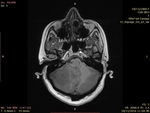
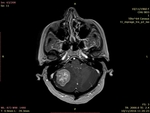
MRI protocol includes :
- T1 Weighted MPRAGE sequences obtained in the axial plan.
- Axial FLAIR,
T2 spin echo and gradient echo.
- Diffusion Weighted Imaging (DWI) in axial plan.
- Injection of Gadolinium is required.
- Perfusion and spectroscopy are performed according to the kind of lesions on 3 Tesla MRI.
Posterior fossa tumors in adults were divided depending on the location:
Extra-axial lesions,
mainly in cerebellopontine angle: schwannoma,
meningioma,
archnoïd and epidermoïd cysts.
Intra-axial lesions:
- Cerebellum: metastasis,
hemangioblastoma,
pilocystic astrocytoma,
and medulloblastoma.
- Brainstemglioma.
- Fourth ventricle: ependymoma and papilloma.
I. Extra-axial tumors
1. Vestibular schwannoma
General Features
- Vestibular schwannoma (VS) is a benign tumor arising from Schwann cells that wrap vestibular branches of CNS in CPA-lAC
It represents 60–90% of all CPA tumors
- It is especially common in patients with neurofibromatosis type 2,
in which 96% of patients will have bilateral tumors.
- Age: 30 - 70 years.
- Sensorineural hearing loss is the most common presentation,
frequently accompanied by tinnitus and dysequilibrium.
Imaging findings (figures 3 - 4)
- CPA / lAC mass for which the shape varies with its location: cylindrical with convex medial margin when it is confined to the IAC or spherical when larger and extends into the cisternal space
- Small lesions measure 2 to 10 mm and larger ones measure up to 5 cm.
- Most (85%) VS have acute angles at the bone tumor interface.
On MR imaging,
the tumor is:
- TlWI: usually iso to hypointense.
- T2WI: hyperintense.
- T2WI FS: High-resolution T2 or CISS: "Filling defect" in hypersignal CSF of CPA cistern :
Small lesion: Ovoid filling defect
Large lesion: "Ice cream on cone" filling defect
- Tl WI C+ FS: VS shows intense enhancement centered on porus acusticus,
it may be heterogeneous by cystic degeneration (15%,
common feature in larger schwannomas).
- T2* GRE: calcifications and hemorrhage are rare.
Differential diagnosis
- Meningioma: eccentric to porus acusticus; broad dural base with dural "tails".
- Metastases: may be bilateral meningeal involvement.
Be aware of misdiagnosing as NF2.
(figure 5)
- Epidermoid cyst: insinuating morphology,
no-enhancing mass,
diffusion restriction (high signal).
2.
Meningioma
General Features
- Benign unencapsulated neoplasm arising from meningothelial arachnoid cells of CPA-lAC dura,
usually arising from the posterior surface of the petrous bone.
- It is the second most common (3%) mass of the CPA.
- 10% of CPA meningioma occur in posterior fossa.
- It is larger compared to the vestibular schwannoma,
and rarely directly involves the internal auditory canal.
- Extension into the middle cranial fossa is common.
Imaging Finding
- CPA dural-based enhancing mass with dural "tails".
- 75% of them show an obtuse angle at the bone-tumor interface,
asymmetric to lAC porus acusticus .
- 3 morphologies were distinguished:
"Mushroom cap" (hemispherical) with broad base towards posterior petrous wall (75%).
Plaque-like (en plaque) (20%).
Ovoid mass (5%).
On MR imaging,
the tumor is:
- T1WI: generally isointense.
- T2WI: variable signal,
mostly hyperintense (figure 6)
- T2* GRE: Calcifications may "bloom"
- TlWI C+: intense homogeneous enhancement,
with“dural tail” in 50–70% of cases (reaction of the dura).
- MRS: elevated alanine at short TE.
Differential diagnosis
- Vestibular Schwannoma: intracanalicular then CPA extension,
centered on porus acusticus
- Metastases:· may be bilateral,
multifocal meningeal involvement.
- Intracranial trigeminal schwannoma: ovoid enhancing mass centered in Meckel cave.
3. Epidermoid cyst
General features
- Epidemoid cysts account for approximately 0.5% to 1% of all intracranial tumors and develop from aberrant ectodermal embryonic tissue in the neural groove.
- They are benign,
slow-growing congenital neoplasms that contain waxy keratinous material that originated from retained ectodermal remnants.
- Most commonly located in the CPA (40-50 %) and parasellar region (30%).
MRI findings
Epidermoid cysts generally appear as well-circumscribed,
homogenous,
lobulated masses:
- T1WI: usually hyperintense to CSF (changes are thought to occur because of a relatively high protein concentration)
- T2WI: variable,
but often isointense to CSF
- FLAIR: usually does not completely null.
- DWI: characteristic hyperintensity.
ADC =brain parenchyma.
- T1WI +C: none.
Differential diagnosis
- Arachnoid Cyst: · isointense to CSF on all standard sequences,
completely nulls on FLAIR,
smooth surface.
- Cystic neoplasm: attenuation of signal intensity not that of CSF,
often enhances
- Dermoid cyst: usually at or near midline,
resembles fat and contains dermal appendages; often ruptured.
4. Arachnoid cyst
General features
- Intra-arachnoid CSF-filled sac without communication with ventricular system.
- Arachnoid cysts of the posterior fossa are uncommon.
Most of them are located in the middle cranial fossa.
- They are usually located in the CPA,
the cerebellum and the fourth ventricle.
MRI findings
Sharply demarcated round/ovoid extra-axial cyst:
- TlWI: isointense with CSF.
- T2Wl: lsointense with CSF
- FLAIR: Suppresses completely.
(figure 7)
- TlWl C+: does not enhance.
- T2* GRE: no "blooming" unless hemorrhage present (rare)
Differential diagnosis
- Epidermoid cyst: scalloped margins,
insinuating morphology; no suppression on FLAIR,
restricted diffusion.
- Dermoid cyst: usually at or near midline,
resembles fat and contains dermal appendages; often ruptured.
- Cystic Neoplasm: often enhances.
II. Intra-axial tumors
A. Cerebellum
1. Hemangioblastoma
General features
- Most common primary intra-axial tumor of the posterior fossa in adults (WHO grade 1).
- Rare tumors of the CNS which constitutes about 1 to 2.5% tumors and 7.3% of those arising within the posterior fossa.
- Location: posterior fossa (90-95%): cerebellar hemispheres (80%),
vermis (15%).
- Capillary hemangioblastoma is the most frequent manifestation of von Hippel-Lindau (VHL) disease.
The overall prognosis for patients with a capillary hemangioblastoma is good with approximately 85% surviving for at least 5 years.
- There were distinguished four variants of HMB:
Solid tumor (25–30%).
(figures 9 - 10)
Large,
smooth-walled cyst with transparent-yellow content,
with a mural nodule on one of the walls (55–65%).
Mixed tumor: a large node with small cyst (4%).
Cystic tumor (6%).
MRI findings
Most (60%) capillary hemangioblastomas manifest as a cystic mass with a mural nodule,
which is usually small in size (<1.5 cm diameter) and near the pial surface.
In the classic “cyst with a mural nodule” form: (figure 11)
- T1WI:
Nodule isointense +/- flow voids
Cyst hyperintense compared to CSF
- T2WI: Both nodule and cyst are hyperintense.
- FLAIR: Both cyst and nodule hyperintense
- T2* GRE: May "bloom" if blood products present
- DWI: Cyst slightly or markedly low signal
- TlWI C+: Nodule enhances strongly,
intensely.
Cyst wall usually does not enhance.
- On MRS: elevation of the Lip–Lac complex peak is seen,
and other brain metabolite peaks are almost absent.
Calcification is not seen in capillary hemangioblastomas.
Mild enhancement of the cyst wall is also seen on occasion.
Differential diagnosis
- Pilocytic astrocytoma: usually in children
- Metastasis: very vascular,
often multiple solid component +++.
2. Pilocytic astrocytoma
General features
- More common in children and younger adults (age <40),
circumscribed margins,
solid or mixed solid-cystic tumor.
- It accounts for 5–10% of all cerebral gliomas and 85% of all cerebellar astrocytomas.
- Age: before 20 years with,
peak: birth - 9 years.
- The vast majority of patients have an excellent prognosis with 5 years survival rate of 86–100 % after surgical resection.
MRI Findings
The classic aspect of a cerebellar pilocytic astrocytoma is a well-circumscribed,
predominantly cystic with mural nodule,
located in cerebellum in 60% of cases.
MRI shows:
- TlWI
A mural nodule: iso/hypointense.
Cyst: iso to slightly hyperintense to CSF
- T2WI and FLAIR
Solid portion: hyperintense to GM (increased amounts of free water contained within the neoplasm)
Cyst: iso-/hyperintense to CSF do not suppress in FLAIR.
Surrounding vasogenic edema and calcification are occasionally noted.
- DWl: Solid tumor has similar diffusivity to GM
- TlWI C+: intense and heterogeneous enhancement of solid portion.
The cyst wall usually does not enhance.
- MRS: elevated choline and lactate decreased NAA.
Differential diagnosis
- Hemangioblastoma
- Metastasis
3. Medulloblastoma
General features
- Medulloblastoma is a hypercellular embryonal primitive neuroepithelial tumor,
representing the most common brain tumors in children and accounting for up to 30 % of all pediatric CNS tumors.
- They are rare in adults,
accounting for 1 to 3 % of all adult primary brain tumors.
- Age: < 40 years old; males are more commonly affected.
- It tends to involve more the cerebellar hemispheres.
- Medulloblastoma has 4 histologic variants: the desmoplastic variant is more associated with lateral hemispheric masses in adults; and has also 4 molecular variants: the sonic hedgehog (SHH) pathway is activated in most adult cases.
- Greater prevalence of late recurrence.
MRI findings
Location: cerebellar hemisphere.
Size: 1-3 cm
On MR imaging,
an even greater degree of heterogeneity among these lesions is noted:
- T1WI: iso to hypointensity.
- T2WI: variable signal intensity.
- Flair: hyperintense to brain.
- DWI: restricted diffusion,
low ADC
- TlWI C+: important heterogeneous enhancement,
Contrast essential to detect CSF dissemination,
up to 1/3 have subarachnoid metastatic disease at presentation.
Contrast-enhanced MR of spine (entire neuraxis) is required.
Recurrence of medulloblastoma most commonly manifests as leptomeningeal enhancement or focal parenchymal nodular enhancement within the brain.
- MRS: decreased NAA,
elevated choline lactate usually present; elevation in Tau (short TE).
Cr/Cho < 0.75 and mI/NAA < 2.1 indicative for MB (DD ependymoma).
Differential diagnosis
- Cerebellar metastasis: usually multiple.
- Choroid plexus papilloma: if important size involving hemispheres.
- Ependymoma: DWl: relatively low cellularity: high ADC.
4. Metastasis
General features
- Metastasis is the most common intra-axial neoplasm of posterior fossa in adults.
- About 20 % of all intracranial metastases occur in the posterior fossa.
- The most common tumors metastasizing to the brain originate from tumors of the lung,
breast,
malignant melanoma,
gastrointestinal and genitourinary tumors.
- Multiple lesions are the hallmark,
but in the posterior fossa there is a high incidence of solitary lesions (25-50%).
MRI findings (figures 12- 13)
- T1WI: most metastases are iso to hypointense (hyperintense areas as seen in case of hemorrhage).
- T2WI: more frequently hyperintense.
Presence of peritumoral edema (hyerintense T2WI/FLAIR).
N.B: Metastatic melanoma are hyperintense on T1WI and hypointense on T2WI (paramagnetic,
stable free radicals within melanin).
- T1WI + C: contrast enhancement can be homogeneous,
nodular,
inhomogeneous or ring-like.
Metastates can be solitary and very large with a necrotic central portion mimicking agressive primary tumors; in other case they can be very small and numerous and high-dose gadolinium examination can be indicated.
B.
Brainstem gliomas
General features
- Brainstem tumors are defined as lesions occurring in the midbrain,
the pons or the medulla oblongata.
- They are rare in adults and account only 1 to 2 % of intra-cranial gliomas.
-In adults,
a low grade glioma phenotype predominates,
which is the feature that likely explains their better prognosis compared to that in children.
- Because biopsies are rarely performed,
classifications based on the radiological aspects of MRI results have been proposes to establish treatment strategies to determine outcomes:
a) Diffuse intrinsic low grade: (WHO grades II–III): younger adults (age <40),
diffuse: >50% brainstem,
they account for most brainstem gliomas.
b) Enhancing malignant glioma: (WHO grades III–IV): adults (>40y),
infratentorial infiltrative glioblastoma.
c) Focal tectal glioma: younger adults (age <40),
focal: <50% brainstem diameter,
account for 8% of brainstem gliomas.
d) Exophytic glioma: extremely rare in adults.
MRI findings
a. Diffuse intrinsic low grade glioma
It usually reveals a diffuse enlargement of the brainstem with:
- T1WI: hypointense
- T2WI and FLAIR: hyperintense areas.
- TWI+C: these tumors are diffusely infiltrative and do not enhance after the administration of gadolinium.
- MRS: currently,
single-voxel MRS is the technique used to study diffuse brainstem lesions,
particularly in pontine lesions greater than 2 cm. More recently,
the application of the 3T multivoxel MRS has improved the spatial resolution of this technique when acquisition times of 12–15 minutes are used.
MRS shows an elevation in Cho/NAA ratio and in the Cho/creatine ratio.
The creatine/NAA ratio was abnormal in because of the loss of the NAA signal.
Lesions may be limited to a brainstem segment (midbrain,
pons,
or medulla oblongata),
or they may infiltrate other brainstem segments or adjacent regions,
such as the cerebellum or thalamus.
b. Enhacing malignant glioma
- T1WI: hypointense
- T2WI/ FLAIR: hyperintense
- T1WI+ C: heterogeneous contrast-enhancing infiltrative mass.
- Often with intratumoral necrosis and peritumoral edema.
- Despite the fact that MRS may be helpful,
it is important to underline that,
in contrast to children,
the radiological pattern of malignant brainstem gliomas in adults is non-specific.
c. Focal tectal glioma
- These tumors are centered in the dorsal midbrain,
occupying less than 50% of the brainstem diameter,
and are well-defined lesions without enhancement.
- The periaqueductal location and long periods of stability are classic features of focal tectal gliomas.
- Acute obstructive hydrocephalus and an intracranial hemorrhage can constitute the first clinical manifestation.
C. Fourth ventricle
1. Ependymoma
General features
- Slow-growing tumor of ependymal cells lining the fourth ventricle,
that accounts for only 2% - 5% of all intracranial tumors,
- 45 % of ependymomas in adults.
- In adults,
it involves the spinal cord (arising from central canal) more often than the brain (2%–6% of adult brain tumors).
CSF dissemination complicates 3% to 15% of intracranial ependymomas.
- Ependymal tumors are classified as subependymomas (WHO grade I),
myxopapillary ependymoma (WHO grade I),
ependymomas (WHO grade II),
and anaplastic ependymomas (WHO grade III).
MRI findings
It has an irregular shape in posterior fossa according to shape of ventricle or cisterns and it measures 2 to 4 cm usually.
If a tumor is large and occludes the fourth ventricle and foramen of Magendie,
then hydrocephalus often develops.
On MRI,
it appears as an heterogeneous mass with uneven surface filling,
which may occupy the cavity of the fourth ventricle and expand into the cisterns magna or the lateral pontine cistern.
- Tl WI : heterogeneous,
iso to hypointense; hyperintense foci (calcifications,
blood products,
cystic foci) are common
- T2WI: heterogeneous,
iso- to hyperintense;
- FLAIR: can show sharp interface between tumor and CSF
- T2* GRE: “blooming" of hypointense calcifications foci
- DWl: relatively low cellularity,
high ADC
- TlWI C+: typically heterogeneous.
- MRS: decreased NAA,
elevated Cho and lactate.
Differential diagnosis
- Medulloblastoma (PNET-MB): homogeneous mass which arises from roof of 4th ventricle,
more distinct interface with floor,
low ADC,
high cellularity.
- Choroid plexus papilloma: vigorously enhancing intra-ventricular tumor.
- Brainstem glioma: may project into 4th ventricle; infiltrating mass expanding brainstem,
homogeneous signal on MR.
2. Papilloma of choroid plexus
General features
- Choroid plexus tumors arise from the neuroepithelial lining and include papilloma (WHO grade I),
atypical papilloma (WHO grade II) and carcinoma (WHO grade III).
-They are rare and affect children (2 – 4% of pediatric brain tumors) more frequently than adults (0.5% of adult brain tumors).
MR imaging
Location: Posterior fossa (fourth ventricle) is more frequently seen adults,
approximately 70 % of cases.
“Cauliflower” like mass,
often of remarkable size at diagnosis.
Hydrocephalus common.
On MR imaging,
choroid plexus papilloma appears as a circumscribed and lobular intraventricular lobulated mass:
- T1WI: iso to hypointense
- T2WI: iso to hyperintense mass,
+/- vascular flow voids.
- T2* GRE: foci of diminished signal if calcifications or blood products are present.
- T1WI + C: intense and homogeneous enhancement.
- Post-contrast MR imaging of the spine is recommended to exclude the possibility of seeding from choroid plexus papilloma on follow-up post-operative studies.
- MRA: flow-related signal within mass; enlarged choroidal artery.
- MRS: NAA absent,
mild elevated choline,
lactate if necrotic