Type:
Educational Exhibit
Keywords:
Education, CT, MR, Pancreas, Gastrointestinal tract, Biliary Tract / Gallbladder, Cholangiography, Artifacts, Calcifications / Calculi, MR-Cholangiography
Authors:
H. D. Peiris1, S. McGee2, D. Sheppard3, M. S. B. T. Wills3; 1Southampton/UK, 2Salisbury, Wiltshire/UK, 3Salisbury/UK
DOI:
10.1594/ecr2018/C-0610
Findings and procedure details
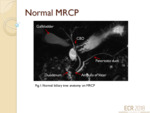
NORMAL MRCP
The biliary tree,
gallbladder,
common bile duct and pancreatic duct can be visualised (fig.1).
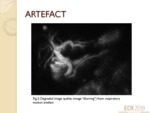
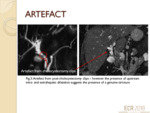
ARTEFACTS
Respiratory motion artefact degrades resolution and results in image “blurring” that poses significant difficulty in assessment of the biliary tree (fig.2).
Artefact from surgical clips post-cholecystectomy (fig.3) poses a diagnostic challenge,
giving the impression of signal void or perceived luminal narrowing.
These can be mitigated by identifying other ancillary features of biliary obstruction such as the presence or absence of intra/extrahepatic ductal dilation.
ANATOMICAL VARIANTS
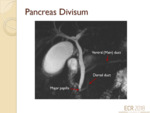
Pancreas divisum2 (fig.4)
- A frequently encountered pancreatic anatomical variant which occurs as a result of the dorsal and ventral pancreatic ducts failing to fuse.
- Ventral (larger) duct drains into the minor papilla and the dorsal (smaller duct) drains into the major papilla.
- Recognition of this variant is important because of its association with acute and chronic pancreatitis.
BENIGN DISEASE
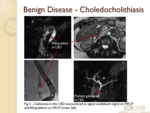
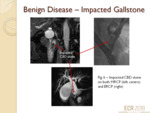
Choledocholithiasis/(Gallstones in CBD) (fig.5,
fig.6)
- Presentation is often with right upper quadrant pain (“biliary colic”),
with or without obstructive liver function tests and CBD dilatation on ultrasound.
May also present as recurrent,
otherwise-unexplained cholangitis.
- Intraductal gallstones are evident as dependant areas of signal void/absent signal surrounded by high signal-intensity bile.
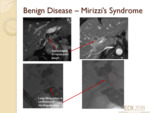
Mirrizi’s syndrome (fig.7)
- Impaction of large gallstone/multiple gallstones in Hartmann’s pouch/cystic duct with resultant acute/chronic cholecystitis and subsequent fibrosis and inflammation,
leading to extrinsic compression of the common bile duct.
- Long/low-insertion of cystic duct are predisposing factors
- Diagnostic accuracy is 50% with MRCP3,
however the risk of complications with ERCP is mitigated.
MALIGNANT DISEASE
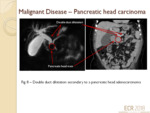
Pancreatic head adenocarcinoma (fig.8)
- An adenocarcinoma in the pancreatic head frequently causes obstruction of the pancreatic and common bile ducts.
- 75% show a “double duct” sign on MRCP1.
- MRCP is a useful initial investigation for patients presenting with painless obstructive jaundice,
but post-contrast CT imaging will subsequently be required for staging if a tumour is suspected.
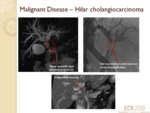
Cholangiocarcinoma (Bile duct tumour) (fig.9)
- A tumour of the bile duct which results in a stricture that manifests as an area of luminal narrowing or absent signal on MRCP,
with upstream biliary duct dilatation.
- May affect the CBD/common hepatic duct/biliary bifurcation (Klatskin tumour)/intra-hepatic duct(s).
- Other ancillary features include wall thickness >3mm,
and delayed enhancement of the tumour on post-contrast CT or MR imaging.
PANCREATIC CYSTIC LESIONS
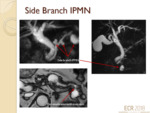
Sidebranch Intraductal Papillary Mucinous Neoplasm4 (IPMN) (fig.10)
- MRCP may be performed to assess a pancreatic cystic neoplasm e.g.
when incidentally discovered on CT.
Demonstrating a thin communication with the non-dilated main pancreatic duct confirms a diagnosis of a sidebranch IPMN.
- These are typically located in pancreatic head and neck.
- NB: dilatation of the main pancreatic duct would imply either a mixed or main-duct IPMN,
which has a higher malignant potential than a sidebranch IPMN.