This review illustrates typical and atypical cases of primary or secondary extranodal lymphoma using imaging techniques such as CT,
IRM with emphasis on imagistic key features of this disease.
This paper does not aim to be an exhaustive presentation of extranodal lymhoma.
This review mainly focuses on tricky cases of extranodal lymphoma.
Brain and spine
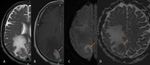
Cerebral lymphoma (Fig.2,
Fig.3)
Primary cerebral lymphoma represents 1-2% of all non-Hodgkin lymphomas and about 2-6% of all brain tumors [2].
Secondary cerebral lymphoma is a central nervous system spread of a lymphoma originating elsewhere in the body and,
unlike primary cerebral lymphoma,
it involves most commonly the leptomeninges.
Typical location of primary cerebral lymphoma is the supratentorial region,
in contact with ventricular and meningeal surfaces. Atypical locations include the brainstem,
pineal gland,
pituitary gland,
cranial nerves,
and cavernous sinuses [2].
Imaging features
Cerebral lymphoma has a specific appearance on CT and MRI scan due to its high cellularity,
disruption of blood brain barrier and predilection for periventricular and superficial regions.
On non-enhanced CT scan,
primary cerebral lymphoma appears as a solitary hyperattenuating parenchimal mass (due to its high cellularity) surrounded by moderate perilesional edema (Fig.2 A).
Secondary lymphoma most often appears as leptomeningeal spread.
On MRI scan,
cerebral lymphoma has usually iso-hypointensity signal on both T1 and T2 sequences and diffusion restriction.
Hemorrhage and calcifications are rare.
After contrast enhancement,
there is usually intense,
homogeneous enhancement (Fig.3).
However,
in immunosuppressed patients,
a ring-like enhancement may be observed.
In contrast to other malignant tumor brains,
cerebral lymphoma does not have necrosis.
Differential diagnosis:
-cerebral toxoplasmosis,
butterfly glioma,
neurosarcoidosis,
metastatic disease,
meningioma (Fig.2 B,C)
Epidural lymphoma (Fig.4)
Epidural lymphomas represents about 0,1- 6,5 % of all lymphomas and 9% of all spinal epidural tumors [3].
Lymphomatous spinal masses are classified according to compartment: extradural,
intradural extramedullary and intradural intramedullary.
Imaging features
On MRI,
epidural lymphomas usually are isointense on T1 and iso- to hyperintense on T2 sequences,
with contrast enhancement.
Typical location for epidural lymphoma is in the thoracic spine and,
within the spinal canal,
it is dorsally rather than ventrally [3].
It generally extends over several vertebra and sometimes,
it may affect the nerve foramina and mimic a nerve sheath tumor.
Differential diagnosis:
-metastasis,
abscess,
vascular malformation,
lipoma,
arachnoid cyst,
hematoma,
Hirayama disease
Thorax
Lung lymphoma (Fig.5,
Fig.6)
Pulmonary involvement occurs more often in Hodgkin’s disease than non-Hodgkin lymphoma.
In Hodgkin disease,
the lung is most often secondary involved by widespread mediastinal disease,
while in non-Hodgkin disease,
about 50% of cases develop a thoracic manifestation [4].
Primary pulmonary lymphoma is 0,4 % of all lymphomas [5].
Imaging features
There is no specific pattern disease in lung lymphoma.
CT findings vary from milliary or discrete nodules to ground-glass opacities and ill-defined areas of consolidation with or without cavitation or air bronchogram (Fig.5).
Another pattern of lung lymphoma,
less frequently,
is peribronchial and/or perivascular thickening (Fig.6).
Differential diagnosis:
-primary lung carcinoma,
metastatic disease,
granulomatous disease,
pneumonia,
round atelectasis
Pleural lymphoma
Pleural lymphoma represents < 0,5% of non-Hodgkin lymphoma and it may appear as diffuse pleural thickening,
plaques or nodules [6].
These lesions can arise anywhere on the pleural surface and are usually accompanied by pleural fluid.
Differential diagnosis:
-mesothelioma,
pleural carcinomatosis,
solitary fibrous tumor of the pleura
Abdomen
Hepatic lymphoma (Fig.7)
Secondary involvement of the liver in advanced stages of lymphoma is quite common.
Hepatic lymphoma is present in the initial stage of 15% of non-Hodgkin lymphoma patients and in 10% of Hodgkin disease patients [7].
Primary hepatic lymphoma is rare; it accounts for < 1% of all extranodal lymphomas [8].
Imaging features
Multifocal hepatic lesions
These lesions vary in size from 1-5 cm diameter,
are usually hypodense on non-enhanced CT and,
after enhancement,
they demonstrate most often no or mild enhancement.
Occasionally,
the lesions show patchy or ring enhancement.
On MRI,
the lesions are iso-hypointese on T1,
moderately hyperintense on T2 and show restricted diffusion.
The main differential diagnosis is with metastatic disease.
Diffuse infiltration of the liver
Diffuse infiltration of the liver is the trickiest appearance of hepatic lymphoma because it may have the same attenuation of normal hepatic parenchyma and may be mistaken for parenchymal disease or fatty infiltration [7],
[8].
Solitary hepatic mass (Fig.7)
Solitary hepatic mass is more often a manifestation of primary hepatic lymphoma than secondary lymphoma.
It may range from 1 cm to 10 cm in dimension and is homogeneous and hypodense on non-contrast enhanced CT.
After contrast enhancement,
most often primary hepatic lymphoma shows no or mild enhancement.
One important feature in the diagnosis is the fact that hepatic lymphoma has an infiltrative pattern,
meaning that it encases the hepatic vessels without invading them.
On MRI,
hepatic lymphoma is usually iso- or hypointense on T1,
hyperintense on T2 and has restricted diffusion.
Differential diagnosis:
-metastatic disease (Fig.7),
focal steatosis,
hypovascular hepatocellular carcinoma
Pancreatic lymphoma (Fig.8)
Primary pancreatic lymphoma appears in < 2% of extranodal non-Hodgkin lymphoma patients,
while secondary pancreatic lymphoma appears in more than 30% of non-Hodgkin lymphoma patients [9].
Two morphologic patterns of pancreatic lymphoma have been described: a focal,
well-defined pancreatic mass form and diffuse enlargement of the gland.
Imaging features
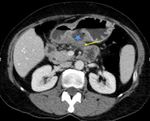
Focal pancreatic mass (Fig.8)
This form of pancreatic lymphoma can appear anywhere in the gland and can easily be mistaken for ductal adenocarcinoma especially when pancreatic and common bile duct are dilated [9],
[10].
However,
pancreatic lymphoma causes only mild pancreatic duct dilatation and atrophy.
Diffuse enlargement of pancreas
This diffuse infiltrating pattern may be misinterpreted as acute pancreatitis; however,
even though serum amylase may be elevated,
in pancreatic lymphoma the abdominal pain is usually absent.
Typical findings in pancreatic lymphoma:
-it may occur anywhere in the gland but more often in the pancreatic head
-on non-enhanced CT,
pancreatic lymphoma is slightly hypodense in comparison to normal pancreatic parenchyma; after contrast administration,
the enhancement is poor but homogeneous
-pancreatic lymphoma causes relatively little pancreatic and common bile duct dilatation and little atrophy of the pancreas
-the vessels may be enveloped by pancreatic lymphoma but there is no vascular invasion
-calcification and necrosis within tumor are rare before treatment
-enlarged lymph nodes below renal pedicle
Differential diagnosis
-ductal adenocarcinoma: has a more heterogeneous enhancement and a significant dilatation of the pancreatic duct; vascular invasion and peripancreatic lymphadenopathy are common findings; lymphadenopathy below the renal pedicle is uncommon for ductal adenocarcinoma (Fig.9)
-autoimmune pancreatitis: has persistent or delayed enhancement; elevation of Ig4,
involvement of other organs.
-pancreatitis: usually it is associated with clinical signs of pancreatitis.
Gastric lymphoma (Fig.10,
Fig.11,
Fig.12,
Fig.13)
The stomach is the first site of involvement of primary lymphoma.
However,
of all gastric malignancies,
gastric lymphoma represents about 3-5% [4].
Various patterns of gastric lymphoma have been described such as diffuse infiltration,
focal polypoid,
ulcerative form etc.
Of these,
the most commonly observed is the infiltrative pattern with thickened gastric wall [10].
Imaging features
Diffuse infiltration pattern (Fig.11 A,
Fig.12)
Diffuse infiltration pattern appears as an extensive wall thickening with mild enhancement of the lesion.
There is diffuse thickening of the segment involved because lymphoma extends along the submucosa and muscularis propria,
unlike adenocarcinoma,
which arises from mucosa [10]; this is the reason why gastric lymphoma may be missed at endoscopy.
Focal polypoid pattern
Focal polypoid pattern may present as multiple polyp-like masses with the surrounding tissue thickened or normal.
Usually,
the lesions are homogenous and hypoenhancing.
When large,
however,
they may appear heterogenous because of internal hemorrhage and ischemia.
Ulcerative pattern (Fig.13)
The ulcerative pattern may determine an abnormal bulge in the gastric contour which fills with contrast.
DBCL often appear as a large tumor with areas of ulceration [11],
[12].
Typical findings in gastric lymphoma:
-markedly and extensive gastric wall thickening with preservation of contour and perigastric fat plane
-bulky regional or widespread lymphadenopathy
-adenopathy below the renal pedicle
-transpiloric spread into duodenum
-the lumen is preserved even with marked gastric wall infiltration because lymphomas usually do not have a desmoplastic reaction [10],
[12]
Differential diagnosis
-gastric adenocarcinoma: focal wall thickening with vivid enhancement; infiltration of the surrounding fat; obstruction due to endolumenal narrowing; less bulky adenopathy (Fig.11 B)
-gastrointestinal tumor
-metastatic disease from melanoma
-infectious/inflammatory non-neoplastic entities
Intestinal lymphoma (Fig.14)
Lymphoma is the most common malignancy of the small bowel.
Colonic lymphomas,
instead,
are a rare entity and tend to arise in the cecum and rectum [13].
Imaging features
Infiltrative form
Symmetric or asymmetric intestinal wall infiltration with minimal enhancement is the most common CT finding in intestinal lymphoma [12],
[13].
Aneurysmal dilatation on the antimesenteric border may be seen due to the replacement of autonomic nerve plexus by lymphoma.
Polypoid form
Another pattern described in intestinal lymphoma is the polypoid form.
The polyps may range from several millimeters to several centimeters in dimensions and may be solitary or innumerable,
like in mantle cell lymphoma (lymphomatous polyposis).
Another important imagistic feature is that these lesions may ulcerate,
giving the appearance of „target” lesion or „bull’s eye” lesion.
Complications
-perforation: uncommon,
it appears usually after chemo/radiotherapy
-obstruction: uncommon because lymphoma does not usually have a desmoplastic reaction; however,
obstruction may be the initial presentation of an intestinal lymphoma [14].
Intestinal lymphoma should be considered in the differential diagnosis of obstruction along with other causes like hernias,
adhesions,
bezoars etc.
-intussception: uncommon in adults; when present,
intussception usually indicates nonendemic Burkitt lymphoma which typically affects the ileocecal region (Fig.14,
A)
-ulceration
Differential diagnosis:
-diffuse thickening: infection or inflammatory conditions such as Clostridium difficile infection,
Chron’s disease,
edema from low protein states,
portal hypertension with cirrhosis,
low-flow ischemia.
-focal thickening: adenocarcinoma (Fig.14,
B)
Splenic lymphoma (Fig.15,
Fig.16)
Splenic lymphoma is most often a manifestation of systemic lymphoma and is present in the initial stage of 30-40% of patients with Hodgkin disease and in 10-40% of patients with non-Hodgkin lymphoma [15]. In Hodgkin disease,
spleen involvement is considered nodal,
while in non-Hodgkin lymphoma,
spleen involvement is considered extranodal disease.
Primary splenic lymphoma,
however,
is rare [16].
Imaging features
Diffuse infiltration pattern
Diffuse infiltration is the most common pattern of splenic lymphoma.
Splenomegaly is neither sensitive nor specific for splenic lymphoma.
However,
on late venous phase,
multiple,
small (< 1 cm),
ill-defined hypoenhancing lesions may become evident in the spleen.
Nodular pattern (Fig.15,
Fig.16 A)
Splenic lymphoma may also present as a solitary mass or as multiple ill-defined,
hypoenhancing nodules larger than 1 cm.
The enhancement of these lesions is homogenous and hypoattenuating compared to normal splenic parenchyma.
Differential diagnosis:
-lymphangioma: hypoattenuating,
small,
ill-defined lesions with no enhancement (Fig.16 B,
C)
-fungal abscesses: multiple nodules with no adenopathies and with a heterogeneous pattern of enhancement
-angiosarcoma: may appear hyperattenuating on non-enhanced CT; on contrast-enhanced CT,
it may show a pattern of enhancement similar to hepatic hemangiomas
Renal lymphoma (Fig.17,
Fig.18)
Secondary renal involvement is quite common in non-Hodgkin lymphoma,
while primary renal lymphoma is rare because the kidneys do not contain lymphatic tissue [4].
Imaging features
Solitary or multiple masses
The most common pattern in renal lymphoma is represented by multiple masses,
usually bilateral.
Typically,
these lesions are 1-3 cm in diameter,
are homogenous and hypoattenuating in comparison with the normal renal parenchyma on contrast-enhanced CT.
After chemotherapy,
a more heterogeneous pattern may develop due to intralesional necrosis.
Calcification is rare [17]. Less frequently,
renal lymphoma appears as a solitary homogeneous,
hypovascular renal mass.
Diffuse infiltration
Diffuse infiltration presents with kidney enlargement with preservation of renal contour.
The pelvocaliceal system may be enveloped and deformed by the infiltrating tumor.
This type of renal lymphoma may result in poor renal function but usually sufficient so as the lymphoma remains clinically silent [7].
Perirenal disease (Fig.17 A,
B,
C)
Perirenal lymphoma manifests as a soft-tissue mass that envelop but does not invade the kidneys.
Other findings are encasement of renal sinus and thickening of Gerota fascia [1].
Contiguous retroperitoneal extension (Fig.18)
Contiguous retroperitoneal extension appears as a large retroperitoneal mass that encases the renal sinus.
Despite this,
the renal vessels are patent; however,
if renal collecting system is involved,
hydronephrosis may develop.
Atypical findings in renal lymphoma
Atypical findings are heterogeneous appearance with hemorrhage,
necrosis,
cystic transformation and calcifications [7].
Differential diagnosis:
-clear cell carcinoma: hyperintense on arterial phase,
heterogeneous,
vascular invasion
-urothelial cell carcinoma
-renal metastases
-pyelonephritis
-retroperitoneal fibrosis,
Erdheim Chester disease- in perirenal involvement (Fig.17 D,
E,
F)