Of a total of 218 patients who underwent IVCF insertion during the selected years,
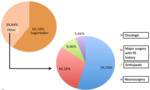
133 patients had a prophylactic indication (Figure 2).
Of these patients,
in the majority,
corresponding to 60.1% (80 patients),
it was placed as part of the comprehensive management protocol in patients undergoing cytoreductive surgery combined with intraperitoneal chemotherapy with hyperthermia (Sugarbaker).
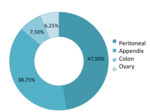
The majority of these patients (47.5%) had surgery indication for secondary neoplastic peritoneal compromise with primary gastrointestinal or genitourinary tract neoplasms.
In the other patients,
without secondary peritoneal compromise,
the indication for surgery was prophylactic by a primary appendix (38.75%),
colon (7.5%) or ovary (6.25%) neoplasm (Figure 3).
In the long-term follow-up of this group of patients,
it was detected that only 11 of them (13.75%) presented thrombotic complications; all had pulmonary thromboembolism despite filter placement and in 2 of the cases it was associated with deep venous thrombosis.
In the remaining 53 cases,
the main indications were in order of frequency (Figure 2): major surgery in oncological patients (54.7%),
another type of major surgical intervention in patients with a history of pulmonary thromboembolism (30.18%),
orthopedic surgery (9,4%) and neurosurgery (5.66%).
In the oncological patients,
the majority had a gastrointestinal tract neoplasm: 20.68% gastric cancer,
10.34% colon cancer,
6.89% pancreatic cancer,
3.44% mucinous carcinoma of the cecal appendix and 3,
44% peritoneal primary neoplasia (the latter not undergoing Sugarbaker surgery).
The other patients had primary hematological involvement (10.34%),
ovarian (6.89%),
prostatic (6.89%),
renal (6.89%),
central nervous system (6.89%),
head and neck (3.44%) and breast (3.44%) neoplasms.
Only 3 patients (10.34%) were affected by more than one neoplasm.
Among patients who underwent another type of major surgical intervention and with a history of pulmonary thromboembolism,
75% were due to indeterminate surgery and the rest due to valve replacement (6.25%),
myocardial revascularization (6.25%),
peripheral vascular surgery (6.25%) and inguinal herniorrhaphy (6.25%).
In orthopedic surgery patients,
the majority (40%) were patients undergoing hip replacement,
20% under spinal surgery,
20% lower limb amputation and 20% other unspecified surgery.
Finally,
the patients undergoing neurosurgery,
which were only 3,
were taken to decortication and drainage of multiple subdural hematomas.
None of these 53 patients presented thrombotic complications during long-term follow-up.
In our series,
we didn´t have indications such as severe trauma,
head trauma,
spinal cord injury,
multiple fractures or bariatric surgery,
which are other prophylactic indications reported in the literature.