Differential diagnosis of ON pathology can be broadly divided into congenital,
inflammatory/infectious,
neoplastic,
vascular and others.
In the following section,
we will be exploring the main pathologies related to each one of these topics and their main imaging features.
1.CONGENITAL:
1.1 Optic nerve aplasia/hypoplasia
ON aplasia is a rare,
congenital developmental anomaly,
comprising of the absence of ON,
central retinal vessels and ganglion cells while the ON hypoplasia is characterized by small optic disc.
Both conditions can affect one or both eyes and are generally accompanied by other CNS anomalies,
such as hydrocephalus,
white or gray matter development abnormalities,
corpus callosal abnormalities,
and septo-optic dysplasia (SOD) [3].
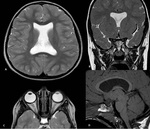
1.2 Septo-optic dysplasia
SOD is diagnosed when two or more features of the classical triad is present: ON hypoplasia,
pituitary hormone abnormalities and midline brain defects (septum pellucidum and/or corpus callosum agenesis) (Fig 4).
The most common clinical feature is hypopituitarism [4].
1.3 Optic nerve hypertrophy
Differential diagnosis of optic nerve hypertrophy is broad and includes both congenital and acquired etiologies,
such as neurofibromatosis 1 (NF1),
histiocytic or granulomatous infiltration,
leukemia,
ON sheath meningioma,
medulloepithelioma,
orbital pseudotumor,
optic neuritis as well as Krabbe disease [5].
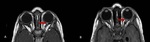
1.4 Optic nerve colobomas
Optic colobomas are focal defects in the posterior globe at the optic nerve head insertion and are related (although distinct from) Morning glory disc anomaly (a defect with glial tissue and pigmented rim) and peripapillary staphyloma (a congenital scleral defect at optic nerve head) (Fig 5).
2.
INFLAMMATORY/ INFECTIOUS
2.1 Optic neuritis associated with multiple sclerosis (ME) and acute disseminated encephalomyelitis (ADEM)
Optic neuritis is the inflammation of the ON,
it is divided into infectious and demyelinating,
the latter being the most common.
Clinically,
it causes pain in the orbit,
usually worse with eye movement and associated with visual loss.
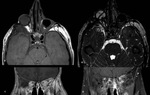
On imaging,
it shows unilateral ON swelling with a hyperintense signal on STIR/T2 fat-saturated images and intense homogeneous enhancement [6],
better identified in the retrobulbar intraorbital segment of the ON.
Chronically the nerve will appear atrophied.
The 2016 MAGNIMS MRI considers the involvement of at least one ON as a disease dissemination in space criteria for ME,
along with ≥3 periventricular,
≥ cortical-juxtacortical,
≥ infratentorial,
≥ spinal cord lesions.
The dissemination in time can be established by either a new lesion when compared to a previous scan (T2 bright lesion and/or gadolinium-enhancing) or the presence of enhancing lesion and a non-enhancing T2 bright lesion on any one scan [7].
ADEM is a multifocal,
demyelinating disorder of the CNS occurring most commonly after vaccination or viral infections,
that can also affect the ON.
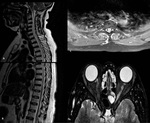
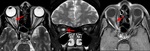
2.2 NMOSD
NMO,
also known as Devic Disease,
is an autoimmune demyelinating disease induced by a specific autoantibody,
NMO-IgG,
directed against aquaporin-4 water channels,
preferably affecting the ON and spinal cord.
The majority of NMO lesions are longitudinally extensive measuring at least 17.6 mm in length and involving at least three optic nerve segments while in MS lesions,
the ON involvement is more commonly focal in one segment anteriorly [8].
In the spine,
the lesions are longitudinally extensive (> 3 vertebral segments) and tend to involve the entire cross section of cord (Fig 6).
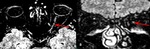
2.3 ON associated with Systemic lupus erythematosus (SLE)
Although keratoconjunctivitis sicca (“dry-eye syndrome”) is the most common orbital condition in SLE,
optic nerve involvement and retinal vaso-occlusion are more dramatic.
The patients present significant clinical improvement after the administration of intravenous corticosteroids (Fig 7).
2.2 Inflammatory perineuritis
It is an uncommon,
usually idiopathic,
a variety of orbital inflammatory disease with enhancement around,
rather than within,
the optic nerve (tram-track sign on axial and doughnut sign on coronal images) and "streaky" fat with or without extraocular muscle enhancement [1].
2.3 Orbital pseudotumor
Orbital pseudotumor is an idiopathic inflammatory process of the orbit with unknown etiology and vastly associated with many inflammatory/infectious diseases.
On imaging,
there is diffuse orbital mass,
extraocular muscles thickening with the involvement of their tendinous insertions and involvement of lacrimal glands and optic nerve with hypointense signal on T1 and T2 and marked post-contrast enhancement.
Tolosa Hunt syndrome occurs when the inflammatory soft tissue is confined to the superior orbital fissure and cavernous sinus.
As in SLE,
there is a dramatic improvement with corticosteroids.
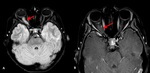
2.4 Sarcoidosis
Optic nerve involvement occurs in the intraorbital segment or the chiasma.
The nerves are enlarged,
thickened,
and hyperintense on STIR/T2 fat-saturated images with post-contrast enhancement (Fig 8).
There can be associated brain and orbital findings,
such as periorbital inflammation,
lacrimal gland enlargement and nodular leptomeningeal enhancement [9].
3.
NEOPLASTIC
3.1 Optic nerve glioma
ON glioma is the most common neoplastic disease in the ON.
They occur typically in children where they account for 15% of supratentorial tumors and often happen in patients with neurofibromatosis type 1 (NF1) [10].
On imaging,
they are isointense on T1 and iso-to-hyperintense on T2W images and shows variable contrast enhancement.
In NF1,
they tend to be multifocal,
bilateral and the ON is the commonest site of involvement.
In non-NF1 patients,
however,
the chiasma is most commonly involved and cystic components are commonly seen (Fig 9).
3.2 Optic nerve sheath meningioma
ON sheath meningiomas account for a third of the ON neoplasms.
They are benign tumors arising from the arachnoid cap cells of the optic nerve sheath,
most being directly extensions from intracranial meningiomas.
On imaging,
they appear most often as masses within the optic nerve,
isointense to grey matter on both T1 and T2W imaging,
with intense enhancement which clashes with the non-enhancing optic nerve ("tram-track sign" on axials or "non-enhancing dot sign" on coronals) [11].
The tram-track sign (Fig 10) refers to the parallel thickening and enhancement around the optic nerve and,
although most often seen in meningioma,
is also seen in orbital pseudotumor,
sarcoidosis,
leukemia,
lymphoma,
metastasis,
and perineuritis [12].
3.3 Metastases
Isolated metastases to ON are extremely rare and they appear similar to primary ON tumors.
The history of previous malignancy (most often breast and lung carcinomas) can help diagnosis.
3.4 Retinoblastoma spread
Retinoblastoma is the most common intraocular neoplasm found in childhood and may direct spread into the orbit,
along with the ON,
into the brain or into the subarachnoid space resulting in leptomeningeal metastases.
Involvement of ON beyond lamina cribrosa is associated with poor prognosis [13].
On imaging,
it presents with disruption of linear enhancement at choroidoretinal or thickening of enhancing choroidoretinal complexes in prelaminar ON involvement and focal ON enhancement and/thickening of the postlaminar ON (Fig 11).
Importantly,
radiation therapy for retinoblastoma may result in atrophy of the optic nerve and optic chiasm (Fig 12).
4.
VASCULAR
4.1 Ischemic optic neuropathy
The Anterior ischemic optic neuropathy (AION) occurs when ischemia/infarction involves optic disc while the posterior ischemic optic neuropathy (PION) involves the optic nerve and/or optic chiasma.
Although imaging plays no role in diagnosis,
the MRI may help when ON or MS must be excluded and in patients with an unusual course.
5.
OTHERS
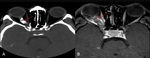
5.1 Trauma
Trauma to the ON can be direct when the ON fibers are anatomically disrupted or indirect secondary to fracture fragments in craniofacial trauma.
CT scan of the orbit is the imaging of choice (Fig 13).
5.2 Toxic optic neuropathy
Several toxins can affect the ON,
causing visual loss,
such as tobacco,
ethanol,
methanol,
ethambutol,
isoniazid,
chloroquine and digitals.
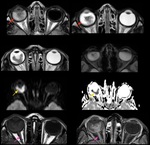
5.2 Idiopathic intracranial hypertension
Idiopathic intracranial hypertension is a diagnosis of exclusion,
characterized by elevated CSF pressure and papilledema without focal neurological deficit most often occurs in middle-aged females.
On imaging,
the most suggestive findings are flattening of posterior sclera,
intraocular optic nerve protrusion,
enlarged optic nerve sheath,
increased tortuosity of optic nerve,
partially empty sella,
and venous sinus stenosis in patients with clinical findings of IIH,
such as headaches,
visual problems (transient or gradual visual loss),
pulse-synchronous tinnitus,
photopsia and eye pain (Fig 14).
5.3 Secondary compressive optic atrophy
Secondary compression of the ON resulting in nerve atrophy can be caused by tumors (most commonly pituitary macroadenoma,
meningioma,
craniopharyngioma,
and gliomas),
vascular diseases (such as tortuous vessels) and thyroid orbitopathy.
5.5 Glaucoma
Glaucoma is an intraocular pathology characterized by an elevated intraocular pressure that can result in optic nerve atrophy of the intraocular segment [14].