1.
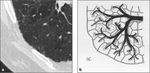
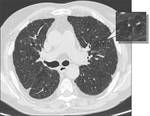
Histiocytosis X
In this disease,
cysts are produced by the progressive increase of the central air component of “star nodules”,
which arise from the proliferation of peri-bronchiolar infiltrates of Langerhans cells.
These regulate the mucosal immunity of the airways; cigarette smoking may be a determining factor in the accumulation and activation of these cells [2],
through the increased levels of cytokines such as GMCSF and βTGF.
Morphologically,
these bronchiole-centric lesions evolve from micro- and macro-nodules with a high cellular component,
in lesions with poor cellularity and fibrotic scars,
often star-shaped [3].
In advanced disease stages,
the expansion of peri-scar airspace and nodule’s cavitation become the most common evolution.
Lung cysts,
which are the most advanced disease expression,
may vary in size from one to several centimeters; they are generally lineated by thickened walls, with “bizarre” morphology and poly-lobulated contours.
These cysts also have a typical distribution,
with predominance in the lung apices and sparing of cost-phrenic angles [4] ( Fig. 1 - Fig. 2 ).
Normal values of lung function or a restrictive framework are appreciable in early stages of the disease,
while obstructive framework predominates in advanced stages [5].
2.
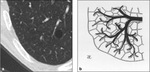
Lymphangioleiomyomatosis (LAM)
In lymphangioleiomyomatosis (LAM),
cysts develop by distension of bronchioles – which become obstructed because of proliferation of atypical hamartomatous tumor-like muscle cells in the walls of the airways.
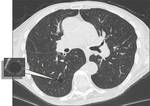
The cysts are typically rounded in shape,
with thin walls and variable diameter (small: 2-5 mm; intermediate: 1-2 cm; large: > 2 cm).
They show indifferent distribution ( Fig. 3 - Fig. 4 ) – with no zonal predilection.
Unlike hystiocytosis X,
the cost-phrenic angles involvement is pathognomonic,
and there is a trend to save the apical regions [6] ( Fig. 5 ).
LAM is a multisystemic disease that primarily affects women of childbearing age (30-35 years); this typical age disease is explained by the role exercised by the activity of estrogen,
although there are cases of the disease encountered in prepubertal and octogenarian patients [7].
Clinically this disease manifests with dyspnea and frequent pneumothorax (30-40%),
occasionally accompanied by hemoptysis [8].
Lymphatic involvement may be systemic,
with typical interest of mediastinal and abdominal regions,
where the detection of renal angiomyolipomas is 50%.
LAM also occurs in patients with tuberous sclerosis (TSC-LAM complex),
and “sporadic” form in patients who do not have tuberous sclerosis (S-LAM) [9].
3.
Lymphocytic Interstitial Pneumonia (LIP)
LIP is a benign lymphoproliferative disease,
characterized by diffuse lymphocyte and plasma cell infiltrates.
In Lymphocytic Interstitial Pneumonia,
cysts result from dilatation of the airways – which is a consequence of bronchial stenosis due to lymphocytic infiltration of the bronchiolar wall; these formations have thin walls and regular distribution predominantly in peri-vascular regions,
also with involvement of the central portion of the lung.
They show variables size,
ranging from a few millimeters up to 3 centimeters,
and persist even after treatment ( Fig. 6 - Fig. 7 ).
LIP is often associated with collagen vascular disorders,
such as Sjögren’s syndrome and systemic lupus erythematosus (LES) and AIDS; it is less frequently observed in association with autoimmune thyroiditis,
gravis myasthenia,
pernicious anemia,
chronic active hepatitis and with Castleman’s disease.
Non-infectious form typically occurs in women in the fifth decade,
with coughing and wheezing [10].
4.
Desquamative Interstitial Pneumonia (DIP)
Desquamative interstitial pneumonia (DIP) is a lung disease caused by accumulation and intra-alveolar aggregation of macrophages [11],
with a few desquamated alveolar epithelial cells,
in the distal branches of the airways.
This disease occurs after exposure to cigarette smoke: indeed,
it has been included into the group of smoking related interstitial diseases.
Clinically,
the disease manifests with dyspnea and cough in patients aged between 30 and 40 years; it is more encountered in females.
The radiological pattern is characterized by areas of parenchymal attenuation “ground glass” with basal and peripheral distribution,
where there are micro-cysts or honeycombing [12] ( Fig. 8 - Fig. 9 ),
pathognomonic signs of parenchymal fibrosis.
5.
Neurofibromatosis
The neurofibromatosis are a group of autosomal dominant disorders,
characterized by multiple schwannomas on all nerve trunks; they are associated with gliomas of optic nerves,
skin changes (such as the cafe-au-lait spots),
visceral formations (mediastinal and digestive system tumors),
meningeal tumors and bone lesions.
Multifocal lung cysts rarely can be appreciated,
predominantly in upper lobes; other thoracic events include subcutaneous neurofibromas,
“ribbon” ribs,
meningoceles,
mediastinal masses and pulmonary fibrosis.
6.
Diseases showing “Honeycombing”
The honeycomb appearance is defined by the presence of multiple cysts arranged in several layers,
ranging between 3-10 mm,
although they can reach 2.5 cm.
Based on cyst’s size,
a macro-honeycombing > 4 mm ( Fig. 10 - Fig. 11 ) and a micro-honeycombing < 4 mm ( Fig. 12 - Fig. 13 ) have been described.
These cysts may be characterized by a thick wall (1-3 mm diameter),
often filled with mucin and inflammatory cells: this feature is pathognomonic of late-stage disease ( Fig. 10 - Fig. 11 ).
The most common cause of honeycombing is UIP,
followed by nonspecific interstitial pneumonia (NSIP) ( Fig. 13 ),
chronic hypersensitivity pneumonitis (HP chronic) ( Fig. 14 ),
sarcoidosis,
asbestosis and the post-actinic fibrosis.
The Usual Interstitial Pneumonia (UIP) is an interstitial pulmonary disease in which “definitive” diagnosis is based onthe detection of reticulations – with or without bronchiectasis – and multiple air cysts resembling a honeycomb appearance.
These findings are mainly distributed in the basal and subpleural lungs.
UIP is usually diagnosed in patients older than 50 years,
especially male,
smokers or ex-smokers.
Symptoms are non-specific: worsening dyspnea,
non-productive cough and digital clubbing in 25% of cases.
The disease worsens over a period of years,
in absence of specific pharmacological therapy,
with periods of relative stability and periods of acute deterioration.
7.
Bronchiectasis and pneumatocele
Cystic bronchiectasis are irreversible abnormal dilatation of the bronchial tree branches and can be localized or diffused; they may be encountered in chronic infectious diseases,
in sarcoidosis ( Fig. 15 ),
in atelectasis due to occlusion lumen,
or in congenital bronchial diseases [13].
The pneumatocele is a cyst-like lesion of the pulmonary parenchyma,
characterized by thin-walled and air content; it is usually found in some acute pneumonias,
after trauma or inhalation of hydrocarbon fluids; in acute phase,
the pneumatocele shows a thick wall,
instead in the chronic phase the wall becomes thinner ( Fig. 16 - Fig. 17 ). The development of a post-traumatic pneumatocele is often preceded by laceration and contusion of the lung parenchyma.
The pathogenetic mechanism is based on parenchymal necrosis and airways “valve” obstruction [14].
It occurs mainly in upper lobes and it regresses after therapy.
8.
Emphysema and alpha1-antitrypsin deficiency
Emphysema is a pathological condition characterized by destruction of the alveolar wall [15],
with a permanent dilatation of the distal airways and terminal bronchioles [16]; it is commonly classified according to the acinar involvement: proximal (centrilobular),
distal (paraseptal) or full (panacinar).
Centrilobular emphysema is the most common kind of emphysema and cigarette smoking is an important cause.
Radiologically,
it appears as minute rounded centrilobular areas of reduced parenchymal attenuation,
without appreciable wall,
with few millimeters diameter; they are more localized in the upper lobes [17].
The central vascular core (centrilobular artery) in the cystic area of low parenchyma attenuation is the pathognomonic finding for a correct diagnostic interpretation ( Fig. 18 - Fig. 19 ).
Paraseptal emphysema involves predominantly alveoli,
bronchial tree duct and distal bags,
and it is radiologically characterized by subpleural and peri-bronchovascular low parenchymal attenuation areas,
separated by intact interlobular septa [16] ( Fig. 20 - Fig. 21 ).
Congenital alpha1 anti-trypsin deficiency is a genetic autosomal recessive condition with variable penetrance and expressivity.
It is due to mutation of SERPINA1 gene,
coding for the alpha1-antrypsin glycoprotein,
to inhibit the neutrophil elastase.
This deficiency determines traditionally panlobular emphysema,
localized in the basal regions,
due to gravitation vascular flow distribution ( Fig. 22 - Fig. 23 ).
9.
Cystic fibrosis
Cystic fibrosis is a multisystem autosomal recessive disorder,
that mainly relates to children and young adults [18].
It is characterized by an anomalous sodium and chloride transport through the epitelium in all exocrine tissues,
resulting in viscous secretions in the pulmonary,
pancreatic,
hepatic,
intestinal and genital tract [19].
Radiologically,
there are multiple cystic bronchiectasis,
filled by mucous secretion [20],
and focal air-trapping areas,
which are a result of small airways obstructive disease [21] ( Fig. 24 - Fig. 25 ).
10.
Cysts from aging
The lungs are affected by aging,
with progressive development of air space enlargement [22].
Various studies have demonstrated high prevalence of thin-walled cysts in many elderly individuals (depicted on 25% of 75-year -old patients) [23] ( Fig. 26 - Fig. 27 ); these cysts have a wide distribution and have no correlation with cigarette smoking.
-old patients) [23] ( Fig. 26 - Fig. 27 ); these cysts have a wide distribution and have no correlation with cigarette smoking.