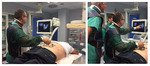
An ultrasound scanner with Virtual Navigator (VN) was used (ESAOTE Italy).
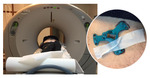
Prone position lumbar spine 3D CT or MRI were obtained with a reference device fixed on the sacral region in 20 patients with FJ degenerative syndrome.
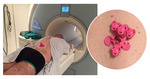
The active patient reference devices were placed on the patient’s body prior to CT (Fig 1) or MRI (Fig 2) series acquisition.
Within a period of 2 months,
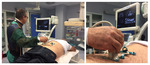
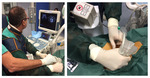
patients were admitted for FJ injection (14) or RFA (6) and positioned in the prone position on the fluoroscopic table.
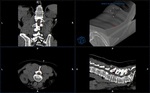
The CT/MRI Dicom series were then loaded into the ultrasound unit (Fig 3).
Needle guiding system,
tracking bracket,
and magnetic sensors were fastened to the ultrasound probe.
The reference tool was fixed again in the sacral region (in the same position as per the MRI and CT scan) so that patient and probe position were co-registered with actual CT or MRI scan.
OmniTRAX skin marker (CIVCO,
USA) for MRI and CT on the patient’s body allowed basic automatic registration with a single click (Fig 4).
This active patient tracking system consists of the disposable locating device (green for CT and pink for MRI) and a reusable general purpose electromagnetic sensor.
Compatible with Virtual Navigator,
the technology allows physicians to register patient anatomy quickly and accurately,
thereby eliminating tedious manual image registration (Fig 5).
Where necessary,
co-registration was manually fine-tuned with internal anatomical markers.
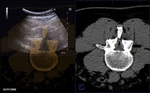
The ultrasound probe was positioned in order to acquire a sagittal view of the spinous process (Fig 6).
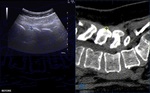
At this stage it was possible to apply manual fine-tuning in order to properly match the ultrasound with the second imaging modality (Fig 7).
Next,
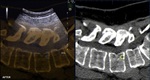
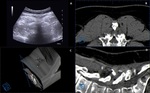
the axial scan was used further evaluate the anatomy also with ultrasound (Fig 8).
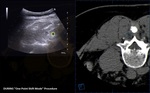
Axial scan with one-point shift mode synchronization (if needed) and the overlap feature additionally guarantee perfect anatomical correspondence between ultrasound and MRI/CT (Fig 9,10).
Multiview layout may additionally be used to increase the level of confidence of the operators before needle insertions (Fig 11).
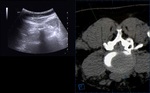
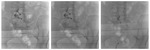
Needle for FJ Injection or Radio Frequency Ablation (RF) was then positioned under ultrasound-CT or ultrasound-MRI fusion guidance (Fig 12,13,14).
Before performing the treatment,
the correct position of the needle was checked by means of fluoroscopy (Fig 15) or CT scan.
Bone pain targeted neurotomy management procedures were performed with 22G RF nitinol probes (Kimberly Clark USA).
Facet joint injection was performed with a 21G spinal needle after local disinfection using a 1-3 ml syringe with low-solubility steroid (0.5 ml) and local anesthetic (0.5 ml).