Type:
Educational Exhibit
Keywords:
Obstruction / Occlusion, Haemodynamics / Flow dynamics, Cardiac Assist Devices, Instrumentation, Education, Complications, CT, Conventional radiography, Interventional vascular, Cardiovascular system, Arteries / Aorta
Authors:
B. Gibney1, J. Ryan1, A. N. Murphy1, C. D. Gillespie 2, C. A. Ridge1; 1Dublin/IE, 2Dublin 7/IE
DOI:
10.1594/ecr2018/C-0028
Findings and procedure details
Complications in the setting of IABP therapy may relate to direct complications from balloon insertion,
positioning,
malfunctioning or removal,
or they may relate to the underlying cardiovascular compromise for which the use of counter-pulsation therapy was required.
This can include myocardial infarction,
pulmonary oedema and acute kidney injury.
The presence of peripheral arterial disease has been the most consistent and reproducible predictor of complications [4,5,6].
In a large multinational registry,
7% of 16,909 IABP recipients experienced IABP-related complication.
Of these,
2.6% had major complications,
including major bleeding in 0.8%,
limb-threatening ischemia in 0.9%,
limb amputation in 0.1%,
and IABP-related death in 0.05% [4].
Importantly,
serious complications associated with IABP use may not be clinically apparent at time of occurrence.
A review of 45 necropsy patients who have had an IABP inserted and who died within 105 days of the time of balloon insertion identified unsuspected dissection of the aortoiliac axis in nine patients and clinically silent arterial emboli in 3 patients.
They concluded that out of the 20 complications (in 16 patients) only 4 (20 %) had been suspected before death [7].
When positioned correctly,
IABP therapy can increase splanchnic and renal perfusion [8,
9] and improve post-operative renal function [10].
However,
covering of the orifices of the branches of the abdominal aorta by an IABP has been shown to significantly reduce visceral and renal blood flow [11,12].
A retrospective review of 645 patients with IABP therapy found malpostioning of the IABP tip (>5cm below the aortic arch) occurred in 11.1% and severe malpositioning (>10cm below the aortic arch) occurred in 6.7%.
Both were significantly more likely to develop major complications compared to correctly positioned IABPs and severe malpositoning was more associated with major complications than the presence of shock [13] (Fig 2).
Even when the IABP appears correctly positioned on chest radiograph there is a risk of visceral arterial compromise.
A study of 107 patients found weak correlation between patient height/BMI and the distances between sub-clavian artery and renal/visceral branches [14].
They observed a mismatch in 73.8% with regard to the aorta length and the length of commercially available IABP devices,
described as “anatomic-balloon mismatch”.
Another study of 63 patients who required thoracoabdominal CT with IABP in situ found that,
despite radiographically satisfactory balloon placement in 96.8%,
placement was appropriate in only 38.1% on CT.
“Anatomic-balloon” mismatch was identified in 68% with high levels of visceral arterial compromise [15] (Fig 3 & 4).
Complications:
- Thrombocytopenia,
defined as platelets <150,000/mL or >50 % decrease from baseline,
is the most common complication of IABP use though in this group thrombocytopenia is generally mild and is not associated with an increased risk of major bleeding or in-hospital death [1].
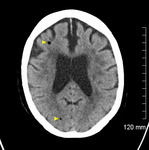
- Peripheral vascular ischaemia can occur due to embolization or local thrombosis.
Ischaemic limbs were reported in 2% of cases in a 2016 meta-analysis [16].
(Fig 5)
- Haemorrhage and pseudo-aneurysm formation.
Pseudoaneurysms are reported with 8F IABP sheath in 1.2% of cases [17].
Major haemorrhage is reported in 2% [16].
(Fig 6)
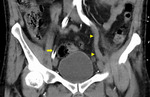
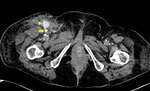
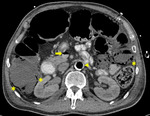
- Visceral arterial ischaemia.
IABP therapy was a significant risk factor for post operative mesenteric ischaemia in 5 of 7 papers in a 2014 review [18].
(Fig 7 & 8)
- Balloon rupture or leak is a rare complication which can result in air embolism [19] (Fig 9).
Helium often used in balloons due to its low density facilitating rapid balloon cycling.
Helium is insoluble in blood and more lethal than carbon dioxide when embolised [20].
Treatment options include hyperbaric oxygen or increasing cerebral perfusion pressure with pressors.