it affords direct visualization of the cartilaginous components of the hip joint.
The value of ultrasound diminishes as the femoral head ossifies; therefore,
radiography is preferable for patients 6 months of age or older,
unless the acetabulum (including the triradiate cartilage) is adequately visualized sonographically.
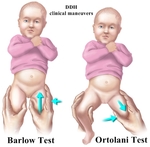
The stress maneuver (posterior push maneuver) is performed to evaluate for hip instability with the hip and knee flexed and the thigh adducted (Barlow maneuver).
If the femoral head is subluxated,
subluxable,
dislocated,
or dislocatable,
reducibility can be assessed by abducting and externally rotating the hip (Ortolani maneuver) (17).
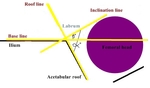
Graf method is an US classification system for DDH (Table 1),
based on three anatomic landmarks—ilial line,
triradiate cartilage,
and labrum—to obtain the α and β angles.
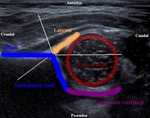
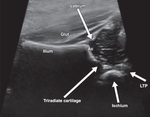
A standard plane includes a straight iliac line,
the femoral head with maximum diameter,
the tip of the echogenic acetabular labrum,
and the triradiate cartilage.
A normally positioned femoral head is more than 50% covered by the acetabulum.
DDH results in a shallow acetabulum and decreased coverage of the femoral head.(Fig.
2-7)
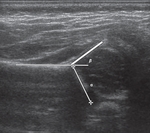
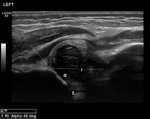
The Graf α angle is measured in the coronal plane and is defined as the angle formed between the vertical cortex of the ilium and the acetabular roof,
indicating the degree of acetabular roof coverage An α angle less than 60° is abnormal and reflects a shallow acetabulum (18).
β angle is formed by a line through the vertical ilium and the cartilaginous acetabular labrum.
Graf β angle greater than 55° is abnormal.
With superolateral femoral head displacement,
the labrum is elevated,
thereby increasing the β angle (19,
20).(Fig.
2-7)
When monitoring is performed in the Pavlik harness,
only static images are obtained.
Color Doppler imaging has been used to evaluate perfusion to the proximal femoral epiphysis although there is little literature in the setting of DDH.
After placement of the Pavlik harness,
serial follow-up hip ultrasound examinations can be performed to assess treatment response (21,
22).
Plain film radiography:
The goals of imaging in late DDH are to first make the diagnosis,
then to quantitate the abnormality,
and finally to assist in surgical planning.
Radiography of the pelvis is the standard tool to diagnose DDH after 6 months of age.
It starts to be used,
after children have reached the age of four months,
due to the fact that the femoral head ossification nucleus will be radiographically visible from fourth to sixth month of age onwards,
and so,
it becomes more reliable for detection of DDH (23).
An anteroposterior radiograph of the hips in neutral position is used to assess the morphology of the acetabulum,
ossification of the femoral head,
and position of the femoral head relative to the acetabulum.
A frog-leg lateral view is sometimes used to determine whether a subluxed hip reduces.
The morphology of the acetabulum changes with age,
with the acetabulum becoming,
from relatively steeper and straighter to more curve inferiorly along the medial and lateral margins.
In DDH,
there is delayed ossification of the femoral head and an abnormally shallow acetabulum,
thereby predisposing to subluxation and dislocation (24).
Indirect measurements of lines,
angles and signs have to be used,
in order to assess the pelvis,
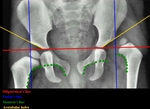
as follows: Hilgenreiner’s line is a line through the triradiate cartilages.
Perkin’s line,
drawn at the lateral margin of the acetabulum,
is perpendicular to Hilgenreiner’s line and intersecting the lateral rim of the acetabular roof.
A normally situated femoral head is localized in the inferior medial quadrant.
Shenton’s line is a C-shaped line that begins at the lesser trochanter,
goes on the infero-medial border of the femoral neck,
and connects to a line along the inner margin of the pubis.
A normal Shenton line should form a smooth arc.
In the dislocated hip,
in DDH it has a step off because the femoral neck lies cephalic to the line from the pubis.
Acetabular index is another useful measurement,
formed by the junction of Hilgenreiner’s and a line drawn along the acetabular surface (25).
A neonate should normally have an acetabular angle of less than 30°.
The acetabular angle should be less than 22° at and beyond 1year of age.
(Fig.8)
The last used parameter is the anterior center-edge angle,
which is an angle subtended by a craniocaudal line through the center of the ossified femoral head and a line from the center of the femoral head to the lateral margin of the acetabular roof.
A center edge angle less than 20° is indicative of dysplasia (24,
26).
Serial radiography can be used to track disease progression,
treatment follow- up or late complications,
such as osteoarthritis and avascular necrosis.
Arthrography:
In infants or young patients with missed DDH,
arthrography is typically performed intraoperatively at the time of reduction,
to assess the anatomy and impediments to reduction such as limbus eversion,
can be identified.
While performing the reconstructive osteotomy,
the arthrogram helps demonstrate the best position of the femur in order to obtain concentric reduction of the hip.
CT and MRI:
CT scans and MR images are useful in assessing acetabular version and therefore helpful in preoperative planning of pelvic osteotomies (27).
Compared with MRI,
CT requires shorter acquisition time and less,
if none,
anesthesia or sedation.
However,
the primary disadvantage of CT is the exposure to ionizing radiation.
Studies that compared the use of CT versus MRI to evaluate hip reduction in patients with DDH revealed that both modalities offer excellent sensitivity and specificity (28).
When using CT imaging,
it is important to realize the high radiation burden,
therefore to limit the number of CT scans,
to what is really necessary and to implement a low radiation technique (27).
The examination is reserved for difficult cases,
often in the setting of pre- or postoperative evaluation of the hip.
More commonly it is used postoperatively,
after the patient has been placed in a cast,
to define the success of reduction,
confirming the concentric reduction of the femoral head.
Preoperative assessment includes evaluation of bony acetabular morphology and the ossified femoral epiphysis as well as the femoral head position relative to the acetabulum (29,
30),
besides obtaining measurements of the acetabulum roof,
cartilage thickness,
acetabular rotation and anteversion.
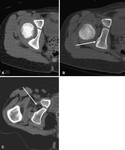
In the normally positioned hip,
when casted in the frog leg position,
there should be a smooth arc formed by the anterior aspect of the femoral neck and the anterior aspect of the pubic bone (the CT equivalent of Shenton line).
In a dislocated hip,
the line is interrupted (27).
(Fig.9)
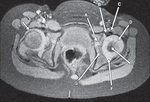
The normal acetabulum has a smoothly rounded shape with a well-defined posterior lip.
In a dysplastic hip,
the posterior acetabulum is often straightened without a well-defined posterior margin and it can also be smaller than normal.
Thickening of the fat in the medial acetabulum (pulvinar) is often seen in dysplastic hips (31).(Fig.10)
MRI indications and usage in DDH are increasing.
MRI is attractive because of the lack of ionizing radiation,
the visualization of soft tissue structures (especially the acetabular rim,
the acetabular cartilage,
and the labrum) as well as osseous structures.
Protocols differ from one institution to another and the length of MRI examinations has ranged in the literature from 3 minutes to 45 minutes.
Sequences like axial STIR,
axial and coronal T2 fast spin-echo,
fat-suppressed equivalent T1-weighted and T2-weighted are routinely obtained (23).
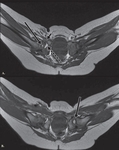
Many MRI studies are ordered in the postoperative period,
usually after reduction and spica cast placement.
Radiography cannot show the extensive soft-tissue remodeling,
and therefore MRI is particularly useful to confirm successful reduction.(Fig.11)
Spica cast placement is one of the most common indications for MRI in the setting of DDH.
After open reduction,
the hip is held in 90° flexion and partial abduction,
and the femoral head is held in position by a plaster spica cast.
The degree of abduction must be carefully controlled because too little results in redislocation and too much can increase the risk of avascular necrosis.
Neither hip should be abducted more than 55–60° (32).
MRI after spica casting is typically performed in the immediate postoperative period while patients are still under sedation.
Gadolinium is not routinely administered.
However,
if there is concern for avascular necrosis of the femoral head,
gadolinium is used to evaluate for femoral head enhancement abnormalities (33).
When characterizing DDH using MRI,
the dysplastic acetabulum should be evaluated for retroversion and degree of femoral head coverage.
There may be associated cartilaginous defects or delamination.
Delayed ossification of the femoral head can be determined by comparing the ossified nucleus of the femoral head in the affected hip with the contralateral side.
A major advantage of MRI is the ability to visualize the cartilaginous acetabulum and determine its contribution to femoral head coverage.
MRI depicts the unossified acetabular epiphysis in the ilium and underlying labrum,
therefore showing greater and more acetabular coverage than that seen on radiography alone (34).
MRI also evaluates the bony and cartilaginous acetabular indexes.
The bony acetabular index can be measured using an anteroposterior coronal view and is similar to the acetabular index measured on radiography (the Hilgenreiner line and Perkins line are drawn using the same landmarks as used on radiography; the bony acetabular index line is drawn from the Hilgenreiner line at the lateral part of the triradiate cartilage to the Perkins line at the lateral aspect of the bony acetabulum).
The angle subtended by the bony acetabular index line and the Hilgenreiner line is the bony acetabular angle.
The cartilaginous acetabular index is measured by drawing a line from the lateral part of the triradiate cartilage at the Hilgenreiner line to the lateral acetabular cartilaginous margin (the cartilaginous acetabular index line).
The cartilaginous acetabular angle is formed by the cartilaginous acetabular index line and the Hilgenreiner line (35).
MRI is particularly useful for determining ligamentous and soft-tissue abnormalities that may serve as obstacles to successful reduction .The fibro- fatty pulvinar in the acetabular fossa can become hypertrophied,
as well as ligamentum teres,
preventing adequate femoral head reduction.
The labrum should be closely checked for hypertrophy and abnormal position,
such as eversion and inversion.
Rarely,
the iliopsoas tendon may be interposed between the femoral head and acetabulum (36).
(Fig.12)