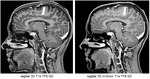
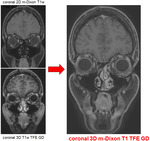
PROCEDURE DETAILS
All MR images have been obtained on the 1.5 T Ingenia Philips scanner with sequence parameters shown in table 1.
The postcontrast 3D T1w m-Dixon TFE sequence has a stable and homogeneous fat suppression achieved by the help of the m-Dixon technique (5).
A reduction of movement artefacts is possible by the use of 4 numbers of acquisitions (NSA).
A reduction of the susceptibility artefacts is obtained by using a high receiver bandwidth.
Table 1: Parameters used on 1.5 T MR Ingenia Philips ® scanner
|
Parameters
on 1.5 T MR
|
Postcontrast sag 3D T1w TFE
|
Postcontrast sag 3D m-Dixon T1w TFE
|
Postcontrast 2D m-Dixon T1w TSE (transverse,
coronal)
|
|
Field of view (FOV)
|
240 x 240mm2
|
250 x 250mm2
|
180 x 180mm2
|
|
acquired voxel size in mm3
|
1.0 x 1.0 x 1.0
|
1.0 x 1.0 x 1.0
|
0.5 x 0.7 x 3.0
|
|
reconstructed voxel size in mm3
|
0.8 x 0.8 x 1.0
|
0.5 x 0.5 x 0.5
|
0.5 x 0.5 x 3.0
|
|
number of slices
|
160
|
400
|
36
|
|
repetition time (TR)
|
7.6 ms
|
6.7 ms
|
676 ms
|
|
echo time (TE)
|
3.5 ms
|
4.1 ms
|
9.5 ms
|
|
flip angle
|
8°
|
10°
|
90°
|
|
prepulse
|
inversion
|
-
|
-
|
|
turbofactor
|
239
|
15
|
5
|
|
profile order
|
linear
|
low-high,
radial turbodirection
|
asymmetric
|
|
fat suppression
|
no
|
m-Dixon
|
m-Dixon
|
|
sense factor
|
P reductions = 1
S reduction = 2
|
P reduction = 2
S reduction = 2.2
|
P reduction = 1.4
|
|
number of acquisitions (NSA)
|
1
|
4
|
1.4
|
|
receiver bandwidth
|
217 Hz/pixel
|
542 Hz/pixel
|
359 Hz/pixel
|
|
acquisition time
|
05:37 min
|
05:36 min
|
04:24 min
|
MRI FINDINGS IN DIFFERENT PATHOLOGIC ENTITIES
It has to be stressed that the diagnostic reliability and the image quality of the new postcontrast 3D m-Dixon T1w TFE sequence has been exceptionally good for all pathologies examined.
The postcontrast 3D T1w TFE sequence as well as the additional postcontrast 2D m-Dixon T1w TSE sequences in at least one plane of section did not offer any real advantage in comparison with the new sequence.
1.Orbit
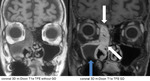
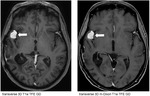
Metastases to the dura and leptomeninx (white arrow) and to the extraconal space in the orbit between 12 and 3 o`clock (double white arrow) are presented in Fig.
1 in a female patient with metastatic breast carcinoma.
The extraconal orbital metastasis infiltrates the lacrimal gland and the superior rectus muscle and the levator palpebrae superioris muscle and the surrounding fatty tissue.
An additional scleral metastasis adjacent to the optic nerve head is visible as a contrast enhancing nodule (white arrow on Fig.
2).
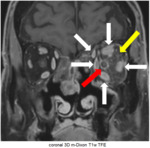
In orbital inflammatory disease (Fig.
3) a unilateral thickening and strong enhancement of all extraocular muscles (white arrows) and of the optic nerve sheath (red arrow) together with streaky enhancement of the retrobulbar intra- and extraconal fatty tissue (yellow arrow) is present on the left side.
2.Superficial temporal artery and giant cell arteritis
In giant cell arteritis a transmural inflammation of the intima,
media and adventitia of affected arteries is present.
The mural hyperplasia results in arterial luminal narrowing.
The disease involves the superficial temporal artery but affects also the ophthalmic,
the occipital,
vertebral and posterior ciliary arteries.
Possible involvement of the aorta,
the carotid,
subclavian and ilial arteries is known.
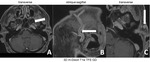
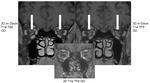
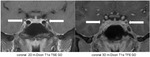
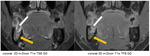
The focal segmental or diffuse thickening and contrast enhancement of the vessel wall along the superficial temporal artery can be detected on the postcontrast 3D m-Dixon T1 TFE sequence in Fig.4.
If oblique sagittal reconstructions are done (white line marked by white arrow in Fig.
4A) the diffuse contrast enhancement of the vessel wall of the superficial temporal artery (Fig.
4B and 4C) is nicely demonstrated labelled by white arrows.
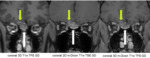
Perineuritis of the optic nerve sheath in giant cell arteritis is an additional common finding as demonstrated in Fig.
5,
where the optic nerve sheath shows a bilateral circular contrast enhancement (white arrows).
The optic nerve sheath is not visible at all on the postcontrast 3D T1w TFE sequence.
3a.
Cavernous sinus,
cranial nerves and foramina: Normal anatomy
Along the lateral sinus wall the cavernous sinus contains from superior to inferior the oculomotor nerve,
the trochlear nerve,
the ophthalmic nerve and the maxillary nerve.
The abducens nerve does not run within the lateral wall of the cavernous sinus but it passes through the middle of the cavernous sinus next to the internal carotid artery.
In Fig.
6 the oculomotor nerve (white arrows) is shown as hypointense non-enhancing dot within the uppermost part of the contrast enhancing cavernous sinus.
The trigeminal nerve has three divisions,
namely the ophthalmic (V1) nerve,
the maxillary (V2) nerve and mandibular (V3) nerve exiting from the trigeminal ganglion in Meckel`s cave.
The Meckel`s cave or trigeminal cave is a dura mater pouch containing the trigeminal ganglion surrounded by cerebrospinal fluid.
The mandibular nerve leaves the skull base through the foramen ovale and the maxillary nerve through the foramen rotundum.
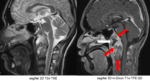
Fig.
7 depicts the normal fluid filled and hypointense Meckel`s cave (white arrows) situated at the postero-lateral aspect of the cavernous sinus.
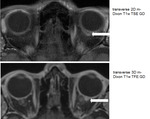
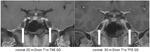
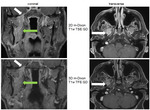
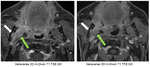
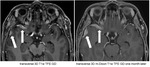
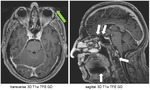
In Fig.
8 the normal maxillary nerve (white arrows) is visible as a punctate dot within the foramen rotundum on coronal images.
On the postcontrast 3D T1w TFE GD sequence the nerve is not reliably depicted due to susceptibility artefacts (red arrows).
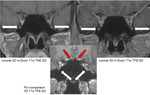
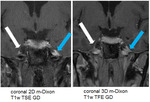
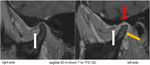
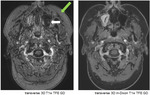
In Fig.
9 the normal mandibular nerve (white arrows) can be demonstrated within the oval foramen both on postcontrast coronal 2D m-Dixon T1w TSE as well as on postcontrast coronal 3D m-Dixon T1w TFE,
but cannot be reliably appreciated on the postcontrast 3D T1w TFE sequence due to severe susceptibility artefacts (red arrows).
3b.
Cavernous sinus,
cranial nerves and foramina: Pathologic lesions
A dural based meningioma (blue arrows) within the Meckel`s cave is present in Fig.
10.
The normal contralateral hypointense but dura lined Meckel`s cave is depicted with white arrows.
In Fig.
11 a perineural tumorous infiltration along the thickened and contrast enhancing mandibular nerve within the oval foramen (white arrow) due to squamous cell carcinoma is visible.
The pterygoid muscles (green arrows) show contrast enhancement due to denervation.
4.
Mandible and Masticator Space
The normal mandible presents with hypointense cortical bone and less hypointense cancellous bone.
The normal inferior alveolar nerve (Fig.
12) can be seen as hyperintense linear structure passing through the cancellous bone within the mandibular canal from the mandibular foramen to the mental foramen (white arrows).
On the postcontrast 3D T1w TFE sequence the nerve is not reliably depicted (Fig.
12).
In Fig.
13 a postoperative defect in the mandible involving both cortical and cancellous bone after extraction of a molar tooth is visible (white arrow).
Reactive osseous changes in the adjacent surrounding cancellous bone are present (orange arrows).
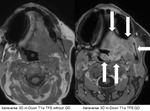
A tumorous perineural infiltration due to squamous cell carcinoma of the alveolar crest along the inferior alveolar nerve is depicted in Fig.
14.
The inferior alveolar nerve within the mandibular foramen is thickened and contrast enhancing (white arrows).
Denervation and possible tumorous infiltration of the pterygoid muscles demonstrated by contrast enhancement is depicted with green arrows.
A widespread left sided squamous cell carcinoma infiltrating the tongue,
the base of the tongue,
the retromolar space,
the tonsilla palatina,
the soft palate,
the masticator space and the mandible with destruction of cortical and cancellous bone is depicted in Fig.
15.
The tumourous extent is marked by white arrows.
The 3D m-Dixon T1w TFE with and without Gadolinium reliably depicts the tumourous extent.
5.Temporomandibular joint
In elderly patients complaints about pain and clicking sounds during chewing and mouth opening are quite common.
Additionally restrictions in mouth opening may be present as well.
In Fig.
16 bilateral anterior disc luxation (white arrows) is present together with deformity and contrast enhancement of the mandibular head (orange arrow),
contrast enhancement of the synovia (red arrow) and a shallow mandibular fossa on the left side and contrast enhancement of the cancellous bone of the mandibular head (orange arrow) due to congenital malformations of the temporomandibular joint left side.
6.Paranasal sinuses and adjacent osseous structures
Acute sinusitis with thickening and contrast enhancement of the mucous membrane (white arrows) and with non-enhancing fluid (blue arrow) within the maxillary,
ethmoid and frontal sinus right side is shown on the postcontrast 3D m-Dixon T1 TFE sequence in Fig.
17.
In Fig.
18 an intraosseous menigioma (white arrow) with dural tail sign (green arrow) and extension into the ethmoid sinus bilaterally can be nicely depicted on the postcontrast 3D m-Dixon T1 TFE sequence.
There are no movement or susceptibility artefacts present.
7.
Dural pathologies
Dural metastases are common both in prostate cancer as well as in breast cancer.
Fig.
19 demonstrates contrast enhancing dural metastases of breast carcinoma along the sphenoid wing and along the temporal bone on the right side,
marked with white arrows both on postcontrast 3D T1w TFE sequence as well as on postcontrast 3D m-Dixon T1w TFE sequence.
8.
Leptomeningeal pathologies
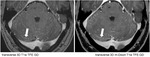
In neurosarcoidosis multiple leptomeningeal confluent noduli can be detected as contrast enhancing nodules within the cerebellar fissures in Fig.
20.
The white arrow marks a line of confluent noduli.
The detection of these contrast enhancing noduli is identical on postcontrast 3D T1w TFE or on 3D m-Dixon T1w TFE images.
9.
Pathologies of the Brain Parenchyma
Intraparenchymal metastases are depicted on postcontrast 3D T1w TFE or on postcontrast 3D m-Dixon T1w TFE images as shown in Fig.
21 in a patient with a solitary parenchymal metastasis due to breast carcinoma (white arrows).
10.
Pathologies of the Neurocranium
Infectious involvement and contrast enhancement of clivus and both vertebral bodies atlas and axis (red arrows) with severe contrast enhancement on postcontrast 3D m-Dixon T1 TFE and with T2w hyperintensity together with a soft tissue abscess with central necrosis (white arrow) due to tuberculosis infection is shown in Fig.
22.
Advantages and disadvantages of the new postcontrast 3D m-Dixon T1w TFE sequence
The postcontrast 3D m-Dixon T1w TFE sequence is a stable sequence with considerably few susceptibility artefacts due to high receiver bandwidth,
usually without movement artefacts due to multiple NSA and with a homogeneous fat suppression in the head and neck region due to the m-Dixon technique as shown in table 2 and in Fig.
23 to 24 if compared to the postcontrast 3D T1w TFE sequence.
Table 2
|
|
3D m-Dixon T1w TFE GD
|
3D T1w TFE GD
|
|
susceptibility artefacts
|
minimal in the head and neck
|
severe in the head and neck
|
|
movement artefacts
|
rare
|
often in head and neck
|
|
homogeneous
fat supression
|
yes
|
no fat supression
|
|
contrast between gray and white matter
|
sufficient
|
very good
|
|
multiplanar reconstructions
|
possible
|
possible
|
|
acquisition time in min.
|
5:36 min.
|
05:37 min.
|
Fig.
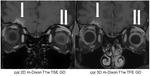
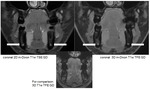
23 demonstrates disturbing and perturbing movement artefacts (green arrow) and susceptibility artefacts (white arrows) on the postcontrast 3D T1w TFE sequence.
Fig.
24 shows that the postcontrast 3D m-Dixon T1w TFE sequence is very stable without movement (green arrow) and susceptibility artefacts (white arrow) compared to the postcontrast 3D T1w TFE sequence in the same patient which presents with disturbing artefacts.
Both sequences have been scanned one after the other.
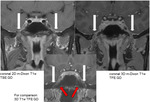
The only disadvantage of the postcontrast 3D m-Dixon T1w TFE sequence is the slightly reduced image contrast between gray and white matter in the brain parenchyma compared to the postcontrast 3D T1w TFE sequence.
This is obvious in Fig.
25 marked by white arrows.
However this disadvantage has no clinical importance because the sequence is routinely used for detection of contrast enhancing lesions and not for the analysis of the gray-white matter contrast.
In comparison with the postcontrast 2D m-Dixon T1w TSE sequence the postcontrast 3D m-Dixon T1w TFE has no disadvantage but only advantages for it allows multiplanar reconstructions in very good image quality without obvious image noise.
This is shown in table 3.
Table 3
|
|
3D m-Dixon T1w TFE GD
|
2D m-Dixon T1w TSE GD
|
|
technique
|
gradient echo sequence
|
spin echo sequence
|
|
susceptibility artefacts
|
minimal
|
minimal
|
|
homogeneous
fat supression
|
yes
|
yes
|
|
signal to noise SNR
|
low
|
high
|
|
acquisition time in min.
|
5:36 min.
|
05:37 min.
|
|
multiplanar reconstructions
|
yes
|
no
|