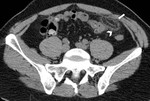
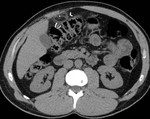
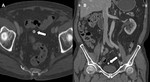
A non invasive diagnosis of epiploic appendagitis can be done at contrast-enhanced CT by identifying the most common findings.
► On contrast CT imaging,
acute epiploic appendagitis may appear as a fat-density ovoid structure,
usually 1–4 cm in diameter,
abutting anteriorly large bowel wall.
This is expression of an infarcted or inflamed epiploic appendage (Fig.1) [1].

Fig. 1: Primary epiploic appendagitis in 43-year-old man with clinical diagnosis of presumed colonic diverticulitis. Axial non-contrast CT scan shows pericolonic fatty lesion (arrow) that abuts colon-sigmoid junction.
► A high-density rim (2-3mm thick) surrounding the ovoid mass represents the inflamed visceral peritoneal covering of the epiploic appendage and it is a suggestive radiological feature of primary epiploic appendagitis (Fig.2); thickening of the parietal peritoneum has also been described as expression of spread of inflammation [1].
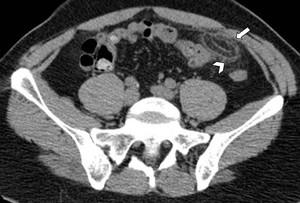
Fig. 2: Acute epiploic appendagitis near the sigmoid colon in 41-year-old man. Axial non-contrast CT image shows inflamed fatty ovoid mass with hyperattenuating rim (arrow) and adjacent fat stranding (arrowhead).
► Segmental thickening of adjacent colonic wall is usually minimal compared to the amount of adjacent mesentery inflammation involvement,
which appears at imaging whit a characteristic fat stranding sign (Fig.3) [1].
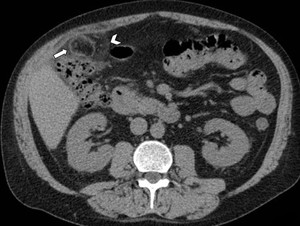
Fig. 3: Acute epiploic appendagitis in a 53-year-old man. Axial non-contrast CT image shows a lesion (arrow) with fat density and surrounding inflammation (arrowhead) that abuts the hepatic flexure of transverse colon.
► A central high-attenuation focus within the fat structure (“central dot sign”) is suggestive of thrombosed vascular pedicle within the inflamed epiploic appendix (Fig.4).
Albeit this is a pathognomonic sign,
its finding is occasional,
so that its absence does not exclude a diagnosis of epiploic appendagitis [1].

Fig. 4: Acute epiploic appendagitis with a hyperattenuating center in a 40-year-old man. Axial non-contrast CT image demonstrates a fatty ovoid lesion with hyperattenuated rim (curved arrow) that abuts the transverse colon and has a central focal area of hyperattenuation (arrow) with surrounding fat inflammation (arrowhead).
► Epiploic appendages may also be present in the vermiform appendix and are usually smaller than those on the serosal surface of the colon.
However,
epiploic appendagitis of the vermiform appendix is rare and only few cases have been previously reported in the literature (Fig.5) [4].
It is important to distinguish this condition from an acute appendicitis to avoid unnecessary procedures.

Fig. 5: Acute epiploic appendagitis near the vermiform appendix in 39-year-old woman. Curved reformatted non-contrast CT image shows an oval lesion of fat attenuation with a hyperattenuating rim (arrow), that is depending directly from the vermiform appendix (curved arrow).
► Within 6 months after an episode of acute epiploic appendagitis,
the CT features generally resolve [5].
Chronically,
an infarcted epiploic appendix may undergo aseptic fat necrosis and gradually transform into a fibrotic or calcified mass.
It may remain connected to the colonic serosa or it may detach from it,
appearing as a mobile,
loose calcified body within the penitoneal cavity (Fig.6).
Many of these lesions are discovered incidentally during abdominal surgery,
autopsy or CT scan performed for unrelated conditions.
Most of amputated appendices epiploicae are oval,
ranged from 1 to 7 centimeters in diameter,
with patchy “popcorn” or peripheral “eggshell” patterns of calcification; they can be mistaken at imaging for a calcified uterine fibroid,
ovarian cyst,
teratoma,
lymph node or urinary calculus [2].

Fig. 6: Calcified, amputated epiploic appendix in a 81-year-old man. A) Axial CT scan of abdomen (bone window) shows a calcified, ring-like mass (arrow) medial to the sigmoid colon. It was initially mistaken for a mesenteric lymph node. B) Coronal reformatted CT image of the same patient shows the peritoneal loose body in the pelvic cavity (arrow).