The presence of pain or swelling in the inguinal region after catheterization is the most common presentation of a FAP.
On physical examination,
there may be a palpable pulsatile mass or the presence of a systolic bruit.
However,
these signs are not present in all cases.
Any patient with pain that is disproportionate to that expected after a percutaneous procedure should undergo an imaging evaluation.
Although conventional angiography remains the standard of reference for diagnosis,
its invasiveness made noninvasive diagnostic modalities (US and CT) more relevant in the work-up.
ULTRASOUND:
The diagnostic examination of choice is duplex ultrasound with a 5- to 7-MHz linear transducer.
A lower frequency transducer (curved linear) may be required to image deeper structures,
if the puncture site is high or there is extensive hematoma.
On B-Mode scanning,
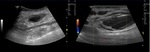
FAP appears like a complex fluid collection near or adjacent to the artery (fig.1).
FAP may have mobile internal echoes or expansions and contractions related to the cardiac cycle that are visible on real-time gray-scale sonography,
or a solid thrombus at the periphery.
Most FAP have a single cavity but multiple connecting cavities are occasionally present (fig.
4).

Fig. 1: Complex fluid collection adjacent to the artery on B-Mode.
Sometimes we can see a tract that connects the FAP chamber to the feeding vessel,
most frequently the common femoral artery.
Alone,
B-mode scanning is unable to differentiate pseudoaneurysm from hematoma.
On Color Doppler,
we can detect blood flow in the lumen of the suspected FAP (key to differentiate it from an hematoma – fig.1,2,8).
The typical pattern is a turbulent swirling flow,
known as Yin-Yang appearance (fig.2),
in which one half of the lumen is red and the other half is blue.

Fig. 2: The complex fluid collection refered on fig.1 has a Yin-Yang appearance on color doppler, which is usual on a FAP.
On Pulsed wave Doppler: When a pulsed wave Doppler is placed within the track (or neck),
a “to-and-fro” signal is obtained (fig.3),
with systolic flow on one side of the baseline and diastolic flow on the other side of the baseline.
This pattern is a hallmark for the diagnosis and it is explained because systolic flow into the aneurysm and diastolic flow out of the aneurysm occur in sequence in the neck of the pseudoaneurysm.

Fig. 3: To-and-fro Signal: we can see systolic flow on one side of the baseline and diastolic flow on the other side, in the neck of a FAP on pulsed wave Doppler.
It is important to describe the number,
size and depth of the chambers of the pseudoaneurysm,
as well as the depth,
width and length of the tract that connects the artery to the pseudoaneurysm.

Fig. 4: On B-Mode scan, we see 3 fluid collection adjacent to the artery, suggesting a multicameral FAP with 3 chambers . On color doppler, only one chamber has flow (the closest to the artery). The other two are thrombosed.
A complete examination should include imaging of the distal external iliac artery,
common femoral artery,
and proximal portions of the superficial femoral and deep femoral arteries.
ANGIO-CT:
Unhenhanced CT scans may demonstrate a low-attenuation rounded structure arising from the donor artery (pseudoaneurysm).
Intermediate or high attenuation (hemorrhage) adjacent to the pseudoaneurysm indicates rupture,
which may vary with attenuation depending on whether it is chronic or acute.
The wall of the pseudoaneurysm is usually smooth and well delineated.
Contrast-enhanced CT may demonstrate a contrast material-filled sac (fig.5,6).
However,
the entire pseudoaneurysm may not fill with contrast.
In that case,
a low attenuation area will remain within the pseudoaneurysm,
a finding that indicates partial thrombosis.
The donor artery is adjacent to the pseudoaneurysm and can usually be seen communicating with it.

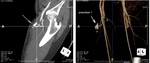
Fig. 5: This Angio-CT reveals a contrast filled linear tract originating from the right superficial femoral artery with 25mm of length and 5mm of maximum caliber, ending in a small sac measuring 7x6.5mm, suggestive of a FAP.
It is important to be aware of other possible local complications after catheterization of the femoral artery,
such as arteriovenous fistula (AVF).
AVF is an abnormal connection between an adjacent artery and vein that bypasses the normal anatomic cappilary bed.
AVF has a number of etiologies.
Acquired AVF of the lower extremity is by far the most commonly occuring AVF due to the frequency of the groin as a site for percutaneous arterial and venous access.
Long-standing AVF can lead to limb edema,
high-output heart failure,
or aneurismal degeneration of the artery.
Regarding an AVF,
B-Mode changes are rare.
On Color-Doppler,
the arterial waveform changes from the typical high-resistance triphasic pattern to the low-resistance pattern with continuous systolic and diastolic flow in the artery immediately adjacent to the fistula.
We can also see flow disturbance in the vein with haphazard arrangement of the intraluminal color and perivascular tissue vibration caused by turbulent blood flow.
Arteriovenous fistula on contrast-enhanced CT will show abnormal early filling/attenuation of an adjacent vein in the region of the arteriovenous fistula (fig.
7).

Fig. 7: Contrast-enhanced CT showing an early filling of femoral vein, near bifurcation of the femoral artery, suggestive of an AV fistula between deep femoral artery and femoral vein
TREATMENT:
Ultrasound-guided compression repair (UGCR):
Ultrasound probe must be placed on the neck of pseudoaneurysm with the intention of complete obliteration of blood flow to the pseudoaneurysm but allowing arterial perfusion to the extremity.
Pressure is applied for a period of at least 1 minute,
with the procedure repeated up to 10 times.
UGCR is safe and cost effective,
but has some drawbacks,
including long procedure time,
discomfort to the patient and high recurrence rate in anticoagulated patients.
Ultrasound-guided Thrombin Injection (UGTI):
At many institutions,
UGTI has replaced UGCR as the therapeutic method of choice for treatment of FAP.
Thrombin is injected into the sac under US guidance with a sterile technique.
Thrombin promotes convertion of inactive fibrinogen into fibrin,
leading to thrombus formation.
It has a high technical success rate (greater than 90%) and low complication rate.
Potential complications include allergy to thrombin and distal embolization.
Surgery:
It was the traditional treatment of choice,
but nowadays is seldom required in the management of FAP.
It is reserved for pseudoaneurysms with local mass effect complications such as ischemia and neuropathy,
infected pseudoaneurysms and cases in which therapy with minimally invasive techniques has failed.