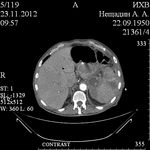
33 patients with PP locaated in spleen were estimated (ultrasound,
CT or/and MRI) and treated (1985-2016).
Men prevailed (84,8%),
average age - 45±7 years.
All patients underwent ultrasound with an evaluation of the spleen parenchyma,
intraorganic blood flow,
spleen artery and vein.
The condition of the pancreas and retroperitoneal space was assessed without fail.
In the presence of any disputable diagnostic issues,
as well as with difficulty in visualization with ultrasound,
computer tomography (CT) or magnetic resonance imaging (MRI) was performed.
All formations were verified as PP after detection of a high level of amylase in the contents of the cyst.
The diameter of spleen PP varied from 3 to 12 cm.
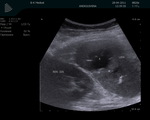
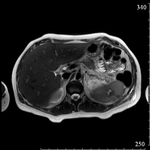
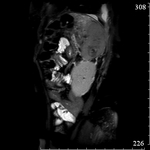
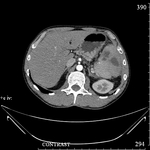
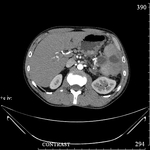
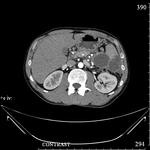
The lesions were divided into two groups according to ultrasound.
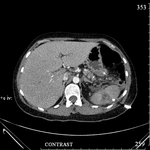
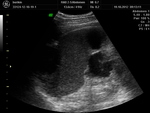
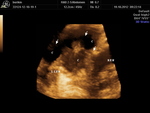
The first group (20 (60.6%) patients): the lesions that had heterogeneous fluid contents of different echogenicity,
however,
no sequesters in the cavity were detected in any case,
the capsule formation was not significant (Fig.
1-3).
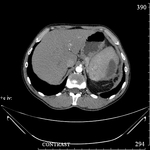
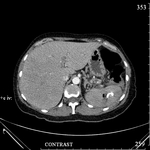
The second group (13 (39.4%) patients): the lesions that also had liquid contents more distinctly heterogeneous,
noted the presence of gas bubbles,
a solid component (the structure of the formation of the "honeycomb" type).
All this indicated an infection.
With prolonged existence and suppuration,
a capsule of uneven thickness was visualized.
In 13 (39.4%) patients more than 50% of the parenchyma of the spleen was replaced by cellular non-uniform cavities.
In the treatment of patients,
they were divided into two groups.
In the first group of patients,
with safe access,
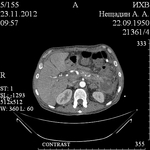
the first stage was percutaneous drainage of PP (Fig.
4-9).
Percutaneous drainage was the final method of treatment in 10 (50.0%) patients,
while 2 required stenting of the pancreatic duct.
The remaining 10 patients in the delayed period required surgery: due to the developed bleeding into the cyst cavity - in 2; due to pronounced changes in the tail of the pancreas (the presence of additional cysts and calculous pancreatitis causing clinical symptoms,
persisting pancreatic fistula) in 8.
In all patients with transcutaneous treatment,
the content of PP revealed a high level of amylase,
while bacteriological confirmation of the growth of which -or any microflora in the content was not obligate.
In the second group PP,
in fact,
they were abscesses,
they had sequestration in the cavity or cellular nature of the lesion,
or the lesion area exceeded 50%,
which made it unnecessary for percutaneous drainage.
It should be noted that,
as a rule,
these patients had a significant lesion of the distal pancreas,
giving clinical symptoms.
Given the presence of the spleen abscess and pronounced changes in the distal pancreas,
in all cases performed a distal resection of the pancreas with splenectomy (Fig.
10-13).
The level of postoperative complications was 43.4%,
while Clavien-Dindo class III - 34.7%,
that is,
8 patients in the postoperative period required additional puncture-drainage treatment.
Lethality was 0%.