This poster is published under an
open license. Please read the
disclaimer for further details.
Keywords:
Breast, Oncology, Interventional non-vascular, MR, Ultrasound, Image manipulation / Reconstruction, Biopsy, Computer Applications-Detection, diagnosis, Diagnostic procedure, Neoplasia
Authors:
N. Capozzi , A. Fausto, D. Spina, F. Gentili, F. G. Mazzei, M. A. Mazzei, L. Volterrani; Siena/IT
DOI:
10.1594/ecr2017/C-2868
Methods and materials
During a five-year period we enrolled 115 consecutive patients (53±12 years,
range 24-79) with 157 breast additional lesions only MR-detected and negative at second-look US. The same radiologist who has read MR exams performed all second-look US exams.
The exclusion criterion was gynecomastia evaluated with two morphologic measurements.
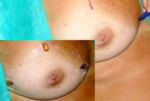
After positioning three pairs of markers made by soft gel capsules of natural d-alpha-tocopherol (Vitamin E),
over a corresponding blue surgical skin marker all the patient underwent supine MR Fig. 2.
We used a 1.5 T MR unit (Signa Twin Speed Hdxt; GE Healthcare) T1w fat sat dynamic sequence (1 pre and 4 post-constrast sequences; high resolution 1 mm slice) before and after intravenous injection of 0.05 mmol/kg of gadobenate dimeglumine (Multihance,
Bracco Diagnostics Inc.) at a rate of 2ml/s followed by a flush of 20 ml saline solution at a rate of 2ml/s.
Patients were in supine position using a body coil.
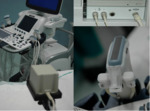
Breast US and MR co-registrations (LogiQ E9; GE Healthcare) were obtained and maintained by means of a dual electromagnetic systems consisting of a magnetic transmitter positioned close to the patient and two small magnetic receivers positioned on a linear probe bracket Fig. 3.
A large core biopsy sampling using US with V Nav was used for BI-RADS 3 or more lesions.
A carbon clip was positioned at the end of the procedure as a tissue marker (BiomarC,
Carbon Medical Technologies Inc.).
Pathology or two-year follow-up were the standard of reference.