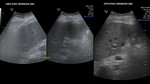
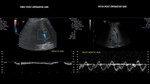
Expected post-operative changes at grayscale US
The ultrasound study is preferred for early evaluation of patients with orthotopic liver transplantation due to its availability,
low cost and security.
Doppler ultrasound of the liver post-surgical varies within the first days,
the findings can be alarming but should not be misinterpreted.
(7)
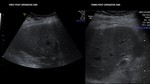
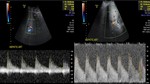
The normal liver transplant has a homogeneous or slightly heterogeneous pattern at gray scale imaging.(5) Fig 4. The starry sky appearance may result from reperfusion edema in the early postoperative period.
(7) Fig 5.
Transient focal areas of increased hepatic echogenicity may result from intraparenchymal haemorrhage secondary to manipulation or from grafting material obtained in patients involved in motor vehicle accidents (7) Pneumobilia is another normal finding in patients with enterobiliary anastomosis.
(8)
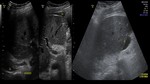
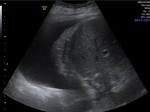
In the early postoperative period,
there is usually a small amount of free intraabdominal fluid in the perihepatic space,
which commonly resolves in 7–10 days.
(5) Fig 6.
Pleural effusion sometimes is observed frequently.
Fig 7.
Expected early post-operative changes at doppler US
Hepatic artery
Arterial peak systolic velocity (PSV)
Evaluation of hepatic artery with doppler ultrasound is important because significant hepatic arterial stenosis or hepatic arterial thrombosis can progress to early graft failure or acute bile duct necrosis-biliary sepsis.(9) Early detection can improve the management and complications.
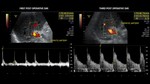
Normal hepatic artery Doppler US waveform shows rapid systolic upstroke,
with a systolic acceleration time of less 80 msec and continuous diastolic flow.
The arterial peak systolic velocity less than 200 cm/seg.
(10) However,
elevated hepatic arterial velocity is a normal transient postoperative phenomenon.(7) These normal allografts also had a wide range of peak systolic velocities of 13.2–367 cm/sec.(10)
At the site of arterial anastomosis,
edema may cause luminal narrowing,
which mimics stenosis and results in elevated velocity at the anastomosis site.
As postsurgical edema resolves,
elevated arterial velocity decreases within a few days.(7) Fig 8.
Hepatic arterial resistive index
After transplantation,
normal hepatic arterial RI ranges from 0.55 to 0.8.
However,
in the immediate postoperative period,
almost one-half of patients have an elevated RI or absent forward diastolic flow that returns to a normal waveform within a few days.(10) Fig 9.
It is important to distinguish transient elevated RI from hepatic arterial thrombosis.
Elevated RIs in both the intra and extrahepatic branches are more likely to be transient.
(7) At immediate postoperative imaging,
absent diastolic flow with very low peak systolic velocity is a more ominous finding than absent diastolic flow with normal peak systolic velocity and should be closely monitored for arterial complications.
(7,9)
Decreased RI and Tardus Parvus
Decreased RI is a good indicator for hepatic arterial complications However,
the combination of the tardus parvus pattern and an optimal PSV cutoff (48 cm/seg) greatly improved the predictive positive value and reduced the false-positive rate in the diagnosis of hepatic arterial stenosis.
(9) Tardus parvus pattern (RI,
0.5 and systolic acceleration time 0.08 second) of the hepatic artery at Doppler US.(9) Fig 10.
Even in the presence of tardus parvus waveform,
an alarming finding,
caution should be taken before making a diagnosis of arterial stenosis during immediate postoperative imaging findings,
especially in patients with good hepatic function.
In these cases,
requesting close follow-up imaging may be prudent.(7)
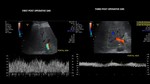
Portal vein
Portal vein shows a laminar flow,
anterograde,
hepatopetal,
with slight ondulations that are secondary to breaths,
however,
up to 43% of the patients in the early postoperative period,
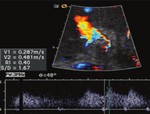
the flow is helicoidal in spiral. On US color Doppler can be observed alternate bands between red and blue.
It is important to distinguish between ellipsoidal flow and bidirectional flow,
which can be seen in portal hypertension and thrombosis.(10) Fig 11.
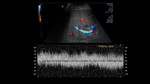
The reduction in portal venous resistance in the immediate post-transplant period can produce increased portal venous flow.
This manifests as a high portal venous velocity,
which gradually normalizes in the postoperative period,
as the body adapts to the new hemodynamics.(8) Fig 12 .
Another cause of increased portal venous velocity in the immediate post-OLT period is transient compression of the portal vein by postoperative edema or fluid.
(7)
A wide range of portal venous velocities (15–400 cm/sec) have been reported in the immediate post-OLT period in patients with no vascular complications.(10) Due to these hemodynamic findings,
physicians should not be persuaded to make a diagnosis of portal venous stenosis on the basis of increased velocity at immediate postoperative Doppler US.
Whereas normal portal venous flow demonstrates mild respiratory variation,
transient pulsatile flow may be present in the postoperative period.(7)
Hepatic Veins and inferior vena cava.
Normal flow of the hepatic veins presents a triphasic flow due to the transmission of heart heartbeats.
The flow of the inferior vena cava is also triphasic,
it is more pronounced.(10)
In the early postoperative period the loss of the phasicity is usually normal,
without clinical significance.
However,
if the venous waves are triphasic initially seen and become monophasic in the follow-up studies may be by acute rejection,
thrombosis or compression of the inferior vena cava.(10)
Monophasic or biphasic waveforms are seen in the postoperative period,
secondary to graft edema or compression by the adjacent fluid collection.
This usually normalizes on follow-up studies.
(7,8) Fig 13.
Follow-up of expected changes
In our institution,
the decision to perform follow up doppler US or angiography in patients with no improvement on subsequent controls depends on the severity of the abnormality and the patient clinical status.
The follow-up frequency of Doppler US in patients with abnormal findings on initial images has not been established and differs for each institution.
(7)
The current protocol evaluation orthotopic liver transplantation at our hospital consists in ultrasound exploration during the first,
third and fifth postsurgical day and periodic subsequent evaluations.