Diagnosing urogenital emergencies in men is very important because,
if not made in a timely manner,
serious consequences may occur.
These include,
but are not limited to,
erectile dysfunction,
infertility and severe infectious conditions.
Ultrasound is the initial imaging method but is limited in quantifying the tissue's injury extent.
Thus, MR imaging is becoming an increasingly widespread technique,
demonstrating greater efficiency in the characterization of male urogenital lesions.
Appearance of normal penis and scrotum
Scrotum
Scrotal sac is made up of multiple layers,
including the skin,
Dartos muscle and fascial layers,
and the tunica vaginalis.
The tunica vaginalis is a two-layered serous membrane that derives from the process vaginalis of the peritoneum.
The inner visceral layer envelopes the testicles and epididymis,
whereas the parietal layer forms the inner lining of the scrotal wall [1,2].
The normal adult testis is a homogeneus oval struture,
that measures
about 5 cm in length and 3 cm in transverse diameter [1].
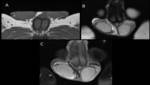
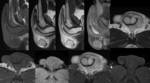
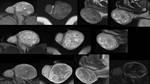
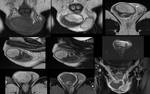
Figure 1.
MR Images of scrotal sac.
A.
Axial T1-weighted image.
B.
Coronal T2- weighted image.
C.
Post Gadolinium T1-weighted image.
At MR imaging,
the scrotal sac is typically hypointense on both T1 - and T2- weighted images.
The normal testis appears hyperintense on T2-weighted images and hypo- to isointense on T1-weighted images.
The tunica albuginea appears hypointense on T1- and T2-weighted images.
The epididymis is isointense on T1 but hypointense on T2- weighted images,
relative to the testis.
The testis and the epididymis enhance after intravenous administration of gadolinium-based contrast agents (C).
Penis
The penis is composed of paired corpora cavernosa along its dorsal aspect and a midline corpus spongiosum ventrally.
Both are surrounded by the tunica albuginea.
Proximally,
the crura of the corpora cavernosa are attached to the ischial tuberosities [1,2].
The corpora cavernosa are composed of venous sinusoids that must be filled by blood during erection.
The corpus spongiosum surrounds the penile urethra and expands distally to form the glans penis [2].
The deep fascia of the penis,
or the Buck fascia,
is superficial to the tunica albuginea.
The venous drainage is through the superficial dorsal vein and deep dorsal vein,
denominated in relation to Buck´s fascia.
The arterial supply is made by three main paired arteries.
The dorsal artery is lateral to the deep dorsal vein and supplies the glans penis and skin.
The cavernosal artery is located in the center of each corpus cavernosum and provides arterial inflow to the corpus cavernosum during erection.
The bulbourethral artery,
supplies the urethral bulb and posterior corpus spongiosum [1].
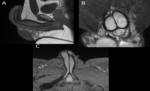
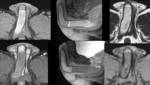
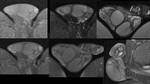
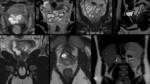
Figure 2.
In general,
the three corpora have intermediate T1-weighted and high T2-weighted signal intensity.
The corpora cavernosa are isointense relative to one another.
The corpus spongiosum may normally have flow and signal intensity characteristics different from those of the cavernosa.
The tunica albuginea and Buck fascia are imaged as low T1- and T2-weighted signal-intensity bands that surround the corporal bodies.
The tunica dartos is another T2-hypointense fascial layer.
On heavily T2-weighted images,
the collapsed muscular walls of the urethra are revealed as a band of relative hypointensity compared with the bright cavernous
spaces of the corpus spongiosum.
MAIN MALE UROGENITAL EMERGENCIES FOUND ON MRI
Penile Bruising
Intracavernosal or extratunical hematoma without tear of the tunica albuginea [5].
Clinical findings are acute pain,
swelling,
widespread ecchymosis and deviation toward the side opposite the injury [1,
5].
MR Imaging is performed for evaluation of the integrity of the tunica albuginea,
which has low signal-intensity in both T1 and T2 [5].
Characteristically,
hematomas have high signal intensity on T2- weighted images [1].
A fast and accepted protocol is the use of T2 in the three orthogonal planes and axial or sagittal T1 [4].
Additional axial and sagittal T1-weighted images after intravenous administration of contrast material may be required [5].
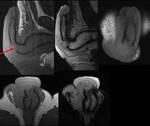
In our series,
we found eight cases of penile hematoma,
whithout rupture of the albuginea.
There was extratunical hematoma in seven studies (87.5%),
and in two of these studies (28%) there was association with intracavernous hematoma.
Hematocele was found in two studies (25%) and lesion of the suspensory ligament of the penis in on study (12.5%).
No intracavernosal bruising was found.
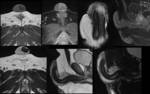
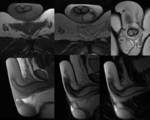
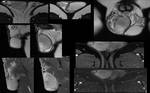
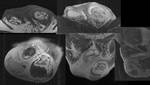
Figures 3 and 4
Penile Fractures
Rupture of the tunica albuginea,
the surrounding sheath of corpus cavernosum (5).
Typically occurs after an unusual external force applied to the penis during erection,
when the thickness of the tunica albugineas ireduces by up to 75% [3].
The main clinical findings include rapid detumescence,
pain,
swelling,
and hematoma [1].
Hematuria or dysuria may be present in patients with lesion of the corpus spongiosum that encloses the urethra ,
which occur in 10-20% of cases [16].
MR imaging is performed to evaluate the tear of the tunica albuginea,
provides superb soft-tissue definition and diagnoses adjacent struture lesion,
as urethral and corpus spongiosum injury.
As in suspected cases of penile hematoma,
the accepted protocol is the use of T2 in the three orthogonal planes and axial or sagittal T1[4].
A need for additional axial and sagittal T1-weighted images after intravenous administration of contrast material may be required [5].
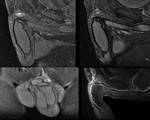
In our set,
there was 17 cases of penile fracture,
which means that we found rupture of the tunica albuginea.
All cases had a penile hematoma,
10 cases (58%) of unilateral lesion of the corpus cavernosum and 2 cases (11%) of bilateral lesion of the corpus cavernosum.
There was isolated lesion of the corpus spongiosum in 2 cases (11%),
unilateral lesion of the
corpora cavernosa in association with corpus spongiosum lesion 2 cases (11%) and in 1 case (5%) there was injury of the three bodies.
There was 3 cases (17%) of urethral injury.
Figures 5 and 6
Mondor Disease
Thrombosis or thrombophlebitis in the superficial dorsal vein of the penis.
Patients normally present with pain or discomfort,
especially with erection and a palpable cordlike lesion along the dorsum in the location of the dorsal vein.
Its cause is poorly understood.
MRI angiography can demonstrate and evaluate the extension of the thrombus and exclude a deep pelvic extension of vein thrombosis,
or overlapping of a concomitant thrombosis in another pelviperineal vein district [6].
MRI protocol: The accepted protocol is the combination of T1-weighted spin echo and T2-weighted spin echo MRI sequences to show the hyperintense thrombosed vessel and MR Angiography to detect the lack of visualization of the same vessel [6].
MRI findings: The signal intensity characteritics at MRI varies according to the time delay between the onset of thrombus formation and imaging.
In the acute stage (0–5 days) the signal intensity of femoral vein is predominantly isointense on T1-weighted images and hypointense on T2-weighted images.
In the subacute stage (6–15 days),
the signal intensity is predominantly hyperintense on both T1- and T2-weighted images.
In a chronic thrombus is typically isointense on T1-weighted and isointense or hyperintense on T2-weighted images.
The flow artifact may result in false-positive conclusions,
that is the main limitation of MRI.
[6]
Figure 7
Partial thrombosis of the corpus cavernosum
Proximal thrombosis of the corpus cavernosum [13].
The presence of a fibrous web at the level of the crurocavernosal junction is the underlying disorder in all cases allowing for entrapment of blood in the crura.
Perineal
compression is frequently seen as a provocative factor [12].
The main clinical findings are perineal swelling,
uni- or bilateral pain and/or pain during erection [12].
MR imaging should be used to identify the presence of the thrombus and
transverse septum [13].
The affected segment is distended by the thrombus and may lead to contralateral cavernous compression.
The intensity of the thrombus signal varies with time,
depending on degradation of its contained hemoglobin.
It is generally hyperintense relative to normal cavernosum in T1-weighted images and hypointense in T2-weighted images.
The lesion does not enhance [3].
MRI protocol: T1- weighted images and T2- weighted images.
In some cases
administration of contrast material may be required.
Figure 8
Testicular hematoma
Intratesticular collection of blood due to blunt trauma.
May range in age from hyperacute to chronic,
and may or may not be associated with other
testicular and extratesticular injuries [11].
The main clinical findings are severe pain,
swelling and scrotal hematoma.
MR images allows to define lesion pattern in doubtful cases and to diagnose testis rupture.
MRI protocol should include T1,
T2,
DP,
and Gadolinium contrast enhanced T1 sequences.
MRI findings: In the early stages high signal is expected in T1 - and T2-weighted images.
Over time,
they become hypointense at T2-weighted images due to the presence of hemosiderin [2].
Figure 9
Orchiepididymitis
One of the common causes of acute scrotal pain in teenagers and adults.
In general,
caused by retrograde bacterial infection from a lower urinary tract infection.
[1]
Clinically,
scrotal pain is usually relieved when the testes are elevated over the symphysis pubis (the Prehn sign).
The epididymis can be palpated as an enlarged tender structure separate from the testis.
[7]
MR imaging can be helpful in some cases to differentiate cystic lesions,
fluids,
solid masses,
fat and fibrosis.
MRI protocol should include T1 and T2 weighted sequences and in some cases,
like when differentiating benign form neoplastic cystic lesions,
Gadolinium contrast enhanced T1 sequences should be acquired.
MRI findings:
At orchitis,
the testis is usually enlarged and heterogeneous areas of low signal intensity on T2-weighted images are frequently associated.
Inhomogeneous enhancement of the testis with hypointense bands may also be seen.
Furthermore,
if the orchitis is focal,
it may mimic an intratesticular tumor at imaging.
In epididymitis,
we can find diffuse enlargement of the epididymis with a possible decrease of T2 signal intensity and hypervascularity with hyperenhancing on contrast-enhanced T1-weighted images.
A combination of these findings can be seen at orchiepididymitis.
[14,15]
Figures 10 and 11.
Testicular abscess
Testicular abscess is a possible complication of an orchiepididymitis.
It is more commonly found in immunosuppressed or diabetic patients.
The main clinical findings are pain,
fever and testicular enlargement.
MR imaging is used to help in the differential diagnosis with a testicular mass.
MR imaging protocol should include T1 and T2 multiplanar sequences, and when there is doubt,
Gadolinium contrast enhanced T1 sequences and DWI might be helpful.
MRI findings include fluid lesions wich have hypointense signal on T1- and hyperinense signal on T2-weighted images,
with a hyperintense halo on T2-weighted images.
On contrast-enhanced images,
the wall presents intense enhancement [16].
Figure 12.
Testicular Torsion
This injury is characterized by the rotation of the spermatic cord with compromised blood supply of the testis.
It may also be associated with trauma [1].
Clinically presents with sudden pain,
swelling and elevation of the testicle.
MRI is useful in cases of diagnostic doubt and differential diagnosis of solid lesions [10].
MRI protocol: T1,
T2,
T2*-weighted and DCE-MRI and post-Gd sequences.
T1-weighted images in the sagittal,
coronal,
and axial directions,
fat-suppressed (FS) T2-weighted,
heavily T2-weighted TSE,
and T2*-weighted FFE images.
DCE-MRI with a fat-suppressed TSE sequence in the coronal plane.
Although the high sensitivity (89%) and specificity (100%) of Doppler US in the diagnosis of testicular torsion has been reported,
it is not always conclusive and accurate.
MRI has been reported to provide additional information regarding testicular perfusion and differentiating testicular torsion from other scrotal disorders.
[17]
MRI findings: Decreased or lack of perfusion in DCE-MRI are diagnostic criteria for testicular torsion.
If necrosis is present,
an low or very low signal intensities with spotty or streaky patterns in fat-suppressed T2-weighted,
heavily T2-weighted,
or T2*-weighted images can be seen.
[17]
Figure 13
Zinner syndrome
Triad composed of ipsilateral renal agenesis or dysgenesis,
seminal vesicle cysts and ejaculatory duct obstruction.
[8]
Patients may be asymptomatic or present difficulty ejaculation or painful ejaculation and/or ejaculatory volume reduction.
[8]
MR imaging should be used to evaluate the relation of the ureters
with cysts of the seminal vesicle and to evaluate other malformations.
MRI protocol should include coronal,
axial,
and sagittal T2 spin-echo and axial T1 weighted images with fat saturation,
before and after gadolinium administration.
MRI findings: dilatation of the seminal vesicles,
ipsilateral renal agenesis and and seminal vesicle cyst.
[9]
Figure 14