- Leptomeningeal involvement
Leptomeningeal involvement occurs with predilection for the basilar cisterns in about 40% of patients with neurosarcoidosis.
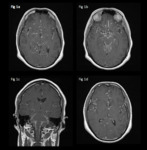
Gadolinium enhancement can be diffuse or nodular on post-contrast T1 weighted MRI (Fig. 1).
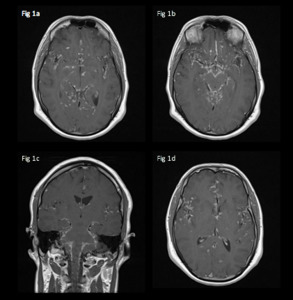
Fig. 1: 24-year-old male admitted with headaches, nausea and fatigue.
Axial (a, b and d) and coronal (c) T1 post gadolinium show linear and nodular leptomeningeal thickening and enhancement predominantly at the base of the skull but also in the Sylvian fissures bilaterally, within the surface sulci and around the brainstem.
- Hypothalamic-Pituitary involvement
The pituitary gland,
infundibulum,
or hypothalamus are affected in about 18% of patients with neurosarcoidosis.
The most common patterns of involvement on MRI are an enhancing mass or thickening and enhancement of the infundibulum.
These findings may occur in isolation or in combination with basilar leptomeningeal involvement.
Perivascular spread can be encountered,
producing enhancing foci that are remote from the brain surface (Fig. 2,
Fig. 3).
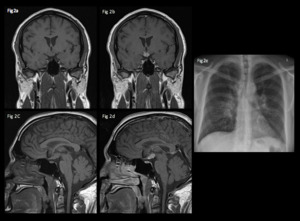
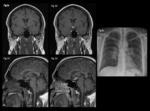
Fig. 2: 30 year old, admitted with fatigue and weight loss.
Coronal and sagittal T1 pre (a, c) and post (b, d) gadolinium show an enhancing mass in the infundibulum.
A chest radiograph (e) in the same patient shows bilateral hilar lymphadenopathy and multiple lung nodules consistent with pulmonary sarcoidosis.
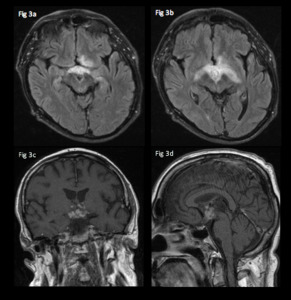
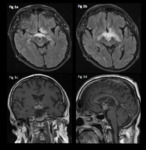
Fig. 3: 48 year-old male admitted with visual disturbance.
Axial FLAIR images (a,b)show expansion and vasogenic oedema affecting the optic chiasm and tracts bilaterally as a result of the hypothalamic inflammatory granuloma shown as multiple small enhancing and coalescing nodules on coronal (c) and sagittal (d) T1 post gadolinium.
- Cranial nerve involvement.
Cranial nerves are affected in up to 50% of patients with neurosarcoidosis.
While any cranial nerve can be affected,
facial nerve palsy is most commonly found clinically and the optic nerve is the most common cranial nerve to appear abnormal on MRI.
The affected cranial nerve shows enhancement and thickening with or without associated leptomeningeal involvement (Fig. 4).
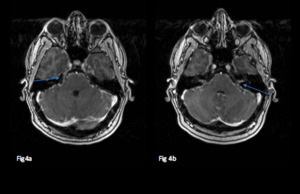
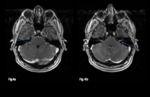
Fig. 4: 50-year-old admitted with facial nerve deficits.
Axial T1 post gadolinium imaging shows thickening and abnormal enhancement of the trigeminal nerves (a) and VII and VIII nerve complexes (b).
Dural involvement occurs in 43% of patients with neurosarcoidosis.
The posterior cranial fossa is most commonly involved.
Lesions can be diffuse,
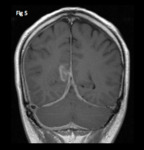
plaque-like (associated with strong enhancement of the dura) or focal (Fig. 5).
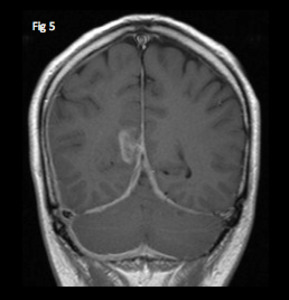
Fig. 5: Coronal T1 with contrast shows diffuse thickening and enhancement of the falx cerebri posteriorly and of the tentorium cerebelli. There is more focal “mass-like” meningeal enhancement in the right parasagittal occipital region.
- Non-enhancing T2 white matter hyperintensities
Signal hyperintensities within the cerebral white matter on T2 are variable and depend on the amount of fibrocollagenous material present.
Alone,
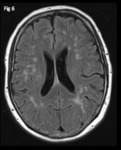
these are entirely non-specific but in combination with other imaging findings they can be suggestive of neurosarcoidosis (Fig. 6).
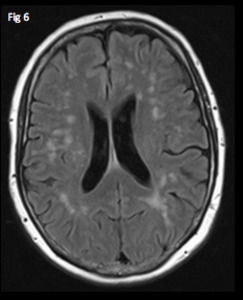
Fig. 6: Axial FLAIR image at the level of the lateral ventricles shows multiple non-specific T2 hyperintensities in the cerebral white matter in a patient with known sarcoidosis.
- Spine intramedullary involvement
Intramedullary involvement occurs in up to 25% of patients with neurosarcoidosis.
Lesions can cause fusiform cord enlargement in the acute phase and may lead to atrophy with chronicity.
However,
the typical MRI features are regions of increased T2 signal with multifocal leptomeningeal and peripheral medullary enhancement (Fig. 7, Fig. 8).
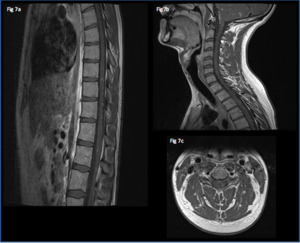
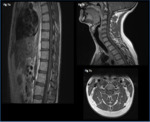
Fig. 7: 27 year old, admitted with weight loss, headaches and ataxia.
Sagittal (a,b) and axial (c) T1 post gadolinium imaging shows peripheral intramedullary and leptomeningeal spinal cord involvement. Note also the posterior fossa leptomeningeal involvement on sagittal imaging of the cervical spine (b).
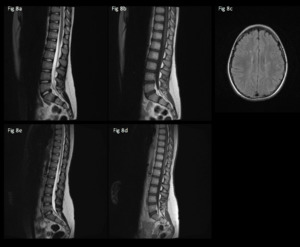
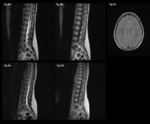
Fig. 8: 12 year-old admitted with lower limb weakness, brisk reflexes and paraesthesia.
Sagittal T2 (a) shows multiple tiny punctate hyperintensities within the lower cord, which enhance on T1 post gadolinium (b).
Axial FLAIR (c) in the same patient shows non-specific white matter hyperintensities.
Sagittal T2 (e) and T1 post gadolinium (d) performed after treatment show complete resolution.