Vascular closure devices are in their third decade of development for diagnostic and interventional cardiovascular procedures.
The adoption of that kind of devices has ocurred because a clear technological feat: vascular closure devices reliably shortens the time of hemostasis (elapsed time between sheath removal and first observed hemostasis) compared with manual compression and thus allow earlier patient ambulation.
In front of another approaches,
femoral vascular closure can be performed inmediately at the end of the procedure regarless of anticoagulation status: procedural success is expected in more than 95% of patients,
time to hemostasis is generally less than 5 minutes and for many patients can allow improved patient satisfaction and confort related to the avoidance of prolonged sheath insertion and manual compression.
We made a retrospective,
observational and descriptive study with all patients treated in our center for the last 4 years by percutaneous closure devices in femoral acceses during an EVAR intervention.
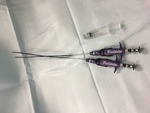
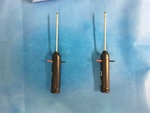
One hundred percutaneous closures in forty-two patients was performed using Perclose Proglide vascular device during the repair of 42 abdominal aortic aneurysms.
Information was taken by medical history and doctors notes.
We studied the technnical success and early complications index due to this device in the first 48h.
The Perclose Proglide system is indicated for the percutaneous delivery of suture for closing the common femoral artery access site of patients who have undergone diagnostic or interventional catheterization procedures using 5F to 21F sheats.
For sheath sizes greater than 8F,
at least two devices and the pre-close technique are required.
There are no contraindications to the use of this advice but there are some warnings: we can not use that device if the puncture site is located above the most inferior border of the inferior epigastric artery (IEA) and/or above the inguinal ligament based upon bony landmarks,
since such a puncture site may result in a retroperitoneal hematoma.
Do not use the Preclose Proglide system if the puncture is through the posterior wall or if there are multiple punctures,
since such punctures may result in a hematoma or retroperitoneal bleed. The use of ultrasound to guide the puncture site is recommended.
If the puncture site is located in the superficial femoral artery or the profunda femoris artery or at the bifurcation of these vessels,
is not recommended neither,
since such puncture sites may result in a pseudoaneurysm,
intimal dissection ora n acute vessel closure (thrombosis of small artery lumen).
The identification of significant femoral arterial disease may allow selective use of manual compression in situations where implantation of an intravascular device may be associated with an increased risk of complications.
Also,
with this device,
you have to use a single wall puncture technique,
and do not deploy the system at an angle greater than 45 degrees as this may cause a cuff miss.
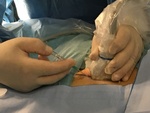
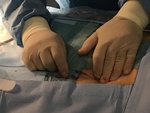
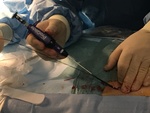
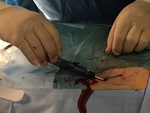
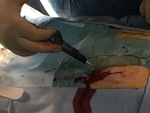
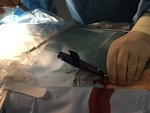
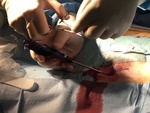
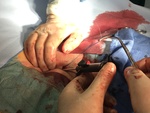
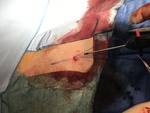
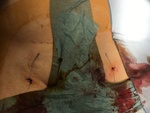
All the interventions were performed by the same person and the percutaneous closure procedure was performed according to the indications of the commercial house in all cases (Fig 1 and 2):
- Puncture the anterior wall of the common femoral artery at an angle of approximately 45 degrees.
Avoid side wall or posterior wall femoral artery punctures.
- Angiographically verify that the puncture is on the anterior wall of the common femoral artery.
The puncture should be proximal to the bifurcation of the superficial femoral artery and the profunda femoris branch and distal to the inferior margin of the inferior epigastric artery.
- Due the diagnostic or interventional procedure.
- Place a 0.038” (or smaller) guidewire through the procedural (or introducer) sheath.
Remove the procedural sheath while applying pressure on the groin to maintain hemostasis.
Fig.
4.
- Backload the device over the guidewire until the guide wire exit port of the device sheath is just above the skin line.
Remove the guidewire before the exit port crosses the skin line.
Fig 5.
- Gently pull the device back to position the foot against the arterial wall.
If proper position of the foot has been achieved,
tactile sensation will be felt and blood marking will cease or be significantly reduced to a slight drip.
If marking does not stop or significantly change,
evaluate the angiogram for femoral artery size,
calcium deposits,
tortuosity,
disease and for location of the puncture (ensure footplate is not in bifurcation or side branch).
Reposition the device to stop blood marking or reinsert the wire,
remove the device to hold manual compression or insert a new sheath.
Fig 7.
- While maintaining device position,
stabilize the device with your free hand (the one not used to deploy the device) to maintain the gentle retraction and to ensure the device does not twist or move forward during deployment.
Use your other hand to deploy needles by pushing on the plunger assembly until you visually confirm that the collar of the plunger makes contact with the proximal end of the body.
Do not use excessive force or repeatedly push the plunger assembly.
After visually confirming contact with the body of the device only one time,
this step is complete.
Fig 8.
- Using your thumb as a fulcrum on the handle,
gently disengage the needles by pulling the plunger assembly back and completely remove the plunger and needles from the body of the device.
One suture limb will be attached to the anterior needle.
The posterior needle will be free of suture.
Pull back on the plunger until the suture is taut,
which confirms that all the suture as been fully retracted from the body of the device.
Fig 9.
- Do not attempt to redeploy the needles if the suture limb is not attached to the anterior needle.
Reinsert the guidewire,
and remove the device over the wire.
Insert a new Perclose ProGlide SMC device to complete the procedure.
- Use the QuickCut suture-trimming mechanism located on the body of the device to cut the suture from the anterior needle distal of the link.
Use of a new,
sterile scalpel or scissors is optional.
- Relax the device and then return the foot to its original closed position by pushing the lever down to the body of the device.
Do not attempt to remove the device without closing the lever.
- Deliberately retract the Perclose ProGlide SMC device to release the suture knot.
Continue to gently withdraw the device until the guide wire exit port is visible above the skin line.
- Slightly rotate the device until you can see the two suture limbs in the bend of the distal guide.
Grasp the suture adjacent to the device sheath and pull the suture ends through the distal end of the proximal guide.
The rail suture limb is blue and is the longer of the two suture limbs.
This rail suture limb will be used to advance the knot.
The shorter,
non-rail suture limb is white tipped and will be used to lock the knot.
- Continue with Knot Advancement.
There should be sufficient guidewire exposed out of the guide wire exit port before removing the device.
Wrap the rail limb (long blue limb) of suture around your left index finger,
low close to skin level.
- Remove the Perclose ProGlide SMC device with the right hand,
while maintaining an adequate length of guidewire inside the artery.
This allows placement of another Perclose ProGlide SMC device or a sheath in the event that hemostasis is not obtained.
- While removing the device with the right hand,
simultaneously advance the knot to the arteriotomy by applying slow,
consistent increasing tension to the rail suture limb,
keeping the suture coaxial to the tissue tract.
(During 5-8F procedures,
do not advance the knot with the Snared Knot Pusher or the Suture Trimmer until the wire has been completely removed from the tissue track).
Fig 11.
- Assess the site for adequate hemostasis.
If bleeding is controlled,
the operator should then remove the guidewire.
Next,
use the Snared Knot Pusher or Suture Trimmer,
to advance and tighten the knot until complete closure is achieved.
Confirm the security of the knot by having the patient cough and/or bend his/her leg (Active testing for hemostasis is only for 5F-8F sheaths.
For 8.5F-21F sheath closures,
active confirmation should not be performed; only visual confirmation of hemostasis should be employed.).
Patients may be able to move freely in bed without head of bed or leg restrictions if the close is successful.
Fig 12.
- If the wire is still in place and suture breakage occurs during knot advancement,
or if hemostasis is not achieved,
another Perclose ProGlide SMC device can be used to complete the procedure or a sheath can be inserted.
Either remove the broken suture limbs or cut the suture limbs close to the knot .
- Care should be taken to avoid excessive force if the insertion of another Perclose ProGlide SMC device or introducer sheath is required.
To avoid resistance,
use an introducer sheath small enough to avoid undue force.
- If hemostasis cannot be achieved after the wire is removed,
apply manual compression.
Fig 12.