Type:
Educational Exhibit
Keywords:
Abdomen, Pancreas, Paediatric, MR, Decision analysis, Congenital, Trauma, Neoplasia, MR-Cholangiography
Authors:
E. Boninsegna, S. Mehrabi, L. sartori, A. J. Cybulski, R. Manfredi, R. Pozzi-Mucelli; Verona/IT
DOI:
10.1594/ecr2018/C-0298
Findings and procedure details
We have revised the most important articles regarding pancreatic diseases in children.
The first imaging examination in these patients is ultrasonography; the second line examination is often MR,
because of its high contrast resolution and lack of ionizing radiations.
The most common pediatric pancreatic disease is pancreatitis,
with an incidence of 1 case per 10.000 children/year [6]; about 25% of them develop severe life-threatening complications [7].
In these patients MR has a double role: to assess the severity of the process and to identify the triggering cause.
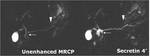
Usually only subtle signs of inflammation are present: mild glandular enlargement,
signal intensity alterations due to parenchymal edema,
peripancreatic fat-stranding and mild pancreatic ductal irregularities at MRCP (Figure 1).
About one quarter of the patients with inflammatory disease presents a severe condition,
with large pseudocysts,
regions of walled-off necrosis and foci of hemorrhage.
Whilst gallstones are more common in the adult population,
children and teenagers are also affected,
especially patients with a high body mass index [8; 9].
MRI,
including MRCP sequences,
is the most accurate non-invasive imaging technique to detect biliary tract stones and enables planning of the most suitable therapeutic approach [10].
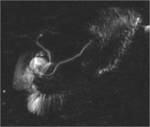
In 15% of population anatomical anomalies are demonstrated at MRCP; the vast majority present pancreas divisum [11] (Figure 2).
It results from failure of fusion of the dorsal and ventral pancreatic ducts during embryological life,
causing drainage of most of the gland through the duct of Santorini and the minor papilla; these patients often present with impaired outflow of the pancreatic secretions resulting in parenchymal damage.
The annular pancreas malformation is rarely observed; it is a ring of pancreatic tissue continuous with the head of the gland surrounding the duodenum and can cause impaired juice outflow or partial duodenum obstruction [7; 12].
Pancreatic tumors in the pediatric population are rare and histologically different from neoplasms encountered in adults [13].
Very young children can be affected by a pancreatoblastoma,
which presents as large asymptomatic abdominal masses; on imaging it has well-defined margins,
solid and cystic components and rapid contrast enhancement [13].
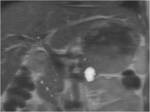
Young patients affected by von Hippel–Lindau (VHL) disease tend to develop pancreatic serous simple cysts and serous cystadenomas,
but also other pancreatic neoplasms with a malignant potential [14; 15] (Figure 3); periodic surveillance with MR is therefore recommended.
In children affected by multiple endocrine neoplasia type 1 (MEN1) pancreatic neuroendocrine tumors (NETs) can be depicted; they are well demarcated homogeneous lesions with intense contrast enhancement; cystic components and calcifications can also be present [16].
Solid pseudopapillary neoplasms (SPNs) usually affect adolescent girls and young women; they present at imaging as large circumscribed mass lesions with hemorrhagic and cystic change [17].
Pancreatic injury during a blunt trauma is more common in children than in adults because of their thinner abdominal walls.
The mechanism is attributed to compression of the pancreas against the rigid spinal column [18].
Often signs of trauma may be difficult to visualize on CT immediately after the incident; MR signs includes fluid collections,
intra-glandular hematomas and pancreatic lacerations.